commentary Commentary
Commentary: In Singapore’s bold plan to reopen, these are the hard-nosed decisions society must make
Vaccination, testing where it matters and social responsibility hold the keys to the new normal we desire, NUS Saw Swee Hock School of Public Health’s Dr Alex Cook and Dr Hsu Li Yang explain.

People wearing face masks cross a road amid the coronavirus disease (COVID-19) outbreak in Singapore on May 14, 2021. (Photo: REUTERS/Caroline Chia)
SINGAPORE: Something amazing happened this week. Half of all people in Singapore have now received at least one dose of a COVID-19 vaccine.
This ought to be an important milestone worth commending, indicating the start of a new phase in Singapore’s grand reopening.
Instead, we found ourselves eating in pairs and still working from home, with new clusters in malls, wet markets and HDB blocks.
READ: Commentary: Not easy but parents could use dining-in for two for needed couple time
VACCINATIONS REMAIN EFFECTIVE AGAINST NEW VARIANTS
SARS-CoV-2 has mutated as it spread around the globe. The latest variant of concern – the Delta variant – is now present in over 80 countries and has become the predominant variant in Singapore.
The Delta variant is thought to be at least twice as infectious than the original virus that emerged in Wuhan in late 2019. Just look at the new COVID-19 clusters that accompanied our cautious emergence from Phase Two (Heightened Alert) restrictions, including one at Bukit Merah and Redhill area that has ballooned to over 80 cases.
People are frustrated and afraid. Despite fighting a pandemic for over a year, the worry is that any further relaxation of already strict restrictions will result in a surge of infections that could rapidly escalate.
But we should not lose hope. For one, we are not losing in the race between vaccines and variants.
READ: COVID-19 task force shares broad plan for new normal with possible home recovery and travel
READ: Commentary: Some pain even as Singapore rises to the challenge of tighter COVID-19 measures
Current vaccines are somewhat less protective against infection by this Delta variant but remain very effective at preventing severe disease. Among Delta cases in the UK, hospitalisation rates were 96 per cent lower in those who had been vaccinated with the Pfizer-BioNTech vaccine than those still unvaccinated.
This means that while we can expect new variants to evolve, current vaccines, with modified booster shots, could continue to protect against serious disease and death in the next few years.
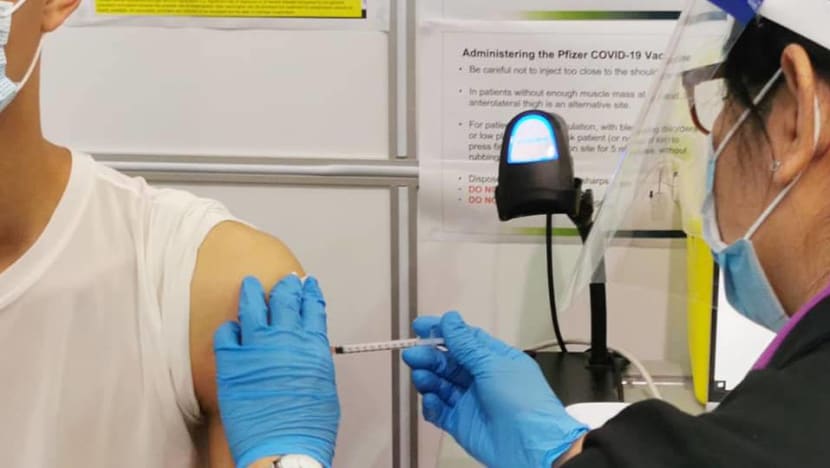
But current headline vaccination numbers belie troubling trends. Singapore’s multi-ministry task force has announced that more than 60 per cent of the elderly, who are at far higher risk of severe infection, have completed both doses, but this rate is not enough to “provide sufficient protection to the population” to permit scaling back the restrictions more rapidly.
READ: Commentary: Inaccurate public understanding of COVID-19 vaccine efficacy has implications for vaccination rates
MOVING TO NORMAL, DEFINING NEW GOALS
Does this mean that we can expect to move back to some sort of normalcy once we hit certain vaccination thresholds?
Perhaps, but we need to first define as a society our objectives and the price we are willing to pay to get there.
Certain goals are unachievable in the near term. SARS-CoV-2 is so transmissible, there is no prospect of it being eradicated worldwide.
Herd immunity, wherein the entire population is protected from a disease because a sufficiently large number are immune through vaccination or infection, is currently also impossible on a global scale.
It may even not be possible within Singapore, given the transmissibility of the Delta variant and that not everyone can, or wishes to, be vaccinated.
READ: Commentary: Variants versus vaccines is becoming the new COVID-19 race
READ: Commentary: Some pain even as Singapore rises to the challenge of tighter COVID-19 measures
Instead, our objective has to be to live with an endemic COVID-19. The conditions for doing so make that scenario possible.
In a few months’ time, everyone willing and able to be vaccinated will have done so.
Indeed, what that endemic state looks like will depend on how many people remain unvaccinated, how willing we are to allow cases to rise, and what restrictions and rules we are willing to stomach.

Once we relax measures, even with relatively high vaccine coverage, we can expect case counts to grow, like during influenza epidemics. This means some people, particularly elderly who did not get vaccinated, getting very sick and dying.
COVID-19 has claimed 35 lives in Singapore so far. What is an acceptable number of deaths from endemic COVID-19? Would we be willing to suffer the same number of annual deaths from COVID-19 as seasonal influenza? Or twice as many deaths?
Hundreds of people die of influenza-related causes in Singapore each year. Against influenza, most of us don’t take any special precautions, and we probably would not accept social distancing or mask wearing mandates to keep the common flu in check.
Setting expectations for how much worse we will tolerate from COVID-19 in the coming years will determine the level of vaccination needed to de-escalate measures.
READ: Commentary: Privacy in a pandemic — can I ask my GP if they’ve been vaccinated for COVID-19?
READ: Commentary: What’s behind no-shows in vaccination centres across Malaysia?
MAINTAINING HIGH VACCINE COVERAGE IS KEY
Ideally, vaccination coverage should be above 85 per cent of the total population, but there are limits because of ineligibility, adverse reactions to the initial dose and vaccine hesitancy.
Both Israel and the UK have managed to provide at least one dose of the COVID-19 vaccine to 80 per cent of their adult populations, achieving more than 60 per cent vaccination rate for their whole population. It would be disappointing if we cannot match that level.
The higher the vaccine coverage, the fewer long-term measures we would need to retain. Singapore should therefore put more effort on promoting vaccination, including offering concrete incentives once all age groups have had a chance to be vaccinated.
For instance, we may well be able to relax quarantine for returning travellers who have been vaccinated, though whether lower-effectiveness vaccines should be given equal treatment to Pfizer and Moderna is unclear since the risk of infection may be higher.

Getting vaccinated with the highest-efficacy vaccines is ideal to protect the individual and population, though for those who cannot take the mRNA vaccines, being vaccinated with an alternative is better than nothing at all.
More generally, government agencies will have to decide how to de-escalate their responses to COVID-19 cases and clusters, in tandem with achieving defined population vaccination thresholds.
In the transition to an endemic state, we could see more activities like events, weddings, movie theatres and eateries open up to accommodate more people with sufficient precautions.
READ: Commentary: COVID-19 unlikely to become a thing of the past anytime soon
WHAT A SUSTAINABLE NEW NORMAL LOOKS LIKE
We must also think about sustainability. While current responses have undoubtedly led to a much better situation in Singapore than many other countries, there is widespread fatigue in maintaining them.
Once we reach the endemic state, the quartet of isolating, testing, tracing and quarantining should be reviewed. What matters then is maintaining the severe cases and deaths at that tolerable level.
We need to apply a targeted approach that can rapidly tackle new cases instead of a blunt sledgehammer. Isolating all cases in hospital or a community facility regardless of severity has been very effective but would not be necessary once most people are protected. Such an approach would also be unfeasible if there are hundreds of mild cases a day.
READ: Commentary: We have to live with an endemic COVID-19. Here's what that could look like
READ: Commentary: Why we missed dining out in Singapore these few weeks
Responding swiftly to contain the spread is key but imposing stringent isolation and quarantine of contacts disincentivises many individuals with mild symptoms from seeking care and testing at primary care clinics, particularly with the widespread availability of home-testing kits. Costly healthcare and hospital resources are not needed in these instances.
But removing hospital-based isolation will require mild or asymptomatic COVID-19 cases to exercise responsibility and self-isolate at home and rest, so that they do not spread it to others.

Moving to this state to relax other safe management measures will require courage to shift away from obsessing over the daily numbers of cases, in the same we do not obsess over how many people catch the common flu pre-COVID-19.
Rather than the tail wagging the dog and policies changing in response to small fluctuations in the numbers of cases found, the Government too needs to de-emphasise the daily case counts.
Preparations for a future of endemic COVID-19 should be made with clear and public signposts of policies and interventions that can be tied to rates of national vaccination and necessary utilisation of hospital resources.
Although there will always be a degree of uncertainty owing to the ability of the virus to mutate further and “black swan” mass transmission events, these are relatively easily explained and accepted if good public communications and high trust in government agencies are maintained.
Alex R Cook in an associate professor who leads the Biostatistics and Modelling Domain and serves as the vice dean of research at the NUS Saw Swee Hock School of Public Health. Hsu Li Yang is the Infectious Diseases Programme Leader, vice dean of global health, and associate professor at the same school.














