Doctors from TTSH successfully treat 'unusual case' of blood clot in artery of COVID-19 patient
Adjunct Assistant Professor Glenn Tan and Adjunct Associate Professor Pua Uei, who were both involved in the surgery, holding a stent graft. (Photo: TTSH)
SINGAPORE: Doctors at Tan Tock Seng Hospital (TTSH) have successfully treated a COVID-19 patient who developed a blood clot in the aorta and was at risk of losing his toes or leg. The medical team later became the first in the world to publish research on the topic.
The patient, a 39-year-old Bangladeshi worker who was hospitalised in May, was “a bit of an unusual case”, with a blood clot in his thoracoabdominal aorta, said TTSH head of general surgery Adjunct Assistant Professor Glenn Tan on Tuesday (Oct 13).
The thoracoabdominal aorta extends from the chest to the abdomen and is part of the aorta, which is the biggest artery in the body.
Developing a blood clot in the aorta is unusual because the blood flow in the aorta is typically very high as it comes straight from the heart, said Dr Tan, who was the presiding surgeon.
Time was of the essence in treating the patient because the blood clot could move to other organs or to his legs, causing further complications. He could even lose his toes or leg from gangrene - which means he would be unable to continue working as a delivery driver in Singapore.
Opening up his chest to directly remove the clot from the aorta meant that everyone involved in the surgery would be exposed to COVID-19. This is partly why the team opted for a less invasive procedure, said Dr Tan.
In a two-hour operation on May 8, the doctors inserted an aortic stent into the aorta to trap the blood clot against the wall of the blood vessel and prevent it from travelling, he added. They then removed the blood clots from the patient’s leg to restore blood flow there.

The doctors later published a paper in the British Journal of Surgery, the first publication in Asia involving the treatment of arterial blood clots in COVID-19 patients. It is also the first publication in the world to describe blood clots in the aorta in COVID-19 patients.
FINDING THE SOURCE OF THE PROBLEM
The patient, Mr Ullah Kefayet, tested positive for COVID-19 in May after coming down with a fever and experiencing breathlessness. Two or three days after he was warded, he felt pain in his right foot and his toes had turned black.
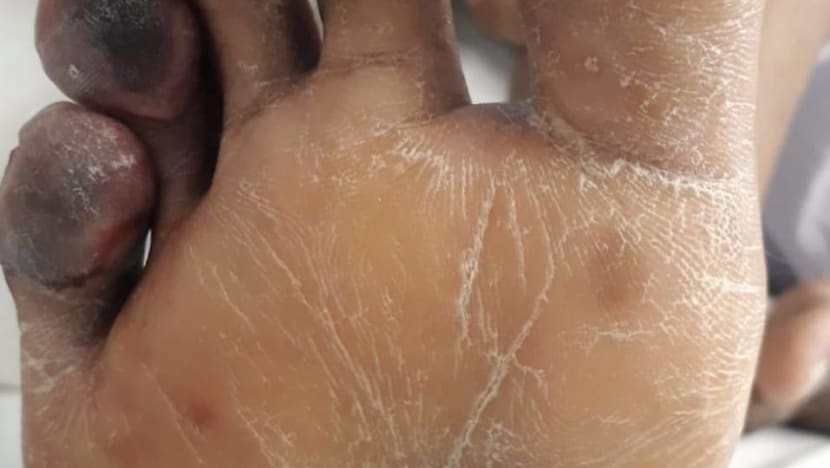
Since it was “very unusual” for young people to have gangrene in the legs if they have no other underlying medical conditions, the doctors decided to conduct a CT scan to find out what might have caused it.
The scan found a blood clot in the aorta, and parts of the clot had also broken off and moved to his right leg, spleen and kidneys, said Dr Tan. Aside from gangrene, this put the patient at risk of kidney failure or blood clots in the gastrointestinal tract.
“So it was quite concerning for a very young gentleman who couldn't walk. And he felt, how is he going to improve and go back to work again? And not only that, at this moment his life was at risk, and he’s also at risk of losing his toes and possibly his leg,” he added.
Timeline: No new COVID-19 case in Singapore's dormitories for the first time in more than 6 months
One month after the surgery, the gangrene patches on Mr Ullah’s toes started to disappear, and he started walking on his own. Three months after the surgery, all the black spots had disappeared.
He finally returned to work as a parcel delivery driver three weeks ago.
Speaking to reporters on a video call, Mr Ullah said that his family thought he had died because he did not contact them for a few days while he was in the intensive care unit after surgery.
Adding that he was initially worried for his health when he tested positive for COVID-19, Mr Ullah, who has worked in Singapore for 14 years, said he was relieved to recover the use of his right leg.
PREPARING FOR SURGERY AMID COVID-19
Although the stent procedure is conducted often, preparations by the team at TTSH and the National Centre for Infectious Diseases helped to get the logistics for the operation set up quickly amid COVID-19 restrictions, said Adjunct Associate Professor Pua Uei, senior consultant in diagnostic radiology.
“And we’ve been preparing this for a long time. So this actually helped us to really push him to surgery in a very safe and a very timely fashion,” he added.
Adding that it is “very challenging” to operate on patients amid the pandemic, especially those who are COVID-19 positive, Dr Tan noted that everyone involved in the surgery had to wear N95 masks, which are more uncomfortable than what they are used to.
“It is a very challenging environment to operate in. But we’ve been preparing this for a while, so we’re not new to the scenario,” he added.
READ: COVID-19 case dies from blood clot in lung artery more than 2 weeks after recovery, discharge: MOH
Blood clots have caused complications in other COVID-19 patients. In June, a 41-year-old man died from a blood clot in an artery in his lungs, two weeks after he recovered from the virus and was discharged.
In May, the Ministry of Health issued an advisory to all doctors to be “watchful” for possible cardiovascular issues in COVID-19 patients.
Noting that about one in 1,000 COVID-19 cases in Singapore experienced “cardiovascular events, such as heart attacks and blood clots”, Health Minister Gan Kim Yong said doctors should take extra precautions.
When the COVID-19 pandemic first struck, most doctors thought it was “just a respiratory illness”, said Dr Tan.
“But as we went on, we found that it caused more problems. It caused problems in clotting and not just in the arteries, but in the veins as well. Not just in the legs, there were also clots in the heart, some people had risks of heart attacks, clots in the brain that can cause strokes,” he added.
“I think we have been fortunate because most of our patients have been in the younger age group and less severely unwell,” said Dr Tan, when asked how common blood clots are in COVID-19 patients.
According to the surgeon, it has been found that these patients develop antibodies that cause their blood to become “sticky”. Some of them also see inflammation in the blood vessel wall, causing a predisposition to blood clots.
“But until now we are still not very clear about ... how it happens. We still don’t know, we are still unclear about this. At the moment most parts of Europe and America have reported this, we still have only theories but no confirmed definite cause of it.”
BOOKMARK THIS: Our comprehensive coverage of the coronavirus outbreak and its developments
Download our app or subscribe to our Telegram channel for the latest updates on the coronavirus outbreak: https://cna.asia/telegram












