People who got Sinovac vaccine nearly 5 times more likely to develop severe COVID-19 than Pfizer: Singapore study
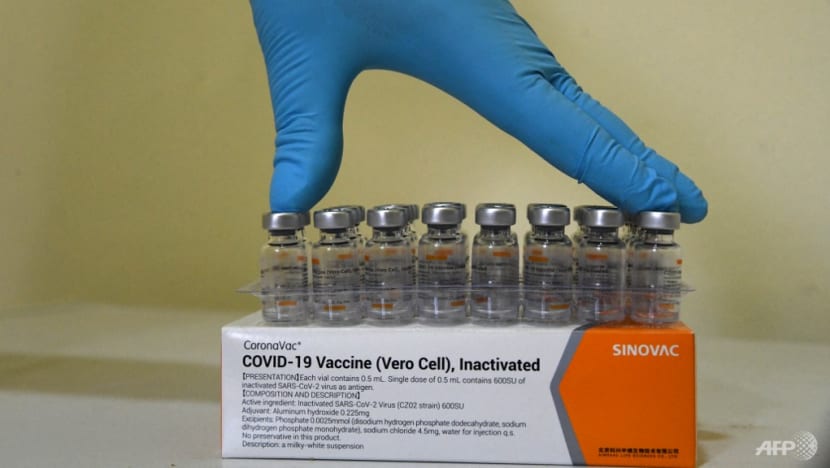
SINGAPORE: People who took Sinovac’s CoronaVac vaccine are nearly five times more likely to develop severe symptoms from COVID-19 than those who received the Pfizer-BioNTech/Comirnaty vaccine, a Singapore study has found.
The study, published on Tuesday (Apr 12), involved about 2.7 million people in Singapore aged 20 and above who received two doses under the national vaccination programme.
It covered a seven-week period in 2021 from Oct 1 to Nov 21, when cases in Singapore surged due to the Delta variant.
The team, which included infectious diseases experts from the National Centre for Infectious Diseases (NCID) and the Ministry of Health (MOH), observed a lower relative effectiveness of the two inactivated whole virus vaccines - Sinovac and Sinopharm - against COVID-19 infection compared to the mRNA vaccines - Pfizer-BioNTech and Moderna.
Those who received the Sinovac vaccine were 4.59 times more likely to have severe COVID-19 compared to those who received the Pfizer-BioNTech vaccine. They were also 2.37 times more likely to be infected, compared to those who took the Pfizer-BioNTech vaccine.
Severe disease was defined as those requiring oxygen supplementation in hospital, intensive care unit (ICU) admission or death.
The findings also suggest that the Moderna vaccine is more effective at preventing severe disease than the Pfizer-BioNTech vaccine.
Those who took the Moderna were found to be less than half (0.42) times as likely to develop severe COVID-19 than Pfizer-BioNTech recipients, and they are also less likely to be infected.
Citing a report from the US Centers for Disease Control and Prevention, the higher effectiveness of the Moderna vaccine was likely because of the higher mRNA content in the Moderna vaccine and longer time interval between the jabs.
| Vaccine | IRR of infection | IRR of severe disease |
| Pfizer-BioNTech/Comirnaty | 1.00 | 1.00 |
| Moderna | 0.84 | 0.42 |
| Sinovac | 2.37 | 4.59 |
| Sinopharm | 1.62 | 1.58 |
(IRR = adjusted incident rate ratio)
“Individuals vaccinated with two doses of inactivated whole virus vaccines were observed to have lower protection against COVID-19 infection compared with those vaccinated with mRNA vaccines,” the study stated.
“Nevertheless, both mRNA vaccines and inactivated whole virus vaccines provide sufficient protection against COVID-19 severe disease and vaccination remains a key strategy against the pandemic.”
As of noon on Tuesday, about 96 per cent of the eligible population in Singapore have been vaccinated under the national vaccination programme. About 73 per cent have received their booster shots.
THE STUDY
The study’s authors included NCID’s executive director Leo Yee Sin, chair of the expert committee on COVID-19 vaccination Benjamin Ong, MOH senior assistant director Wycliffe Wei, as well as MOH director of communicable diseases Vernon Lee.
The study aimed to compare the effectiveness of mRNA vaccines and inactivated whole virus vaccines in the same population. The findings will be useful for guiding policy recommendations to prevent infection and reduce strain on the healthcare system, the paper said.
Of the 2,709,899 individuals involved in the study, about 74 per cent received the Pfizer-BioNTech vaccine, 23 per cent took the Moderna vaccine, while 2 per cent received the Sinovac vaccine and 1 per cent the Sinopharm vaccine.
The Pfizer-BioNTech vaccine was approved for use under the programme in Singapore on Dec 30, 2020, while the Moderna and Sinovac vaccines were approved on Feb 3, 2021 and Oct 23, 2021 respectively.
From Aug 30, 2021, the Sinopharm vaccine was also available at private healthcare institutions, but not part of the national programme.
The cohort was restricted to those two weeks after completion of two vaccine doses to allow sufficient immune response, and who had received their second dose within 120 days of the analysis.
A total of 107,220 of those vaccinated were confirmed by polymerase chain reaction (PCR) tests to have COVID-19 over the study period, and 644 developed severe disease.
While the study was based on “comprehensive national data”, the team said there were “several limitations”.
This included the “residual confounding” from comorbidities as well as factors that influence a person’s choice of vaccine or risk of exposure. There were also asymptomatic cases who did not see a doctor and were not recorded as cases.
BOOKMARK THIS: Our comprehensive coverage of the COVID-19 pandemic and its developments
Download our app or subscribe to our Telegram channel for the latest updates on the coronavirus pandemic: https://cna.asia/telegram