For the first time, KKH to study whether long COVID is a problem in children in Singapore
It is likely that some children have come down with long COVID, which could affect their development. The coming study will determine how prevalent it is, among other important aims, the programme Talking Point learns.

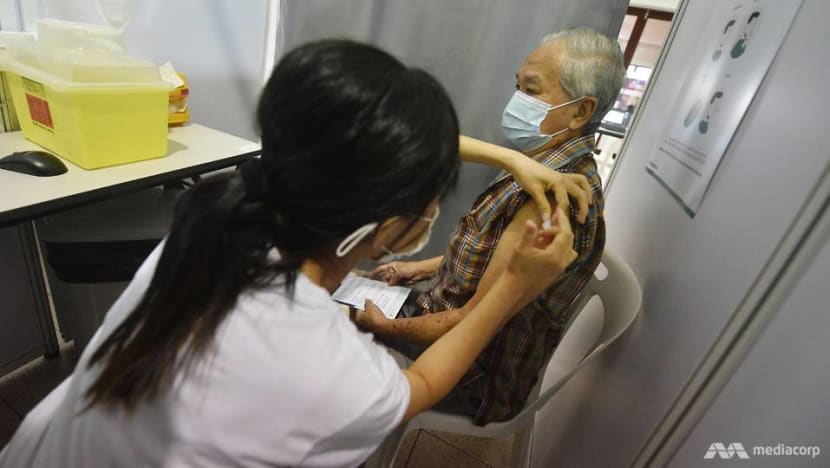
Siblings receiving their COVID-19 vaccinations at the Queenstown Community Club vaccination centre. (Photo: MOE)
SINGAPORE: Some studies overseas have put the prevalence of long COVID in children at anywhere from 4 to nearly 60 per cent of those who became infected with the virus.
But in Singapore, such a study — which would help to better manage children here who have had COVID-19 — has not been done yet.
That is about to change. KK Women’s and Children’s Hospital (KKH) is planning to embark on a study to determine whether long COVID is indeed a problem in young children and teenagers in Singapore.
Long COVID is the experience of lingering symptoms. And it can affect a child’s development if he or she has it.
“We do know that long COVID might potentially be a problem in children,” said KKH consultant Li Jiahui, who specialises in paediatric infectious disease. Hence the coming study will be “important”, she noted.

KKH intends to roll it out in the second half of this year, over a period of three to six months, she told the programme Talking Point. Results are expected by year end.
The study comes in the wake of the Omicron wave having seen children contract COVID-19 at the highest rate among all age groups in Singapore. For example, between December and February, around 27,000 children aged five to 11 were infected with the virus.
So far, KKH has not seen any cases of children with long COVID. But there are “several possibilities” as to why this is so, said Li.
One that she cited might be the way the hospital defines long COVID: As typically lasting for more than two months after the initial infection.

“And (children) might very well have symptoms that are really mild,” she added. “But they might otherwise be well enough to be attending school and not seek medical attention (for) these persistent symptoms.”
This means it is likely that some children have come down with long COVID, she noted.
The main aims of the KKH study are to determine how common it actually is and what “some of the risk factors are that can predispose a child or teenager to develop long COVID”, she said.
“(The study) will help us define the natural cause of long COVID in children. It will identify … how to better follow up on children who’ve had COVID-19.”
Persistent symptoms, such as sleep difficulties and disturbances in concentration and memory, can potentially affect children’s development and learning, she said.
“We do need more studies to characterise these difficulties and symptoms. Right now we don’t know the … trajectory of long COVID.”
Most of the studies of long COVID in children are from the West, she noted. And their findings “may not be entirely applicable to our context” and may not give an “accurate representation” of long COVID in children in Singapore.
For one thing, Asian children may show particular symptoms differently. “Secondly, the symptoms may be partly attributable to various factors such as lockdowns, social restrictions, safe management measures, which differ from country to country,” she cited.

Nonetheless, some symptoms are “red flags” that should alert parents to seek further attention for their children.
“In very young kids, if they’re unusually sleepy, lethargic, if they have a great disturbance in their appetite and their energy levels, all these would be warning signs,” she advised.
In older children, the symptoms include a persistent cough, headaches and disturbed sleep cycles. The children may not necessarily have long COVID, but “they’d need further evaluation and possibly further tests to see why they’re having these symptoms”.
LONG COVID IN ADULTS
Among adults, classic symptoms of long COVID include a persistent cough, breathlessness, chest tightness, heart palpitations and loss of stamina.
“In many ways, it’s complex … It’s a big mixture of different symptoms,” said Barnaby Young, who heads the Singapore Infectious Disease Clinical Research Network at the National Centre for Infectious Diseases (NCID).
“Sometimes people say that they didn’t have them initially, and they came on a couple of weeks later and can often be going through a waxing and waning pattern.”
Then there is brain fog, which is also common but is an area he highlighted as important and needing further research, “to really understand whether this is going to be a long-term problem”.
A recent United Kingdom study found that persistent brain fog from severe COVID-19 can cause cognitive impairment that is equivalent to losing 10 IQ points — and studies like this have been “very worrying for people to hear”, he noted.

At the NCID’s long COVID clinic, which he runs and was started in November, he has heard people describe brain fog as a loss of concentration and having difficulty focusing throughout the day.
Hor Chor Kiat, for one, has “difficulty choosing certain words to describe certain things” at times.
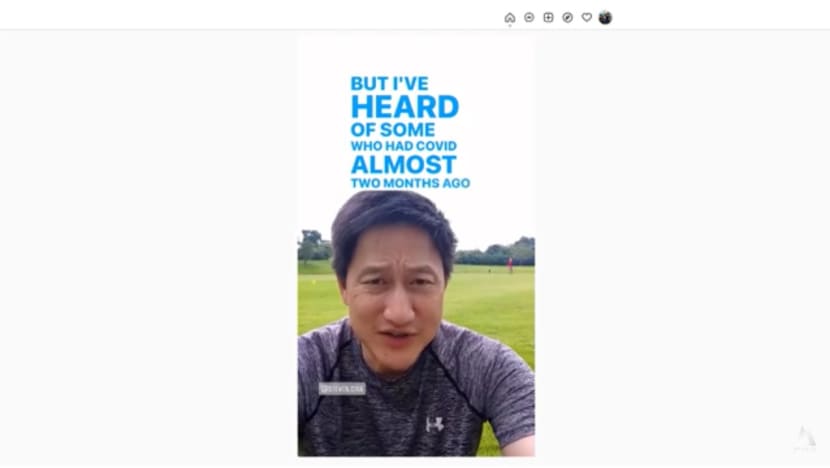
He was among Talking Point viewers who replied to the programme’s call for questions and stories from people suffering from COVID-19 symptoms two months after they tested negative for the disease.
Some of them had what they thought were lesser known symptoms, such as ringing in the ears and a headache that lingered on from time to time.

Joanne Thum had a back pain that she already recovered from, but after her COVID-19 infection, it “came back stronger” and became “even more painful”.
CNA executive producer Pearl Forss complained that her stomach “has just not been the same” following her infection.
“I’ve had constant bloating and discomfort. And I’ve had several rounds of food poisoning when my friends and family would be eating the same food and they’ll be okay,” she recounted.
It may be difficult to be sure, but all these symptoms can be attributed to long COVID, said Young. More than 200 different symptoms have been reported internationally.
There are also studies showing that long COVID affects women more than men.
Paradoxically, the immune system in women is “often better”, which probably means a higher risk of long COVID “because the immune system’s reactivity is continuing after the infection has resolved”, said Young.
But why do some people have such bad symptoms while others feel fine? And why do some people with mild initial symptoms also end up getting long COVID?
“We don’t really know what the exact trigger is,” he replied. “Something going wonky with the immune system is the most likely explanation.”
WATCH: Do you have long COVID? When COVID-19 symptoms linger (21:57)
What the data show, however, is that the elderly aged above 70 — a high-risk group for severe COVID-19 compared to younger patients — will also have more long COVID symptoms, pointed out Steve Yang, a consultant in The Respiratory Practice.
“If you’ve been in the ICU, if you’ve been on the ventilator … with a lot of scarring in your lungs, you’ll have a lot of long COVID symptoms,” he continued.
People can develop long COVID even if they are vaccinated. But vaccination helps: The evidence points to “around a 50 per cent reduction in the rates of long COVID”, noted Young.
According to the NCID, in findings published last year, one in 10 unvaccinated adult patients in Singapore had persistent symptoms six months after their initial infection.
WHAT CAN BE DONE ABOUT IT
For good management of long COVID’s symptoms, the general advice of Tan Tock Seng Hospital rehabilitation medicine consultant Wong Chin Jung is to “do light intensity exercises and not to over-exert”.
“For example, instead of jogging or running, maybe start with walks first and gradually increase them in intensity or even duration,” he suggested.
What people need to recognise is that there’s a period of time when the body doesn’t respond in a normal manner. Doing more doesn’t necessarily equate to significant improvement.”
The question of exercise was on the mind of Talking Point viewer Alif Adam, who felt that his muscles were taking longer to recover than before.
That experience is a typical one, observed Wong. “Even without COVID, just (by) resting at home for one month, most people will undergo deconditioning. There’ll be an element of the heart rate not being so good, muscles deteriorating,” he said.
“What long COVID does is it hinders the ability to tackle the deconditioning aspect.”

As for antiviral options such as Pfizer’s oral medicine Paxlovid, “don’t expect there to be a good treatment soon”, said Young.
Paxlovid is now approved only for adult patients with early-onset COVID-19 who are at high risk of severe illness.
A few reports suggest that it may also help those who already have long COVID, but Young thinks the chances are slim because their symptoms are “probably being driven by the immune system” and not the virus any more.
“Finding something that can modulate the immune system without suppressing it, without overstimulating it … is going to be very challenging,” he said.
In the United Kingdom, trials are being done to determine whether statins such as cholesterol medication and blood thinning agents can be used against long COVID. So there may be “some options” within the next year or so, he reckoned.
“But I don’t think we’ll get anything before then, and it may be that these agents turn out to not be effective.”
For Stephen Lim, who started to develop new symptoms a week or two after his initial recovery around mid-February, it took many specialist tests before he was put on medication for his lungs, heart and gastrointestinal tract.
Previously, he had been to accident and emergency four times; at one stage, he thought he was having a heart attack. His treatment plan gives him “a sort of assurance”, but he is still suffering from symptoms.
“I don’t go out as much any more. If I do go out, it’s best that I have someone with me,” he said.

Most people, according to Young, will be “back to where they were” within three months of infection. But some will continue to struggle after that.
“I’ve seen a few patients in the long COVID clinic who’ve had symptoms that have gone on for more than a year,” he said.
“We could be talking about this … in two years’ time. It could be something that drags on for that long for a small number of people.”
Watch this episode of Talking Point here. The programme airs on Channel 5 every Thursday at 9.30pm.





















