Commentary: How India’s COVID-19 story went from humanitarian crisis to managed calm
The country faced one of the most devastating waves when a more virulent variant ran rampant killing hundreds of thousands. It has managed to tame the beast but what lessons did its twists and turns yield? India’s former Auditor-General weighs in.

Volunteers wearing face masks as a precaution serve free food provided by a Hindu temple in Bengaluru, India, on Jun 30, 2021. (Photo: AP/Aijaz Rahi)
SINGAPORE: India ordered a total clampdown on its 1.3 billion population for three weeks last March when COVID-19 first appeared.
Though India only had 500 reported infections, the lockdown was harsh and brought untold misery on the poor but was believed to be in the larger interest of citizens to stop the spread of the virus. As cases increased, the lockdown was extended until May 31, 2020.
When the situation seemed to improve from June 2020 onwards, there was a phased opening of manufacturing and commercial establishments. States were also givsen more flexibility in easing social distancing rules.
After the number of cases declined from September 2020 to about end January 2021, the Indian government declared it had gained victory over the spread of the virus and that India was seeing the “endgame” of the pandemic.
India even increased its exports of vaccines and exported around 193 million doses. Lockdown curbs were eased with travel, local elections, religious gatherings and weddings permitted, albeit with some restrictions.
READ: Commentary: Survivors of India’s ferocious second COVID-19 wave left scarred by crisis
THINGS TAKE A NASTY TURN
Little did the government know that things were about to take a very nasty turn. By January, India totally let its guard down even though experts were pointing to the possibility of new variants.
There was a sudden surge in April with new infections spiking to the highest ever at about 300,000 cases a day.
The spike was attributed to super-spreader events such as the festival of Kumbh in which about 4 million devotees bathed in the holy Ganges in Hardwar and returned to their homes.

Another string of events that caused grievous setback was the huge rallies during elections in the states of Assam, West Bengal, Kerala and Tamil Nadu.
This second wave saw the spread of the Alpha variant, first identified in the United Kingdom. Scientists also point to a new Delta variant behind India’s second surge.
This variant is also believed to be triggering new surges in Bangladesh and Pakistan. India began recording a dramatic increase in new cases from Apr 15 this year, with more than 200,000 cases daily.
READ: Commentary: My harrowing brush with COVID-19 in New Delhi as India is ravaged
That was the worst phase of the pandemic when hospitals complained of inadequate supplies of oxygen. In an unprecedented situation, in April, a local hospital pleaded before the Delhi High court that it had only three hours of oxygen left, which would put to risk the lives of 400 of its patients.
The Government was finally seized by the seriousness and immensity of the problem facing the country, after the State Elections were completed, and drew up a cohesive action plan, in collaboration with the state governments.
A national lockdown was ruled out and states were advised to explore the use of micro-containment zones, where infection was detected, to protect livelihoods. Strict measures to minimise social mixing and increase the use of masks were stringently implemented.
The states were given flexibility to decide on micro containment to avoid worsening the hardships of the poor in areas which with fewer infections. States like Maharashtra and Kerala had to resort to extended lockdowns due to a very high incidence of infections.
(Why not allow dining in for those vaccinated when MICE and other big events can continue? Public health experts discuss whether new rules mean prior plans to live normally with COVID-19 will shift on this week’s Heart of the Matter podcast.)
VACCINATION AND DISCIPLINE IS KEY
Two-thirds of Indians have developed SARS-CoV-2 antibodies according to an Indian Council of Medical Research released in July but 400 million are still vulnerable.
Still, immunity has increased compared to when the survey was last released six months ago, which showed only 25 per cent had COVID-19 antibodies.
The prevalence of antibodies could be due to the large number who had been infected with the virus. India has a recorded 31.4 million infections. Only 12.6 per cent are fully vaccinated as of Jul 20.
The only silver lining is that India may be reaching “herd immunity”.
For a country the size and diversity of India, the ultimate answer still lies in ramping up its vaccination drive so the majority would not need hospital care and, hence, not strain the healthcare system. The vaccination schedule needs to pick up speed. Mobile and mass vaccination drives should be introduced.
READ: Commentary: Indonesia is Asia's new COVID-19 epicentre
The other issue is ensuring sufficient vaccine supplies. The Indian government has made concerted efforts to ensure that adequate quantities of the vaccine will be available as soon as possible.
India has almost two dozen vaccine production units. Covishield produced by the Serum Institute of India in Pune and Covaxin of Bharat Biotech in Hyderabad, are the main suppliers of its vaccine drive.
READ: Commentary: Overwhelmed Indonesian hospitals with COVID-19 cases behind high doctor fatalities
Covaxin is a home-grown vaccine Bharat Biotech developed in collaboration with the National Institute of Virology. About half a dozen vaccine makers such as Biological E Limited, Hyderabad and Panacea Biotech, have been commissioned to ramp up vaccine production.
The multinational pharmaceutical company Dr Reddy’s Laboratories has teamed up with Russia to procure Sputnik V vaccines.
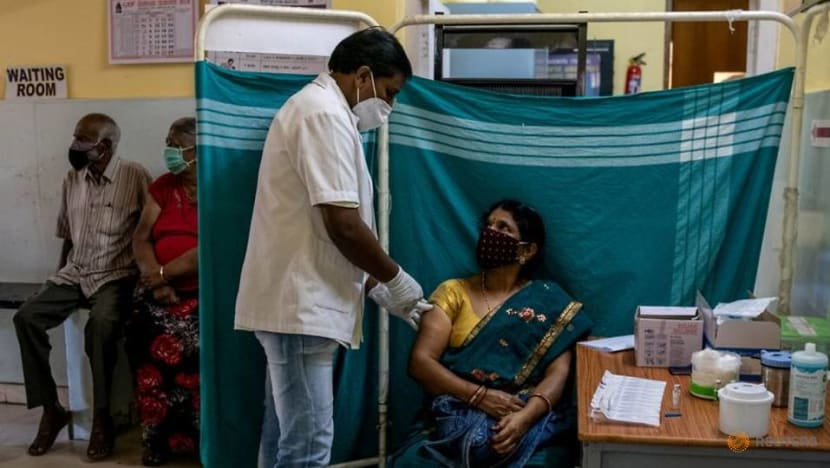
As the vaccination drive picks up, the Indian public has also grasped the need to maintain discipline given the devastating effects of the second wave.
Looking ahead, experts have insisted that opening indoor dining, coffee shops, gyms and similar “high-risk facilities” should be delayed. Until then, maintaining COVID-19 appropriate behaviour – mask, social distancing, sanitisation and avoidance of mass gatherings – is the norm to be followed.
Contributing to global knowledge of the virus, genome sequencing of the virus has been an important step taken to identify new potentially more infectious or deadly variants.
READ: Commentary: India’s COVID-19 crisis could cause long-lasting economic scars
The Indian SARS-CoV-2 Genomic Consortia was therefore set up last year, bringing together 10 labs in the country, though India is sequencing just over 1 per cent of all samples at the moment.
This could also help India track new variants or upticks in infection, using real-time epidemiological and sequencing data.
Months after its deadly wave, India seems to have gained control over the spread of the virus and precautionary steps are being taken to avert a third wave.
The government’s efforts, citizenry discipline, along with so many people who have developed antibodies because they caught the virus, have appeared to calm India’s COVID-19 crisis but to avoid another hit, a sustained vaccination drive is critical.
Vinod Rai is Distinguished Visiting Research Fellow at the Institute of South Asian Studies, National University of Singapore. He served as the 11th Comptroller and Auditor General of India and is a former chair of the United Nations Panel of External Auditors. He is also a Trustee on the global board of the International Financial Reporting Standards Foundation.














