Commentary: New primary healthcare plan for migrant workers can mitigate risk of disease outbreaks
A recent Request for Proposal by the Manpower Ministry sends a powerful signal that migrant worker health is now front and centre on the agenda, say two researchers from the NUS Saw Swee Hock School of Public Health.

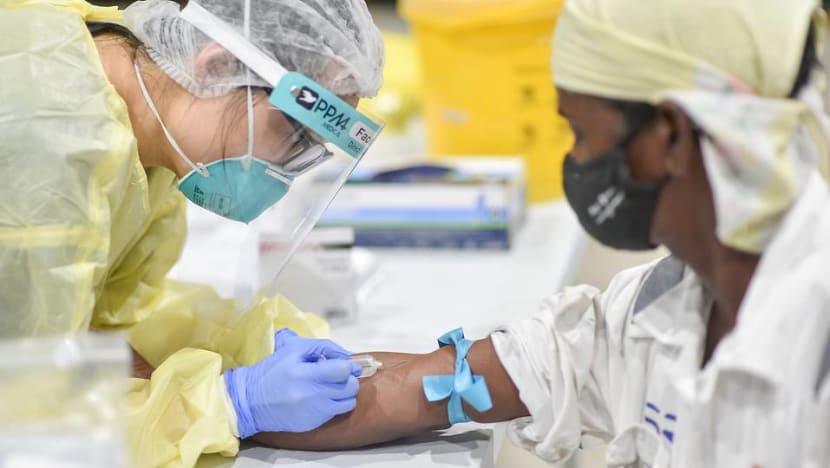
Migrant workers wait to be transported to a medical facility from their dormitory, amid the COVID-19 outbreak in Singapore, Apr 27, 2020. (Photo: REUTERS/Edgar Su)
SINGAPORE: In late June, the Ministry of Manpower (MOM) issued a Request for Proposal (RFP) for the provision of primary healthcare services to migrant workers.
In the RFP, the workers would be organised into six geographic regions with each having a comprehensive medical centre supported by mobile clinics and telemedicine capabilities.
The RFP sends a powerful signal that migrant worker health is now front and centre on the agenda and that the Government is prepared to intervene proactively and shape the market.
To appreciate the significance of this plan, one needs to understand how migrant healthcare worked.
MIGRANT WORKER HEALTHCARE CAN BE IMPROVED
Today’s approach for migrant worker healthcare is largely reactive, focusing on episodic treatment of acute conditions such as injuries and infections with minimal attention to preventive health.
READ: IN FOCUS: How fewer migrant workers means challenges beyond the construction sector
Even in immediate care, little is known about the extent, duration, whether adequate treatment is delivered and whether the costs are fully borne by employers.
Health insurance today mainly covers in-patient and day surgery expenses and is more limited in covering chronic conditions which do not warrant medical attention in an in-patient setting.
So migrant workers may not seek treatment for chronic conditions such as diabetes, high blood pressure and high cholesterol due to cost barriers.
Through our networks, we know that prior to the COVID-19 pandemic, some migrant workers with chronic diseases such as diabetes would circumvent the cost issue by seeking care in their home countries with medicines prescribed for an entire year or brought into Singapore informally by friends at regular intervals.
This arrangement was far from ideal and today is no longer even tenable given travel restrictions.
A GOLDEN OPPORTUNITY
The organisation of primary care as laid out in the RFP presents a golden opportunity to re-imagine primary healthcare for migrant workers.
Primary care should be comprehensive, accessible, and affordable, with strong coordination and continuity of care. There is further opportunity to encourage providers to innovate care models given the stable patient population in a clearly defined geography and the prescribed capabilities operators need to possess.
Patients with high blood pressure need only to consult the physician only once a year instead of the quarterly visits, if daily blood pressure readings can be captured in the dormitories, patients communicate remotely with a care coordinator or physician assistant and medicines delivered to the dormitories.
READ: Commentary: Spate of workplace deaths and what needs addressing in Singapore's safety culture
While this arrangement may appear to segregate the migrant workers from the larger population, a tight primary care network would make sense from quality and efficiency perspectives whereby more timely and targeted interventions can be delivered.
This arrangement also allows for more culturally and linguistically sensitive settings for the migrant workers, with fewer logistical barriers.
The American integrated payer-provider Kaiser Permanente (KP) shows what successful primary care could look like. KP is both an insurer and a healthcare provider. Incentives are strongly aligned to keep patients healthy and minimise healthcare episodes through preventive services.
Interestingly, while KP is now in multiple states across the US serving all age groups, its genesis in 1933 was in employer-funded healthcare for workers building the Colorado River Aqueduct in the Mojave Desert.
Why has KP been able to achieve good and cost-effective patient outcomes?
First, it adopts an integrated, population health approach that pays equal attention to both acute, reactive care and preventive, proactive health services such as health education and screening.
READ: Can Singapore rely less on foreign workers? It's not just about dollars and cents, say observers
Second, it heavily uses care pathways to integrate and standardise care provided to ensure consistent, high quality care. A care pathway is a clinical protocol used to manage a defined group of patients (like those with a specific condition such as diabetes).
The protocol sets out step-by-step the tasks each healthcare professional is responsible for and the timeline to be followed. It is evidence-based and serves as a guide for clinicians on the best practices for managing patients with this condition.
Third, KP has prioritised “digitalisation” to seamlessly monitor patient outcomes and service delivery indicators. It can also identify opportunities to innovate and improve at both individual patient and at system levels.
For example, KP’s IT system allows them to identify when changes have been made to the care pathway, what results these changes produced, and their effects on costs. Changes which improve outcomes or optimise costs can then be scaled to other care providers in the KP system.
Finally, and perhaps most crucially, the adoption of a capitated healthcare financing model that utilises a fixed payment per person covering all eligible services with some financial upsides in the form of bonus payments for improved patient outcomes, has encouraged providers to invest in systems that minimises waste.
Providers keep the difference between the operating costs and the amount paid by the insurer. They are thus incentivised to invest in preventive health approaches such as health education and screening because early intervention can stop or slow disease progression, thereby reducing utilisation of costly healthcare services.
EXECUTION IS EVERYTHING
Beyond the intent of better structuring today’s haphazard provider networks, the RFP emphasises minimising language and cultural barriers.
READ: New task force set up to improve support for migrant workers' mental health
Healthcare providers must be able to communicate in the major languages used by migrant workers (for example, Tamil, Bengali and Mandarin). There are also provisions to allow recruitment of care professionals hailing from workers’ home countries to ensure care is provided in a culturally sensitive manner.
Will the RFP be successful in transforming primary care for the migrant worker population?
The right balance must be struck. The health financing model – how much, who pays and how is the system financed — is critical to achieve success and sustainability for the long term.
Workers should not be deterred from seeking care due to financial constraint, but the economics must be sustainable for operators.

But as Kaiser Permanente has shown, this is possible. It will require upfront investment in IT systems, hiring of staff in advance of demand, and maturing the operating models until the efficiencies and improvements in care kick in with corresponding decline in costs.
Hence bidders for the RFP will need a prospective payment system such as capitation to generate enough funds for these investments. But this may not be sufficient and some degree of initial government subsidisation will be needed.
READ: Commentary: Foreign labour shortages in construction sector is a wake-up call for change
Why should the Government, or rather the taxpayer, fund this? Beyond the humanitarian imperative, a healthy worker is a more productive worker.
The painful circuit breaker we have gone through last year makes it clear that a country is only as safe as its weakest link.
At present, a review of health insurance coverage for migrant workers is underway. While the exact design of the scheme is yet to be known, configuring a risk pooling mechanism for a community care insurance with shared responsibilities from the Government, employers, and employees in financing the premiums would make pragmatic sense in the long run.
A robust primary care system for migrant workers will strengthen disease surveillance and mitigate the risk of uncontrolled outbreaks.
The MOM should be applauded for taking this first step to improve migrant workers’ access to better healthcare.
But as John Doerr, the famous venture capitalist said:
Ideas are easy. Execution is everything. And it takes a team to win.
Chia Hui Xiang is a Research Assistant from the Leadership Institute for Global Health Transformation, and Tan Si Ying is a Research Fellow, both at the Saw Swee Hock School of Public Health, National University of Singapore.












