Commentary: Even if I knew a pandemic would hit, I would still choose nursing
Songs have been sung and applause given but the work is hard and can push people to their limits. Christopher Soh, an assistant nursing director gives a ring side view of what it is like to be a nurse in a pandemic.
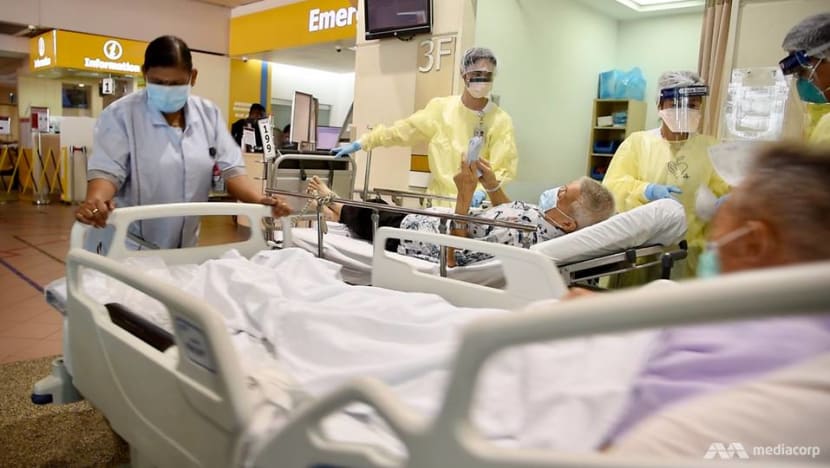
Patient care in the Emergency Department at Tan Tock Seng Hospital.
SINGAPORE: It was January 2020, on the eve of Chinese New Year and I was at the hospital finishing my shift.
I rushed off to squeeze in a haircut with my neighbourhood barber who despite having to close early for reunion dinner, kindly agreed to cut my hair.
Little did I know that the first COVID-19 case would reach our shores mere days later and the first locally transmitted case would follow soon after. That would be my last haircut for months.
In a way, that incident reminds me of what nursing or in general, the healthcare sector is about – a mix of unpredictability and challenge.
But as they say in financial investments – the greater the risk, the higher the rewards and in my nearly two decades as a nurse, I found this to be true.
READ: Commentary: Paying nurses more is long overdue but they need clearer professional ladders too
Looking back, my entry into nursing set the stage for what was to come. 18 years ago, I was a junior nurse, completing my diploma at Nanyang Polytechnic and just as I was entering the sector, SARS hit.
There was no time for leisurely training – my classmates and I were called up to the frontline and it was intense.
As a junior nurse, my role involved direct patient care, assessing their condition, taking blood and other samples from patients according to tests ordered by doctors and closely monitoring patients round the clock, and other clinical tasks.
This baptism of fire meant we had to get over a crippling fear of a deadly diseases: Getting infected. As frontliners, we have come to accept the risk and are mentally prepared – this is the call of our duty.
READ: Commentary: Second-hand smoke a health problem for home care workers
What was unbearable to me then was the thought of potentially spreading the infection to my family or loved ones.
This meant, we had to make sacrifices. In 2003, when SARS hit, my wife (who is also a nurse) and I were newly-weds and were living with my parents while we waited for our flat to be completed.
Seeing how deadly this was, we made a swift decision to move into our home that was barely furnished, to keep my parents safe and allay fears. After this we didn’t see our parents for a few months and called them instead.
But this was a small sacrifice compared to dying patients who did not get to see their loved ones before died and this included two of our own staff who succumbed to SARS.
The other battle we faced was the discrimination from the public. We understood this fear and uncertainty led people to avoid sitting next to us on public transport or not pick us up in taxis or ride-hailing cars.
READ: Commentary: Is housing still affordable for first-time homeowners?
But for every person who does that, we have many others who rally behind us, speak up for us and cheer us on.
One example is President Halimah Yacob who took to her social media to say the harassment and abuse of nurses and other healthcare workers was “abhorrent and unacceptable” and she asked for everyone to “respect and support our nurses and other healthcare workers who, despite facing a greater risk of exposure to the virus, continue stoically with their work to serve others.”
FROM H1N1 to COVID-19

When the COVID-19 situation escalated in Singapore last year, the Screening Centre, sited at the National Centre for Infectious Diseases (NCID) was ready to operate within 72 hours, after years of careful planning since 2016.
This time around, I was tasked with the planning and preparation of the Screening Centre from the perspective of a nursing administrator in the hospital.
Some examples would be planning the clinical setup, patient and staff routes, procuring medical equipment and coordination with many other departments: The laboratory, hospitality and environmental services, porter services, and administration teams among many others for smooth operations.
READ: Commentary: You don’t have to age and grow frail alone. Nurses have your back
The most adrenalin pumping time was when we had to go back to the drawing board and work out a solution, because things are fluid and evolving in real life, real time.
For example, when Singapore reported the first four cases of local transmission of the coronavirus with no travel history on Feb 4 2020, this meant a change in the definition of a suspect case to include those in close contact with Chinese travelers, such as tour operators, people working in tourist hotspots and tour guides.
This created a surge in attendance at the Screening Centre from about 70 to more than 300 within hours. We had to re-plan the segregation zones which were separated between high-risk and low-risk areas.
With the influx of people coming through the Screening Centre, more space was demarcated as high-risk areas, and we brought in additional tentage to cater to increase our capacity.
READ: Commentary: Music, a powerful medium that can move the memory of people with dementia
Another example was when Singapore’s border restrictions for several European countries kicked in, and many of the returning students and workers were also considered suspect cases.
In the thick of the action, protocols, workflows were constantly updated, sometimes even by the hour. The key was to maintain clear communications, help our staff teams adapt quickly and most importantly, assure them with our presence.
These experiences have been great learning tools for how to plan for the next large-scale outbreak.
LESSONS IN LEADERSHIP
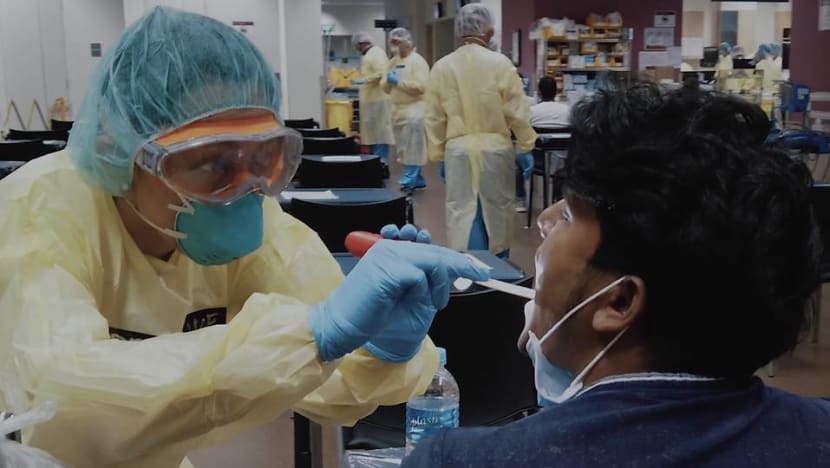
I saw first-hand how this leadership rests on the idea that no one has a monopoly on what is the best idea or solution - junior to senior staff are encouraged to come up with solutions independently when faced with unfamiliar terrain.
Eighteen months into battling this pandemic, I recall the many conversations with a multitude of colleagues, each playing a critical role and influencing the make or break of the mission at hand.
One text message stands out. It is from a colleague from the Department of Laboratory Medicine. Amid the surge, I proposed some changes that could speed up specimen dispatch process so that more samples in large quantities could be processed sooner.
This change would affect the workflow at the laboratory which was already facing heavy workloads. In a highly tense situation, it was a lot to ask for.
But hours later, I received a reply from saying: “Don’t worry, we are in this together and we will overcome this.”
This simple message speaks volumes of the trust and camaraderie and collective leadership. I hold it even more dear to me today because this dear friend unfortunately passed on after an acute bout of illness, just some months prior.
READ: Commentary: Overwhelmed Indonesian hospitals with COVID-19 cases behind high doctor fatalities
The priority of looking after our staff and establishing meaningful relationships is the key to successful pandemic operations – when we look after each other, we can look after others.
In the 18 years I have been a nurse, I have seen SARS, Ebola, Zika, H1N1, MERS-CoV and now COVID-19 and I am sure, there are others on the horizon.
Each one of those experiences have sharpened and deepened my skills as a nurse but what they have also shown me is that despite the challenges, the sacrifices and the exhaustion we feel when we are fighting a disease, I would choose nursing again.
To me, it is not just a job or a career. It is a life filled with meaning and worth living.
To my fellow nurses, Happy Nurses Day.
Christopher Soh is Assistant Director of Nursing, Emergency Department at the Tan Tock Seng Hospital.














