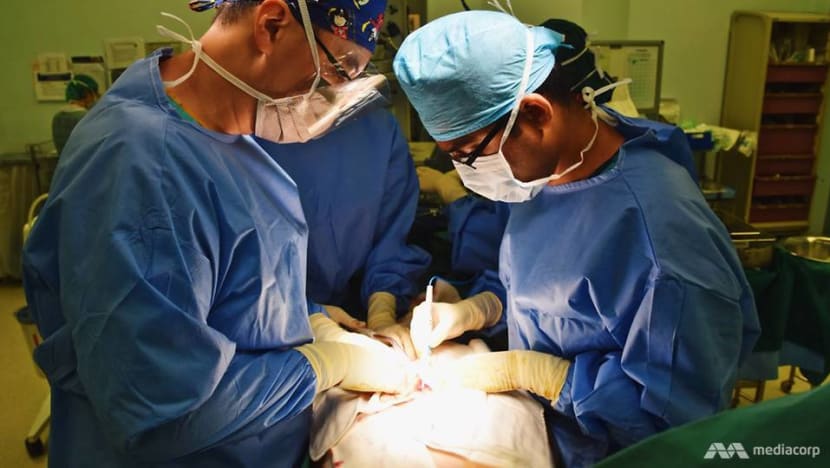
Inside the trauma unit: The surgeons who fight to save every life
If you are badly injured, they are the ones in the front line fighting to not only save you, but also help you get back on your feet. CNA Insider is given unprecedented access to Singapore’s most advanced trauma service.
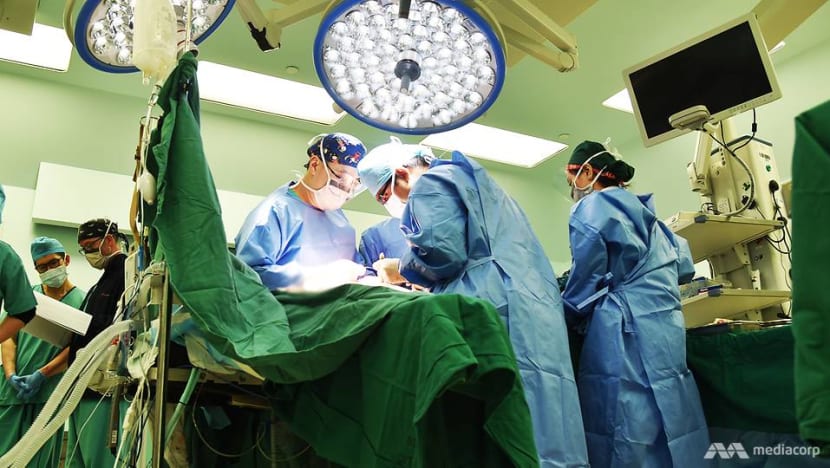
The trauma specialists from Tan Tock Seng Hospital, doing a job few are equipped to handle: Making life-and-death decisions for their patients, with time running out.
SINGAPORE: The alert came in at 9 p.m. on a Sunday. Dr Teo Li Tserng had been in hospital since he was called in for an emergency operation at noon. A busy day was about to get busier.
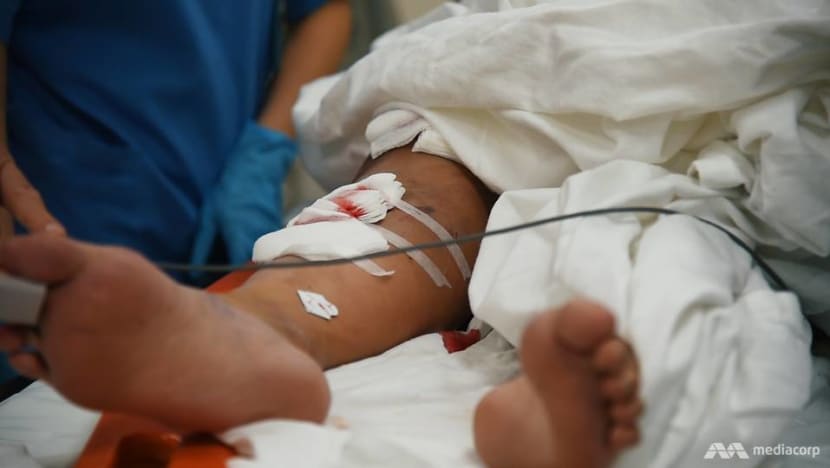
A patient with around 20 stab wounds — on her chest, abdomen, back and arms — had just been wheeled in, and time was running out.
Amid the whirlwind of activity and hubbub in the operating theatre, Dr Teo made the first crucial call: Put in a chest tube. If blood were to gush out, that would mean excess bleeding inside the area and having to open her up, an intrusive procedure he was hoping to avoid.
A hush fell momentarily as the tube was inserted. There was no spurt of blood.
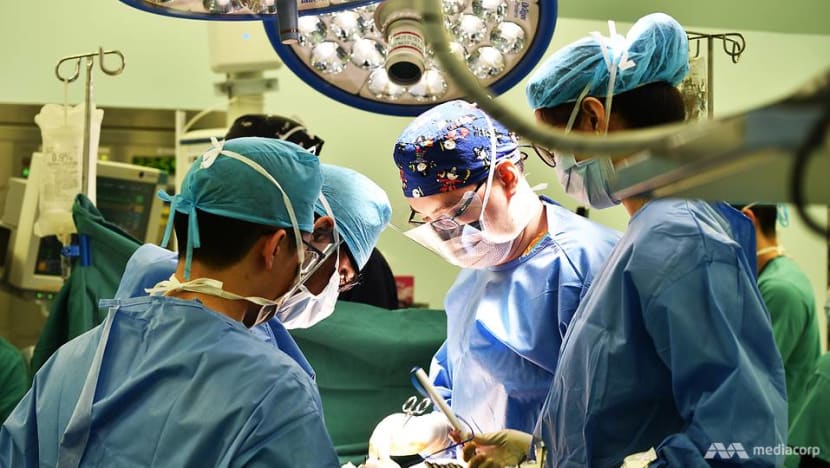
But something else soon caught his attention. Her blood pressure was falling — perhaps an issue with the anaesthetic, ventured another doctor.
Troubled, Dr Teo had taken a step back to watch the rest of the operation on Patient A’s wounds — something he often does during trauma operations, as CNA Insider would learn. “No, no,” he said half-impatiently. “I want to know if it’s due to blood loss. Are we missing something?”
Speeding up their search for an answer, his team found it in her abdomen. So we’ve got a breach there,” he said, referring to her intestines. “Bo bian (no choice), we need to open her up.”
‘ADRENALINE JUNKIES’
In Dr Teo’s area of speciality, time is always running out. The chief of trauma and acute care surgery at Tan Tock Seng Hospital is part of an exclusive breed — one of around 10 trauma surgeons in all of Singapore.

They are the “adrenaline junkies” of the medical profession — as he admits — plunging headfirst into life-threatening cases once they get the call.
Any form of injury caused by an external force can be considered a trauma. Many of their patients, however, have multiple injuries or trauma in multiple regions, whether from traffic accidents, bad falls or penetrating wounds.
Given unprecedented access to TTSH’s trauma unit, CNA Insider found a team of four surgeons always starting every case “on the back foot” as he described it.
While their emergency physician colleagues are the first to resuscitate and stabilise trauma patients brought to hospital, what comes next — to save the patients — is the trauma surgeon’s call.
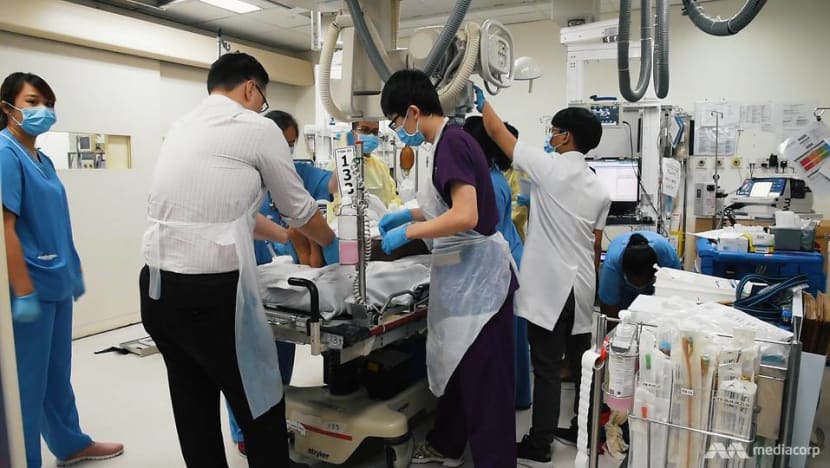
And they have less than an hour to get it right — the “golden hour”, starting the moment a trauma patient is injured, and not upon arrival in hospital. No period is more crucial to the patient’s survival and recovery than this.
“That’s where, if you’d like to put it, the thrill of doing trauma is,” said Dr Teo, who was appointed to his position in 2014. “You have to play catch up — if you don’t, and you don’t know what you’re doing, the patient tends to not do well, and that’s the challenge we have.”
The 43-year-old has a way of distilling thoughts about his highly specialised field from popular culture and through analogies, and there is one famous line from the film Forrest Gump that he correlates with trauma surgery.
“It’s like a box of chocolates. You really don’t know whether you’ll like everything in the box,” he said, contrasting it with planned surgery, which is “relatively predictable” and where even the curve balls are those “you sort of expect”.
It takes more than a dislike of monotony, however, to do what he does. The ability to “change direction in the management of a patient midstream” is a must.
That could have happened in the case of the stabbing victim, for example. “If the patient had bled into the chest after we put the chest tube in, I’d have had to change tack and quickly open the chest,” he explained.
When he gets the chance — when his patients are still conscious — he sees it as his job to share with them his “plan A and B” for treating them.
But what you wouldn’t know is I actually have up to plan F, which you don’t need to know because that’s when things happen really badly.”
That is the nature of trauma surgery. And it was something he was warned about when he was a young trainee hoping to specialise in the field.
He related what his mentor told him: “If you do trauma, when shit hits the fan, you must be able to mop it up properly. And not everybody can do it.”
WATCH: Life and death — On call with the trauma service (11:34)
48 HOURS IN HOSPITAL
The working hours are also a challenge. Over the one month that CNA Insider had to catch TTSH’s trauma team in action, it was rare to find Dr Teo without his caffeine fix — a cup of coffee — in his hands.
When he is not practising his other clinical interests in colorectal and other general surgery, he is on call for trauma cases, usually every alternate week. He is then activated about three times a day, even on weekends.

He may be at work by 7.30 a.m., but could still be called back after 5 p.m., which happened more than once during one of the weeks.
“Essentially, you barely get much rest because after you come back (home) from a trauma, you’re in bed, they call you again to update you on the results. Then after that, you get another (case),” he said.
“That’s the life for that week. You really just have to sleep when you can. … Cut down on other activities if you can.”
The longest shift he has worked was 48 hours, operating on four cases over that stretch. It was “just an unfortunate series of events” as he was about to go home, he said, shrugging it off.
“You’re changing, you’re in your car, they call you, and then you’re stuck — you’re back up again. It just rolled over, and by the time you know, 48 hours are up. You’re still in hospital.”
In such cases, he said, the adrenaline surge “makes you really alert and really quick”.
When there’s a lull, we’re really tired, but then that surge wakes us up … and you’re constantly doing something — you’re addressing a problem.”
“You’re going in and out,” he added. “And the patients are very sick, so you don’t really have time to think of whether you’ve had dinner or used the bathroom or not. So that’s just that.”
Patient A’s case was one of those that stretched into the early hours. It was around midnight, as his team was about to wrap up, when he said: “I just realised I’ve been here (in hospital) for 12 hours.”
Under these circumstances, he has found that humour is as good a tool as any to employ in the operating theatre. So he told his staff: “You’ve got two more hours before my caffeine runs out.”
And it was back at work at 7.30 a.m. again. Despite such demands, Dr Teo avers that there has not been a case he has missed, which goes to explain why he carries two phones.
“I sleep with my phones. I shower with my phones near me. I go for dinners with my phones on the table,” he said. “Everything else is secondary to a call.”
That calls for a certain lifestyle revolving around his on-duty period: No parties or inviting people to his home or football games with his friends.
“It sort of becomes part of your life. Everybody like my friends would, after a while, just ignore it. … If you show up, you show up — that sort of thing,” he added.
“And relationship-wise, people who are around you would also have to accept that.”
Chinese New Year is no exception. If a case calls, “then my mum would pack dinner”, he said matter-of-factly.

CONDUCTING THE ORCHESTRA
There is a reason that trauma consultants are so important when patients arrive with severe injuries. They are the ones who coordinate the care of those patients, the main part of the job scope.
This involves up to seven departments of the hospital, from the accident and emergency department to radiology to the intensive care unit. And they take their cue from Dr Teo’s team.
“If there’s no trauma surgeon, then there’s essentially no leader in the group,” he said. And that means patients with multiple injuries would not have anyone prioritising the sequence of treatments they should receive.
In Patient A’s case, for example, the orthopaedic surgeon wanted to do a full exploration of the wounds of her left wrist that same night. But Dr Teo decided that it would have to wait until the next day.
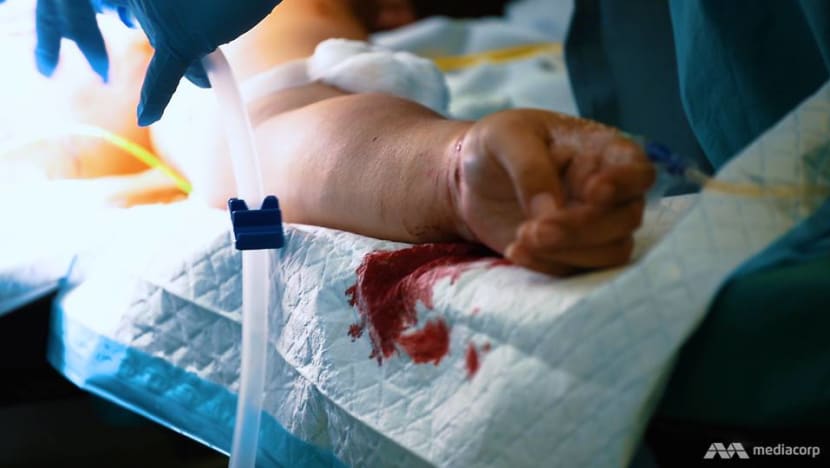
“At that moment in time, what was important was resuscitating the patient in terms of stopping the bleeding, making sure the lung didn’t have an air leak and making sure the heart didn’t have a leak of blood,” he said.
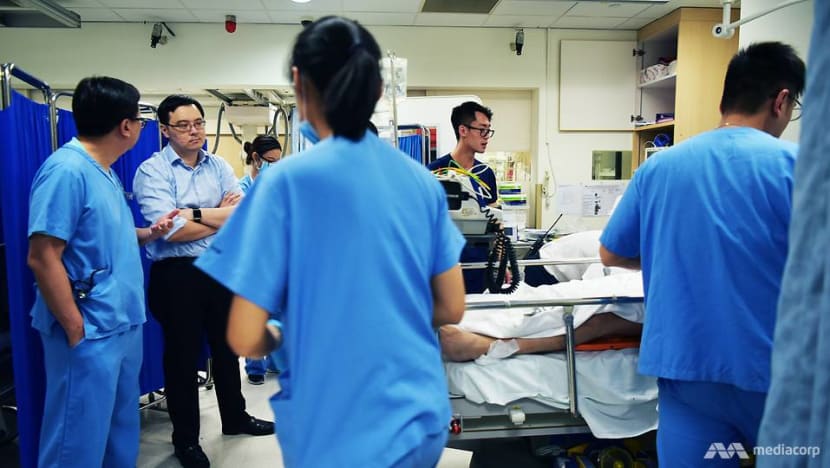
It is in those moments when he can be found standing aside and observing the medical practitioners in action, in order to give his input.
“If the trauma team leader is actively involved in doing something, he loses sight of everything else,” he explained.
I’m the only person who doesn’t seem to be doing anything, yet those in the know would know that the most stress is on the trauma team leader.”
There was an analogy he found apt here to explain why “someone needs to know a bit about everything”, enough to tell everybody what to do first.
“We’re like the conductor of an orchestra. We may not have all the sub-speciality knowledge that bassoon players have, for example, but we know what their roles are — we know when they’re supposed to come in,” he said.
“That’s where we coordinate them, to come in to play a nice tune, … in this case, to make sure that the patients get timely care.”
This “power of coordination”, he added, is “conferred” on trauma consultants by their hospital colleagues because with patients in the state they are in and the clock ticking, “the last thing we need to do is have a consensus”.
That power is only one part of the equation, however, as illustrated by another of his movie references. “Like what we watch in Spiderman, with great power comes great responsibility,” he cited. “So if something goes wrong, it’s our fault.”
It is not a simple responsibility to bear, for one thing because trauma surgeons usually know little about what exactly has happened to their patients.
“Most of the time, we only have collaborative history from maybe a passerby or whatever the paramedics saw,” explained Dr Teo. “We’d just have to go on our clinical experience and our hunches on what we’re going to do next.”

Patient B, a motorcyclist hit and dragged by a vehicle, was a case in point. How exactly the accident transpired or even what vehicle it was, which would offer more clues as to how the doctors should proceed, was unclear.
Dr Teo had to order a head-to-pelvis scan, which showed no obvious fracture of the skull. In the end, beyond leg and arm fractures, which he had asked his orthopaedic colleagues to fix, the patient was in the clear.
SLASHING MORTALITY RATES
It seemed like a well-oiled machine at work as Patient B was wheeled out of the emergency department to the main hospital, from the resuscitation room to the CT (computed tomography) scan room to the high dependency ward.
But it was not always like this at TTSH or any other hospital.
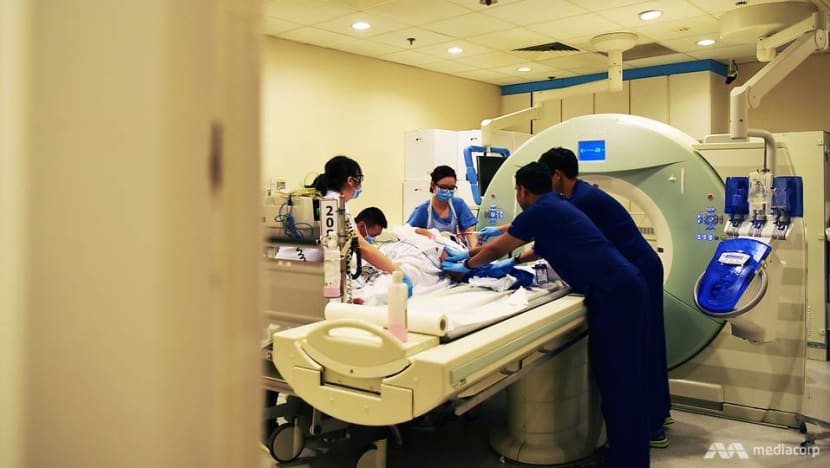
“Before a trauma system was ever invented, the surgeon or doctor with the loudest voice or greatest power in the hospital would do whatever he needed to do first,” said Dr Teo.
“The knowledge in Singapore on how to manage trauma was at best driven by personalities within a hospital.”
The care of trauma patients was poorly coordinated and even held up at times by, for example, delays in getting radiologists to do a scan.
This time, Dr Teo found a football analogy for the situation.
“Imagine a soccer team like Real Madrid. You can have every single defender knowing what he needs to do, but if you don’t have a manager who knows how to gel everybody together, you’re never going to get a Champions League-winning team,” he said.
But (for) every trauma patient that comes in, you need to win. Because if you lose, the patient dies. The equation is that simple.”
That state of affairs showed up in the mortality rates, compared with a mature healthcare system like the United States’.
Then in 2003, TTSH set up the Republic’s first trauma unit with two surgeons, Associate Professor Appasamy Vijayan and Assoc Prof Chiu Ming Terk.
In four years, the hospital halved its mortality rates. And over the period 2005 to 2012, the crude trauma mortality rate fell from 13.6 per cent to 5.9 per cent.
Within a decade of the unit's founding, the rates were “comparable if not better” than in major centres in the US, said Dr Teo, citing Maryland’s shock trauma centre’s benchmark of 4.78 per cent.
And in 2016, TTSH reduced it to 2.7 per cent.

He was just a trainee “gravitating towards the more emergency-based specialities” when the TTSH trauma service was being set up, and has not looked back ever since the two pioneer doctors brought him on board.
“I realised that I liked to follow up on my patients,” he said. “I like talking to patients, I like understanding their difficulties and being, in the local colloquial context, kaypoh about how to now help them manage their lives.
“The A&E people, if you psychoanalyse them, may like just to deal with the acute problem and then after that, they may not necessarily like to follow through.”
As CNA Insider discovered, the trauma service is not only about being in the operating theatre. After bringing mortality rates down to the US’ levels, the team began to focus more on returning patients to society — their “psychosocial reintegration”.
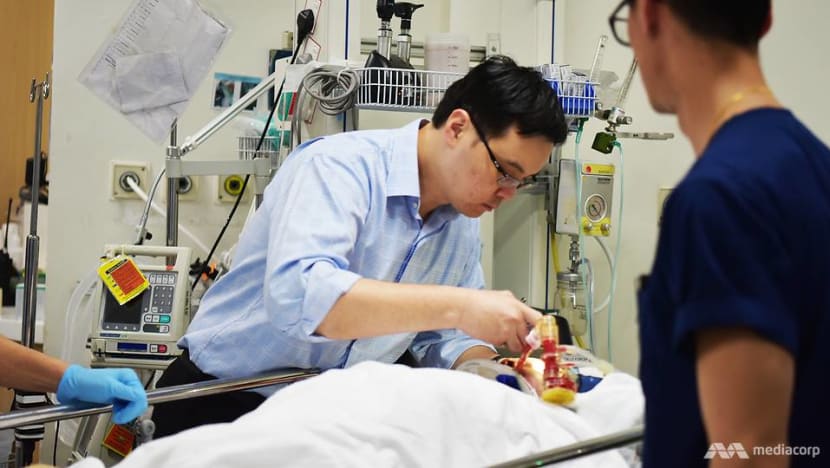
One way it is doing that is by partnering the Manpower Ministry to identify patients who can return to their workplaces “or at least a modification of their work, such that they can carry on being a part of society”.
“Our occupational therapists reassess the patients, go down to their areas of work, look at their scope of work and speak to their employers, and then re-scope the work such that the patient doesn’t necessarily jump back into his initial role,” explained Dr Teo.
Patient B is now at the beginning of that journey. Physiotherapist Debra Ow has been working daily with him to increase his strength and balance, to speed up his recovery process.
It started with something as simple as using a walker to get about on his feet again, with specific exercises scheduled in due course — and a lot of motivation provided by Ms Ow along the way.
“Words of encouragement do help these patients go a long way, especially if they’re in hospital for a period of time,” said the 25-year-old.
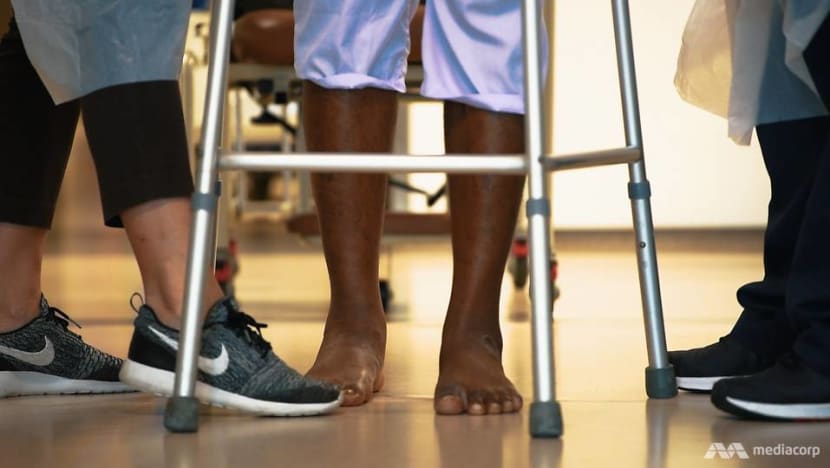
REHAB, EMOTIONAL TRAUMA, AND DEATH
The return-to-work programme was a natural progression for a trauma team who noticed that the majority of their patients were relatively young.
“If we don’t return them to the socio-economic state they started with, or at least something resembling that, then they’d be a burden on their own families and, at a bigger level, would be a burden on society because we’d have to support them,” said Dr Teo.
Once a week, the trauma surgeons do their rounds with physiotherapists and occupational therapists, among other rehabilitation practitioners, discussing cases and seeing patients together to understand the complexity of care.
The earlier a rehabilitation specialist gets involved in a case, the sooner he can identify what trauma doctors must do to facilitate a patient's rehabilitation later, for example where to put the splint in the case of a spinal injury.

It is not only the physiological aspect of care that is starting early in the treatment process at TTSH. There is also collaboration with psychologists who have an interest in post-trauma anxiety.
This is where senior psychologist Lanurse Chen comes in, like she did to help Patient C, a motorcyclist who collided with an elderly pedestrian. He suffered significant bruising, while the latter subsequently died from her injuries.
It was Dr Teo who called in Ms Chen, 38, after sensing that the patient “probably needed some support emotionally”. And there she was the next day, by his bedside to assuage his feelings of guilt.
He told her: “I saw that they (paramedics) were doing CPR on her. (I was like), ‘I don’t want this to happen, man. Come on.’” Trying to reassure him, she replied: “Of course, nobody wants that to happen.”
As the session went on, she suggested some logical reasoning tools to help prevent his feelings from overwhelming him.

Dr Teo has seen how important it can be to fix such psychological trauma, including in young patients. He cited a six-year-old boy who was injured and then could not pass his Primary One for three years.
“Everybody attributed it to a head injury, … but the scans were all normal,” related the doctor. After his team brought in a child psychiatrist and psychologist, the boy “started getting back to advancing” at school.
The case that has had the most impact on him, however, is not one of success, but rather of a patient he could not save — a motorcyclist around the age of 30 who was run over by three vehicles.
“When I went to see the wife of the patient, that’s where it changed my life. … She was extremely calm, which made me even more uncomfortable,” said Dr Teo, who was then roughly the same age as the deceased.
“She said, ‘Thank you for trying your best.’ … Then she asked me, ‘Can I go and look after my four-year-old kid now?’
That left an indelible impression on me because whatever we do to a patient, the downstream effect on the family — the four-year-old kid — is really large.”
Generally, his team members are left to their own devices to cope with a death. Dr Teo does so by running, playing computer games, travelling abroad sometimes and by “not being the friendliest person after a death”.
“But like I share with my team, we do need to bounce back because you never know when the next case is coming. … If you continue to not focus on your task, you may lose your next patient,” he added.

THE FUTURE OF TRAUMA
While mortality rates are no longer the sole markers of success for the trauma unit, there has been no let-up in the efforts to prevent deaths. But that now extends beyond the hospital, to outreach programmes in the community.
Some 90 per cent of TTSH’s trauma cases are caused by blunt injuries, the majority of which are motor vehicle accidents. So the trauma team has started giving talks on road safety, in partnership with the Traffic Police.
The topics include defensive driving techniques as well as the type of injuries that can be sustained and how to treat them at an accident scene.
“Part of this public awareness … is basically, for want of a better term, a scare tactic,” said Dr Teo, who would rather have fewer people coming in as trauma patients in the first place.
With self-drive holidays growing in popularity among Singaporeans, the talks are also done at travel fairs to educate the public on “what medication to avoid, how to time their drives, how to avoid fatigue and how to recognise fatigue”.
As of late, another pattern of injury has also emerged — from crashes caused by personal mobility devices (PMDs), he disclosed. And they usually involve the young, who are not quick enough to avoid such collisions.
While he lauded the recent move to decrease the speed limit of these devices to 10 kmh on footpaths, he noted that there were still dangers.
“A lot of these PMDs, if you look at it, can be used on a park connector, for which access to immediate medical care may be far away, and therefore the first responders would be important,” he said.

To reduce the incidence of severe injuries, the first project his team is planning is to engage educational institutions such as primary schools. The trauma unit will also be publishing a research paper on the issue next year.
As education, research and prevention become part of the mature trauma system alongside emergency and rehabilitative care, Dr Teo’s team has expanded.
He now has 10 junior doctors, which has also allowed him to look into collaborating with other hospitals whose facilities or trauma service are not at the level of TTSH, to help them manage trauma patients.
Most of all, however, he is pinning his hopes for the future of trauma care on the next generation.
“We hope that we can attract more people to be interested in trauma care, not only the surgical part of it, but also the overall trauma care of the patient and the holistic care,” he said.
Despite the long hours and emotions running high sometimes, Dr Teo still manages to personify calm on the job — one of the key attributes he said a trauma surgeon must bring to a “very chaotic situation”.
Then there is his sense of humour, sometimes morbid — especially in the operating theatre — but also meant to produce a calming effect on colleagues and patients alike; for example, when he checked on despatch rider Rafidah Eunos during his rounds.
The 30-year-old had been in an accident and needed stitches on her lip, among other treatments, but did not think it was necessary. “Can just leave it, lah,” she told him.
“You want to leave it, ah? No lah, you want to keep it pretty, right?” he replied in mock surprise. “Then next time you can still go for Miss Universe.”
Press him about what he has given up for the job, and he is emphatic that the word “sacrifice” should not come into something that one does willingly. And he looks no further than his patients to find the rewards.
“Some of my friends say, ‘You abuse yourself, you abuse your body, just to do this. Is it worth it?’” he said. “It’s worth it, because otherwise a young life would be lost.”