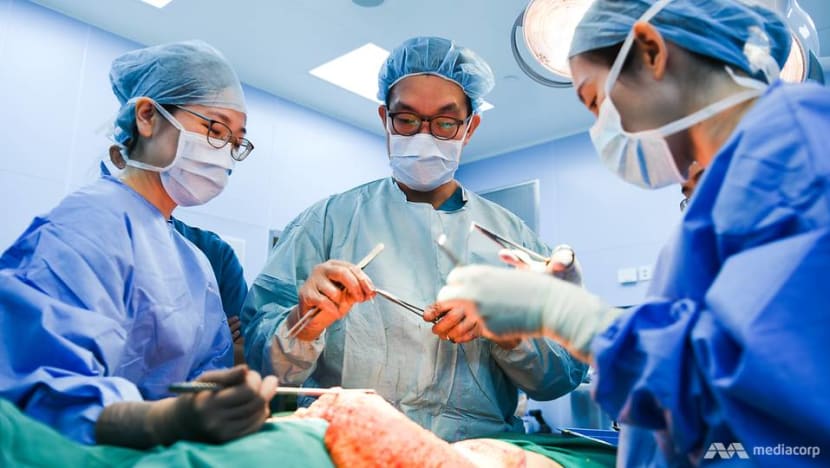
More than nose jobs and facelifts: The plastic surgeon who saves body parts
The work Dr Pek Chong Han does in a government hospital goes far beyond the aesthetic. In reconstructive plastic surgery, he patches “holes” to help patients regain their functions.
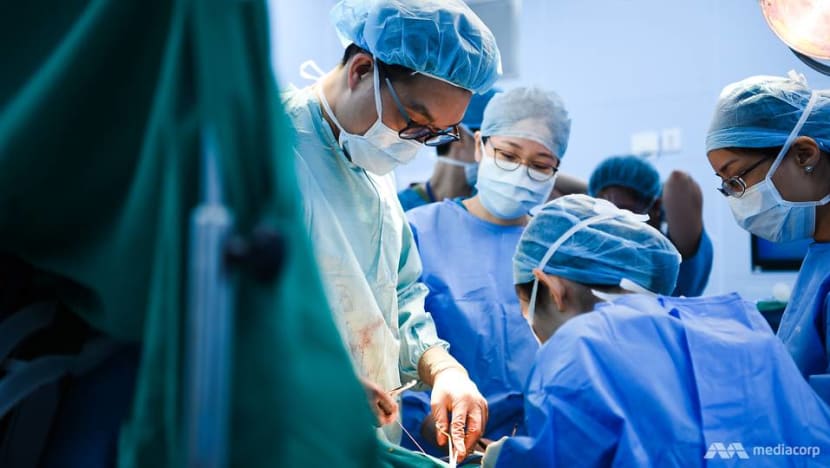
His job title reads “plastic surgeon”, but it is not only about beautifying his patients. Even during the COVID-19 “circuit breaker”, when non-essential surgeries were postponed, he had many emergency cases.
Warning: This article contains graphic photographs of surgical procedures.
SINGAPORE: Dr Pek Chong Han has performed surgery on bacteria-infested feet and cancer-ridden tongues. But few of his patients, on introduction, are aware of why they must see him.
The mention of plastic surgery brings to mind procedures like breast augmentation and eye lifts. So he has to take a few moments to explain: Yes, he is a plastic surgeon. No, he is not here just to beautify them.
“It’s about making you recover faster ... or recover what you’ve lost to whatever disease,” said the 36-year-old, who has been with Khoo Teck Puat Hospital (KTPH) for three years.
While he does some cosmetic procedures, most of his work at the government hospital is reconstructive surgery. That means literally patching “holes” and restoring function to defective body parts.
In fact, the full name of the speciality is Plastic, Reconstructive and Aesthetic Surgery. The term “plastic”, he explained, comes from the Greek word plastikos, which means to be moulded or formed, rather than the “synthetic material”.
Where there is a hole, he is there to patch it up — whether it is a trauma case such as a facial laceration from a road accident, a severe foot wound aggravated by diabetes, or a deep burn.
Some holes are created by other surgeons, for instance after a big cancerous tumour is removed, and are later referred to the plastic surgery team, which currently comprises six doctors.
So Dr Pek could be working with neurosurgeons on the scalp, orthopaedic surgeons on the lower limbs and general surgeons for anything in between. The list is bound only by the human anatomy.
WATCH: Inside the work of a plastic surgeon at a public hospital (5:48)
That means he must be well acquainted with diseases in every body part and understand how to reconstruct those areas, he said. “We approach the same problem, (just) from a different angle.”
Quite apart from the glitz and glamour of cosmetic surgery, this is the work of its lesser known twin in the field of plastic surgery.
TO SPEAK AND SWALLOW AGAIN
One of the best parts of the job, said Dr Pek, is being in the “special ops force” behind these multi-disciplinary surgeries. It usually entails a discussion with the primary surgeon to come up with a “reconstructive plan”.
“When the army has something that they ... can’t do, they’d call (us), and then (we’d) come in and do something on top of what they can do, to help resolve that issue,” he said.
“We get to learn from others, and we also can help each other along the way.”
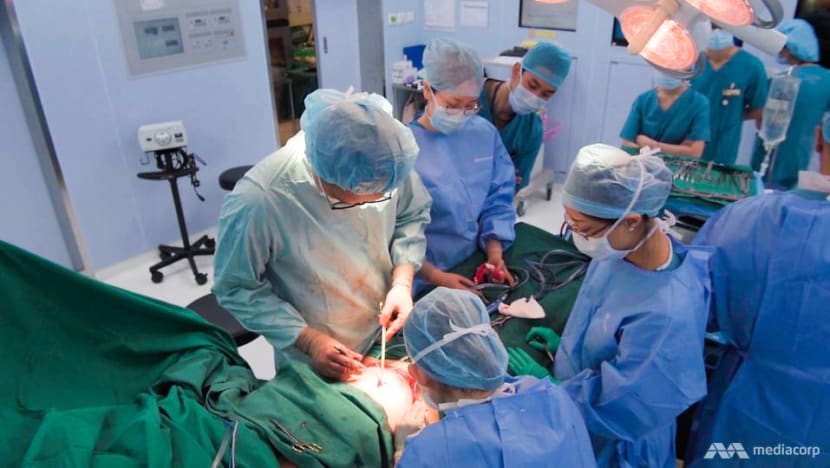
In the case of 46-year-old Ben (not his real name), having stage two cancer meant a 3.5-centimetre tumour on his tongue needed removing. That was the entire left side down to the floor of his mouth.
Armed with this information, Dr Pek determined how big a flap was needed from the donor body part, Ben’s left arm.
A flap differs from the more commonly known skin graft, which is a thin sheet of skin. A flap comprises skin, soft tissue and its accompanying blood vessels and nerves, which can restore the bulk of the tongue, with sensation and movement.
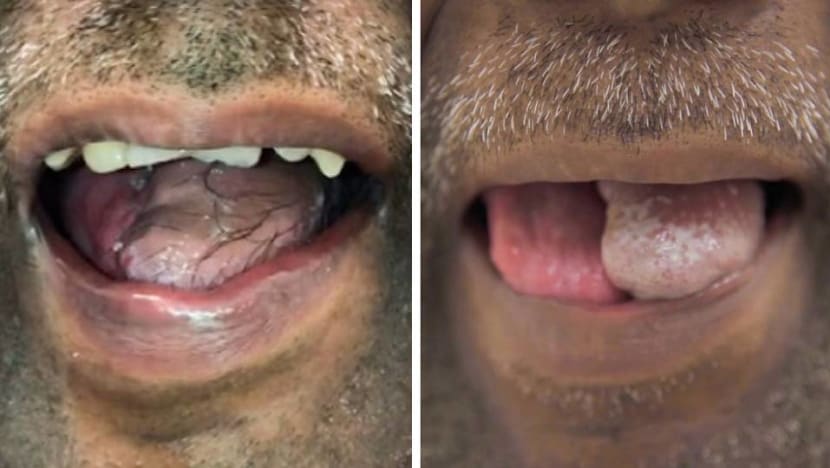
The work did not stop, however, with surgery last year. For many weeks, hair from the flap continued growing on Ben’s tongue and needed trimming during each follow-up consultation.
“(The skin) is alive, and therefore the cells are active and ... the hair’s also growing,” said Dr Pek. “It took us almost 20 or 30 minutes just to (trim) all the hair inside (each time).”
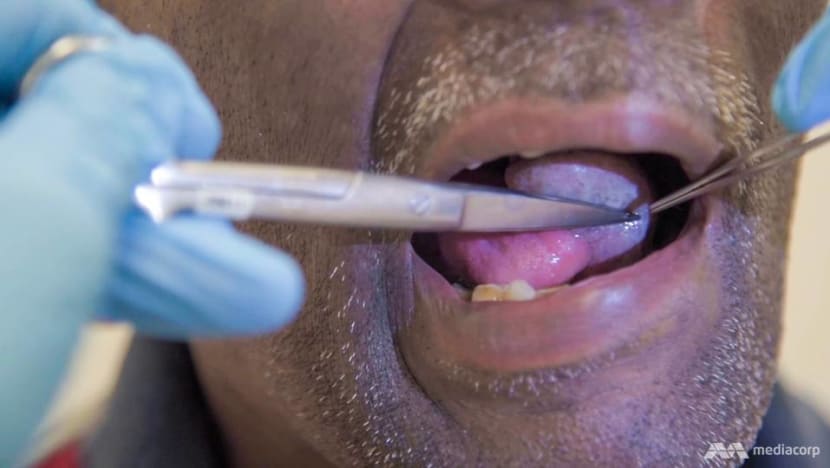
But with time, as the flap is constantly in contact with saliva, the cells undergo a “transformation”, or “metaplasia”, to mimic the mouth environment.
Ben also had speech therapy for a few months as therapists helped him to “maintain his airway to facilitate breathing” and relearn how to use his new tongue.
“It’s like going back to when you were young, like a baby,” said Ben, who could not chew, swallow and talk properly for “two to three months” post-surgery.
Six months after the operation, when CNA Insider met him, the flap was pinker in colour, and barely any hair was present. “It’s much closer to the final result now,” Dr Pek said while examining Ben’s tongue.
ALMOST LOSING A FOOT
For another patient, 33-year-old Kelvin Seah, plastic surgery meant being able to walk and play sports again, after flesh-eating bacteria attacked a significant portion of his left foot.
He was on holiday in Iceland when his foot began to swell. He had a cut on a toe then and suspects he caught the bacteria while at the iconic Blue Lagoon geothermal spa.
On returning home, he went into KTPH, where he had four operations in total. The first two involved his orthopaedic surgeon removing as much bacteria-infested flesh as possible. The third, for good measure, was to clear him of any bacteria.
By then, his tendons, bones and muscles lay exposed. Portions of his foot also lacked blood supply, which would not have supported a skin graft.
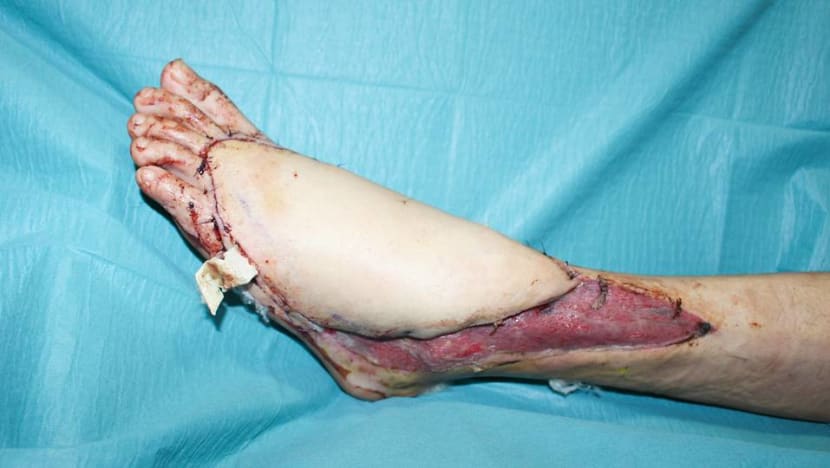
“The wound needs to be able to ‘receive’ a skin graft, much like applying wallpaper on a wall that’s been prepared,” said Dr Pek, who used a flap instead.
“This flap allows him to wiggle his toes nicely; he can move his ankles nicely. It gives him good contour, and it’s more resilient.”
But the flap, which had more fat cells as it was transplanted from the left thigh, also needed to adapt to the foot post-surgery.
As Seah had put on weight while recovering, the thigh flap grew disproportionately bigger than his foot. Liposuction had to be done to thin down the flap so that he could wear shoes of the same size again.
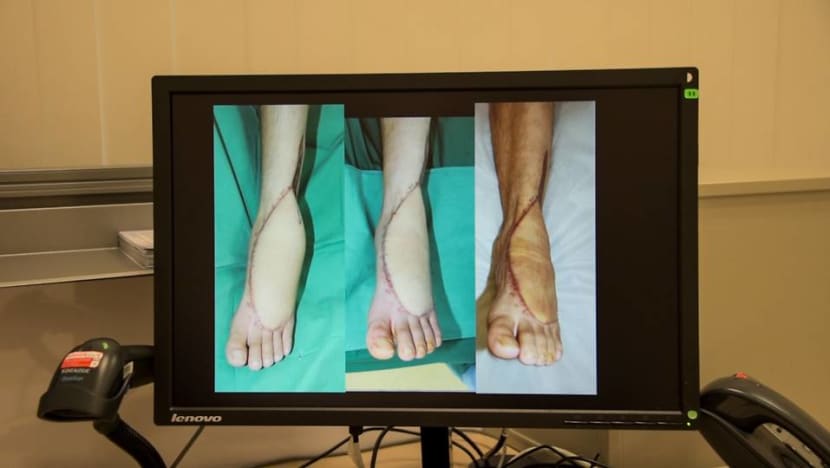
Two years after his surgery, he not only can walk, but also play sports such as basketball and badminton. Rock climbing, however, is one thing he cannot really do, as he cannot grip well with his toes, he said.
“That’s fine, I don’t do it much,” he added. “The most important thing is to resume my original lifestyle.”
RECONSTRUCTION VS COSMETIC
Whether one’s surgery is reconstructive or cosmetic is important in determining if its cost is covered under Medisave.
The distinction lies in whether the patient’s pre-existing condition is medical, said Dr Pek. There is, for the most part, “guidance” from the Health Ministry and the plastic surgery specialist board on what is medical or cosmetic in nature, he added.
“It isn’t black and white; it’s a little bit grey,” he said. “As a doctor, you’d have to determine what symptoms (the patients) have. Or is it just purely about their appearance?”

For example, if a patient asks for a “crooked” nose to be fixed but he does not see it as such, he would have to say no.
“As long as we’re trying to improve someone’s symptoms or function, then that, in general, should fall under some kind of medical indication,” he said.
That was the case for Vanessa (not her real name), who had an abdominoplasty, commonly known as a tummy tuck.
She had undergone bariatric surgery in 2015 — to make her stomach smaller — and the weight loss resulted in excess skin, which impaired her “hygiene around the groin area”. It also impeded exercise.
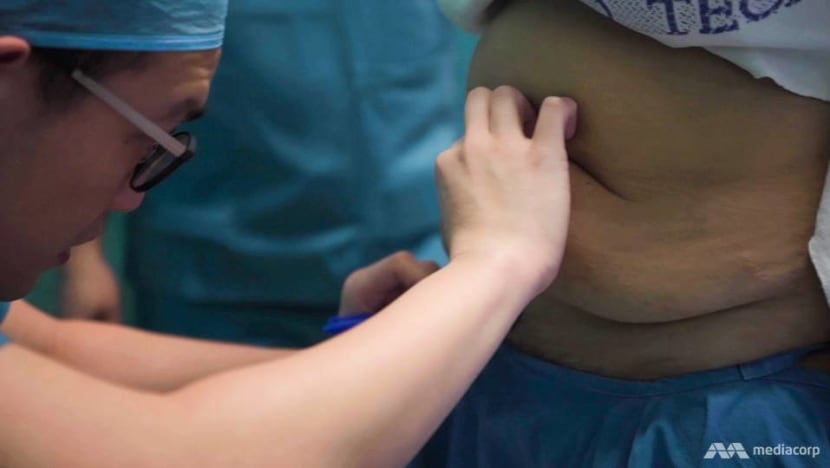
“Imagine you have a large waist pouch with a 1.5-litre or 2-litre Coke bottle in there and try to go for a run. It’s a very difficult task,” said Dr Pek.
The skin was unlikely to normalise on its own, he added, as it had been “expanded for many, many years”.
“There were tyres appearing on my stomach, so it wasn’t a good thought,” Vanessa described. “It was impacting my self-esteem.”
So last year, on the advice of the bariatric team, she opted for the tummy tuck, which involved cutting off the excess skin, shifting back the abdominal muscles that had splayed and repositioning her belly button.
“Health wise, I do believe … there’ll be no more hygiene issues, skin reactions and all those things,” she told CNA Insider post-surgery.
“I’m already looking forward to now going back to my exercise regime. It’s up to the individual to maintain it, so I’m not just relying on this surgery.”
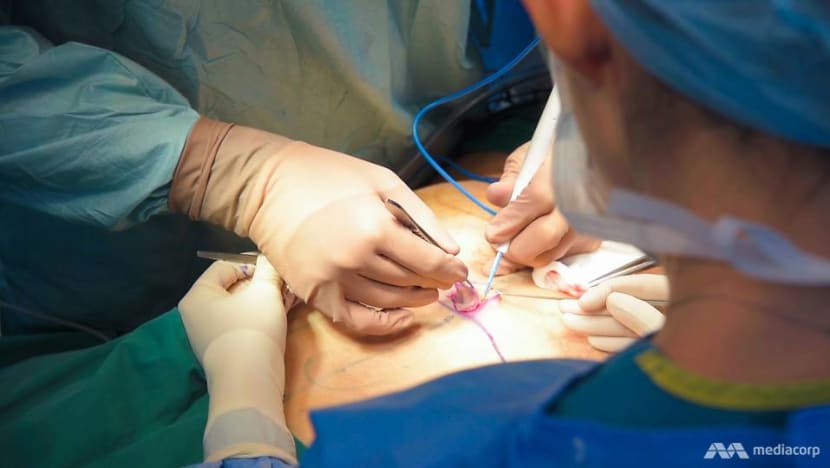
Following such surgeries, Dr Pek would review the scars to make sure that they heal well and that the patient is “happy with not just the physical appearance, but functional appearance”.
That includes finding out if the patient can move properly or experiences any pain when exercising.
‘A MEANINGFUL LAST STEP’
In a week, Dr Pek does about five surgeries. Even during the COVID-19 “circuit breaker”, when non-essential surgeries were postponed, he had many emergency cases. The most rewarding cases, however, are not necessarily the most challenging ones.
“Some of these patients, when you restore them to normality, they’re so grateful to you,” he said.

Before surgery, it is not uncommon for patients to experience anxiety, since they are facing a major bodily change, he noted. But the satisfaction comes when they “see how far they’ve (come)” and “gain confidence to return to society”.
“They come in with a severe problem … and usually when they come to the plastic surgery team, we’re the last part of the treatment plan. So we help to round off their journey on a high note,” he said.
“They can go back to functioning. To me, that’s a very meaningful last step.”
With all this in mind, he hopes that impressions of plastic surgery can move beyond what is “commonly sensationalised” in the mass media as merely aesthetic surgery. He hopes to bring more awareness in favour of breast reconstruction in particular.

“Singapore ... actually has one of the lowest breast reconstruction rates,” he said.
He has seen how mastectomy, the surgical removal of one or both breasts, is “a scarring surgery not only for the body but also for the mind”.
“Patients sometimes do suffer from depression ... because of a loss of a body part,” he said. “We hope to give patients more knowledge and the power of optionality in terms of what they want to do after breast cancer treatment.”
As for the money he could earn — never mind the glitz and glamour — if he were an aesthetic surgeon in private practice, he said: “To put it plainly, if I really want to earn money, there are better ways than being a doctor.”