commentary Commentary
Commentary: We have to live with an endemic COVID-19. Here's what that could look like
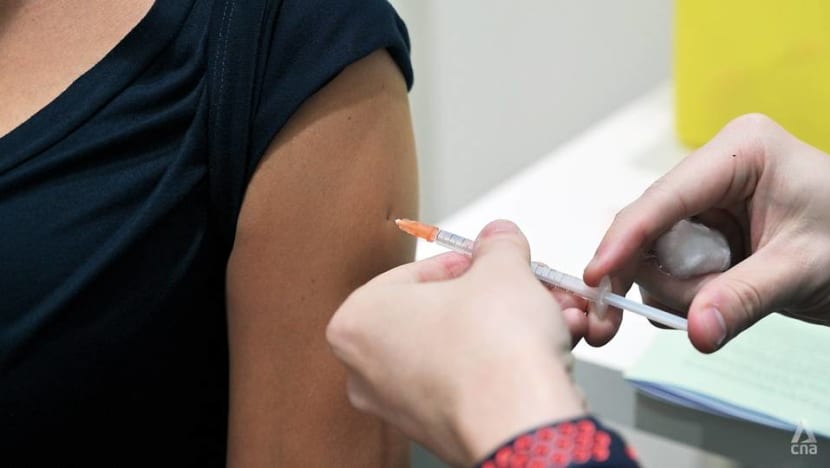
We should be prepared to live in a world where the majority are vaccinated and testing is quicker, says infectious disease expert Dr Leong Hoe Nam.

People wearing face masks cross a road amid the COVID-19 outbreak in Singapore on May 14, 2021. (File photo: Reuters/Caroline Chia)
SINGAPORE: We first heard rumblings of a novel virus in Wuhan in October 2019. People were hospitalised with pneumonia a few months later.
The first case of the severe acute respiratory syndrome now known as SARS-CoV-2 was finally announced by the World Health Organization (WHO) on Dec 31, 2019 and was only identified as COVID-19 weeks later.
Since then, the virus has been doing what all viruses are programmed to do: Survive by adapting to their human hosts, almost flawlessly.
READ: WHO classifies B1617 from India as COVID-19 variant of global concern
In less than 12 months, it arguably created the ultimate mutant, the B1617 strain first detected in India and has since been reported in 53 territories according to WHO.
This in a way signals to us an important turning point in our story: The endemic strain is here. On Friday (May 28), co-chair of the COVID-19 multi-ministry task force, Lawrence Wong alluded to this possibility too saying that the Government is planning for a scenario where we live with the virus.
Endemics have a constant presence in a specific location and can lead to outbreaks that happen anywhere. Four other coronaviruses already co-exist as common colds and we have come to live with them.
The question before us now is how did the B1617 strain become so successful at spreading across continents and can we live harmoniously with it?
ADAPTING BY MUTATING
The primary weapon of a virus is its genes. It uses single-stranded ribonucleic acid (RNA) for coding. RNA gives the virus up to a thousand times more opportunities to mutate than human genes which are coded with DNA.
And being single-stranded, there is no complementary strand to keep accidental mutations in check.
READ: FAQ: What you should know about getting infected after COVID-19 vaccination
READ: Singapore accelerates national COVID-19 vaccination programme, students the next group to be inoculated
Once the virus enters the human body, there are plenty of opportunities for it to mutate. Scientists estimate there could be between 1 billion and 100 billion copies of the virus in just one human body.
That is a staggering figure - at more than 10 times the number of people living on the planet. Most mutations are harmful to the virus itself. Many are neutral and provide no benefits to the virus, but some help its transmission and support its ability to survive.
The latest B1617 mutant benefits the virus in three distinct ways. The virus is more easily transmitted with higher viral loads which results in a greater total number of viral particles per cough.
Second, it is more infectious and can bind its targeted ACE2 protein receptor more easily. Third, it is better at evading the immune system although it is still unclear how much of a milder strain it has mutated into.
So, the B1617 is in the lead. It is replacing existing strains. Countries exposed to this mutant have reported increasing prevalence of this new strain, from Singapore to Nepal, Australia and the United Kingdom.
But precisely because the world answers the virus challenge with a disorganised mix of lockdowns, masks and social distancing, the mutation is able to break through these.
Even if the B1617 strain does not spread further, other strains – even though they are unrelated – could mutate in the same way, under evolutionary pressures.
This is called convergent evolution, where viruses from different strains adapt the same beneficial mutations without these strains ever meeting.
VACCINES – THE GOOD, THE BAD, THE UGLY
Just as most of the world’s vaccine manufacturers focused on developing immunity against the spike protein - the part of the virus which attaches to receptors on human cells and gains entry inside - the virus adapted by mutating the same protein, evading the immune response triggered by the vaccines.
The good news is that the mRNA vaccines produced by Pfizer and Moderna are highly effective against the original COVID-19. The bad news is that their 94 to 95 per cent efficacy falls to 70 to 75 per cent against the B1617 strain.
But the illness has been milder in those who have fallen sick from this “ultimate mutant”, transforming a deadly infection into a common cold. This was seen in the mild or asymptomatic people who fell sick in the Tan Tock Seng Hospital cluster despite having been vaccinated.
READ: Commentary: Booster shot for COVID-19 - not everyone needs it
READ: Commentary: Some pain even as Singapore rises to the challenge of tighter COVID-19 measures
Only one elderly patient required the very transient use of oxygen. So one could say that the SARS-CoV-2 only had bark without bite because of vaccination.
Which is why vaccinations must go on. The hope of every vaccine is to achieve “sterilising immunity” - when a vaccine prevents infection effectively because the immune system stops the virus from entering cells and replicating. But no vaccine has ever achieved that.
Breakthrough failures occur, constantly, in varying proportions but the impact of these failures diminishes with rising herd immunity.
The classic example is the measles vaccine, where herd immunity of greater than 90 per cent minimised breakthrough failures. Pockets of infection occur when the highly transmissible measles virus infects a community with low herd immunity, resulting in significant deaths.
Amidst the global vaccine shortage, we should therefore try and use the best available vaccine and achieve a high vaccine coverage of at least 70 to 90 per cent, especially in the face of mutants which render the vaccines less effective.
In a census continually updated, the US Center for Disease Control (CDC) reported only 1,949 hospitalised or fatal, vaccine breakthrough cases among 123 million fully vaccinated people. This equates to 0.002 per cent risk of hospitalisation or death.
READ: Commentary: COVID-19 unlikely to become a thing of the past anytime soon
READ: Commentary: Why is COVID-19 surging in the world’s most vaccinated country?
Even overestimated at 10 times higher risk of breakthrough infections with mutants, the burden on the hospitals and healthcare system would still be dramatically reduced.
Among vaccinated individuals, transmission to others has been significantly reduced. A research paper by British doctors and yet to be published has estimated the chances of vaccinated people transmitting the virus to members of their household were reduced by more than half, or 54 per cent, while the likelihood of it being transmitted to healthcare workers was cut by 92 per cent, 14 days after the second dose.
It is worth noting that this study was done between December 2020 and March 2021 involving 144,000 healthcare workers and their families – before the B1617 variant changed things significantly.
But the data shows that vaccinations do convert a deadly disease to a mild illness, reducing the need for hospitalisation, cutting the burden on healthcare systems and slowing the spread of infection across highly vaccinated communities.
READ: Singapore accelerates national COVID-19 vaccination programme, students the next group to be inoculated
Crucially, it shows vaccines are an integral strategy in living with an endemic virus. With the threat of failing immunity over time, and the virus adapting further, all vaccinated people must be prepared for a third booster shot to top up their immunity.
This may be a painful proposition but if we want to live with the virus, it’s a necessary step.
Science is rushing to answer the question if the third dose is best with the same or different technology. The possibility of a third dose guided by our understanding of the level of protection provided by antibodies may be a reality in future.
In some individuals, there may be even a requirement for repeated annual doses, much like how we get flu shots annually.
(Are COVID-19 vaccines still effective against new variants? And could these increase the risk of reinfection? Listen to the full conversation with Profs David Matchar and Gavin Smith on on CNA's Heart of the Matter podcast.)
WHAT ENDEMIC LIVING LOOKS LIKE
The future of endemic living with COVID-19 is tenable but it means we will need to accept and learn to live with the virus.
Apart from vaccinations, masks must persist too. Data clearly shows they reduce transmission but people must give up frivolous cosmetic masks and replace them with certified masks known to be effective.
Testing is another big plank in living with an endemic virus. Healthcare providers at family clinics must offer rapid antigen testing recommended and endorsed by the WHO. This is a cheaper, more easily administered alternative, with a much shorter 15-minute turnaround time.
The strength of these tests is their excellent sensitivity and their ability to identify COVID-19 positive individuals in the first five days of illness when infectiousness is highest.
READ: Fashionable masks may look good - but how can you tell if they protect against COVID-19?
According to the American CDC, antigen tests - when done correctly - approximate the gold standard PCR tests, in sensitivity and specificity, in the first five days of illness - especially when done in symptomatic persons. Similar home-care kits are available in countries such as the US and the United Kingdom.
These tests have limitations as a confirmatory test, a role better served by polymerase chain reaction, or PCR tests, which detect fragments of virus even after you are no longer infected.
We should expect that, in future, rapid antigen testing will be done at each individual’s home - either with a swab or a nasal rinse, or a saliva test kit, prior to leaving home, which is the holy grail.

This can be done when a person is showing symptoms, or a few times a week, at least.
These could also render those highly visible thermometer readers less necessary, if people carry their results with them before they head out.
Care of COVID-19 patients will improve with better medical technologies, and perhaps oral anti-viral treatments and highly effective, broadly neutralising, monoclonal antibodies that can kill the virus.
READ: Commentary: The systematic testing Singapore needs to ditch circuit breakers for good
Endemic living will happen in Singapore when we achieve a high vaccination rate of about 70 to 90 per cent of the population and when unlinked cases do not overwhelm our contact tracing capabilities.
Singapore may win the current fight, but the next battle will be even tougher. Preparing for endemic living with COVID-19 should start now.
The earlier we prepare ourselves, the more resilient we become. After all, the coronavirus has succeeded on four other prior occasions. There is no reason for it to fail now.
Dr Leong Hoe Nam is Infectious Disease Specialist at the Rophi Clinic at Mount Elizabeth Novena Hospital.















