Ebola drug remdesivir used to treat COVID-19 patients in Singapore as part of clinical trials
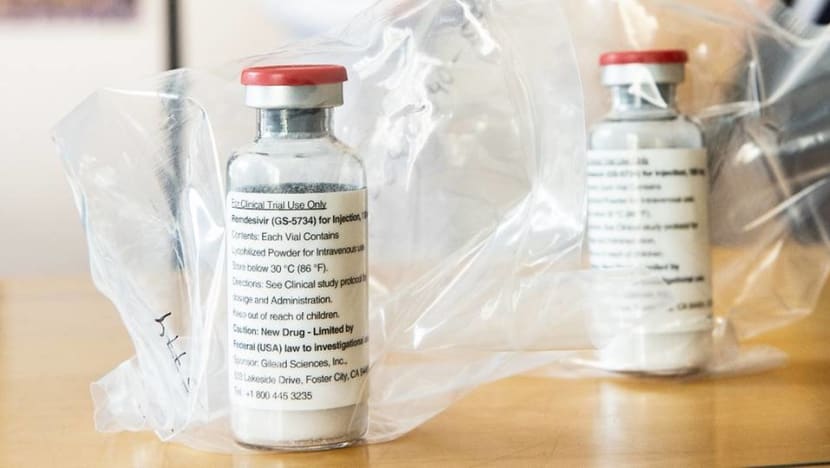
Vials of the drug Remdesivir, the Ebola drug that is being studied as a treatment for COVID-19. (Photo: AFP/Ulrich Perrey)
SINGAPORE: Doctors in Singapore are using remdesivir – a drug created originally to tackle Ebola – to treat COVID-19 patients here as part of clinical trials.
Dr Shawn Vasoo, clinical director at the National Centre for Infectious Diseases (NCID), told CNA that there are “no proven therapies” for the coronavirus, and that remdesivir is among the drugs being trialled here as a possible treatment for COVID-19 patients.
Antiviral drug remdesivir has been described by the World Health Organization as one of the most promising therapies against COVID-19, which also includes two HIV drugs and anti-malaria medications chloroquine and hydroxychloroquine.
Remdesivir was granted emergency use authorisation by the US Food and Drug Administration (FDA) last Friday (May 1) for severe COVID-19 cases. Japan said a day later it would “fast-track” a review of the drug so that it can be approved for use within “a week of so”.
The NCID is part of a workgroup announced by Health Minister Gan Kim Yong in March that is looking at how repurposed drugs and new therapies can be used to treat the disease.
READ: Singapore scientists plan to start testing COVID-19 vaccine this year
These include antiviral drugs, anti-inflammatory drugs, humoral therapies such as convalescent plasma and biologics, and vaccines.
The group will then provide a critical evaluation of the proposed treatments and address any queries about treatment regimens or adverse reactions.
Patients who have signed up to take part in the clinical trials will either receive remdesivir or a placebo, if they are in the control group.
“Some of these trials may be industry-sponsored, for example remdesivir, or conducted together with other national or international bodies,” Dr Vasoo said.
“The workgroup reviews available evidence as it emerges and makes recommendations for therapy for COVID-19 in the form of therapeutic guidance.
“Because they are as yet no proven therapies for COVID-19, it is important that robust clinical trials are conducted.”

READ: Optimism over COVID-19 drug, Fed stimulus boosts Dow 2.2%
WHAT IS REMDESIVIR?
Remdesivir, manufactured by pharmaceutical company Gilead, is an experimental, broad spectrum antiviral drug created to treat Ebola.
A major trial against Ebola started in the Democratic Republic of Congo about four years ago, but was halted last year when it did not boost survival rates as greatly as two monoclonal antibody drugs.
But in February this year, the US' National Institute of Allergy and Infectious Diseases (NIAID) said it was dusting off remdesivir to investigate how it would react against SARS-CoV-2, the pathogen that causes COVID-19.
Dr Anthony Fauci, who oversaw the study, told reporters at the White House last week that the data shows remdesivir has a “clear-cut, significant, positive effect” in COVID-19 patients’ recovery time.
But a trial of the drug in Wuhan, China – the epicentre of the pandemic – showed there were no benefits in terms of recovery time or mortality.
“In this study of adult patients admitted to hospital for severe COVID-19, remdesivir was not associated with statistically significant clinical benefits,” reported medical journal The Lancet, which published the findings.
The study in Wuhan had to be stopped early and it did not have enough participants as planned.
READ: Experimental coronavirus drug remdesivir failed in human trial
Dr Vasoo said: “We are still awaiting the publishing of the full results of the NIAID trial and further data on remdesivir, and also trial results (of) other agents such as immunomodulating (anti-inflammatory) drugs, such as tocilizumab.
“Meanwhile the mainstay for COVID-19 patients is supportive ICU and ventilator support for those with severe disease.”
HIV, MALARIA DRUGS USED AGAINST COVID-19
In February, the Ministry of Health's chief health scientist Prof Tan Chorh Chuan said retro antiviral drugs lopinavir and ritonavir – which are more commonly used to treat HIV – were given to “a small number” of patients in Singapore infected with the coronavirus.
READ: Cocktail of flu, HIV drugs appears to help fight coronavirus, say Thai doctors
Individual treatment decisions are made by doctors in consultation with their patients, with the “best available evidence”, said Dr Vasoo.
He added that there has been some “limited” clinical trial and experimental data regarding the use of lopinavir, ritonavir and hydroxychloroquine to treat COVID-19 patients.
“These have had some limited off-label use, on a case by case basis with careful discussion with patients or their next of kin, weighing the risk-benefit ratio,” Dr Vasoo explained.
While the outcomes of such “off-label use” are being monitored, it is not the same as a “well-executed clinical trial”, the NCID clinical director said.
The published data on all three drugs have not shown a “clear beneficial effect” or have shown “conflicting data”, he cautioned.
READ: Commentary: Can chloroquine really treat COVID-19?
He noted a trial in Hubei that used lopinavir and ritonavir on patients with severe COVID-19 infection had come back with “disappointing results”. The trial started within days after the virus was identified.
An editorial in the New England Journal of Medicine (NEJM), which published the findings, said “no benefit was observed in the primary end point of time to clinical improvement”.
The findings showed “intriguing results” for secondary end points, in that there were fewer deaths among patients who received the two HIV drugs, but this observation was “difficult to interpret” because of the small number (199) of patients in the trial.
The drugs had “no discernible effect” on viral shedding, the trial found.
READ: The drugs, tests and tactics that may conquer COVID-19
Dr Vasoo said the trial showed that both drugs did not seem to be effective in patients with severe or later stages of the disease.
“It is not so clear if it will be so in a study with earlier treatment or combination with other antivirals, and the authors suggest that more studies are needed,” he added.
“Thus there appears to be a limited role, if any, for lopinavir-ritonavir; certainly more data of its performance in earlier treatment and in combination with other anti-virals (eg beta-interferon) would be welcome.”
BOOKMARK THIS: Our comprehensive coverage of the coronavirus outbreak and its developments
Download our app or subscribe to our Telegram channel for the latest updates on the coronavirus outbreak: https://cna.asia/telegram














