5 things you need to know about a COVID-19 vaccine

Research assistant Marion Hong, of RNA medicines company Arcturus Therapeutics, conducts research on a vaccine for COVID-19 at a laboratory in San Diego. (File photo: Reuters/Bing Guan)
SINGAPORE: Early data this week from trials of three possible COVID-19 vaccines have raised hopes of a vaccine being rolled out as early as year’s end.
This is welcome news for billions of people in ending a global pandemic that has infected more than 14 million people and claimed about 610,000 lives worldwide.
But scientists have cautioned against raising expectations because these trials still require much larger studies to prove they can safely prevent infection or serious disease.
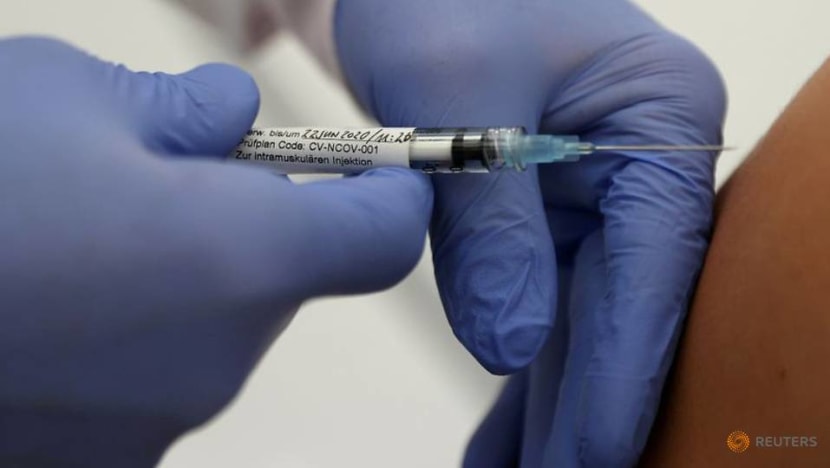
HOW DO VACCINES WORK?
Vaccines generally aim to boost the body’s immune system. For COVID-19, 23 vaccines are on human trial. These include inactivated vaccines which are made using particles of the virus that were killed so that they would not be able to infect or replicate in those injected with it.
The doses are also meant to help the body create antibodies against the dead virus. The private Chinese company Sinovac Biotech is among those pursuing this type of vaccine.
A new class of vaccine that uses genetic material in the form of ribonucleic acid (RNA) is also being explored, particularly by American company Moderna. The vaccine uses messenger RNA to produce viral proteins that mimic the outer surface of the coronavirus.
The body recognises these virus-like proteins as foreign invaders and can then mount an immune response against the actual virus. Moderna announced promising results on Jul 14 and said it would enter the final stage of human trials on Jul 27.
WHAT HAPPENS IN EACH PHASE OF CLINICAL TRIAL?
Producing a vaccine is a process that involves multiple stages. These include pre-clinical tests which sometimes involve testing on animals to determine if the vaccine produces a desired immune response.
Next comes Phase 1, which is when scientists assess the initial safety of the drug in a relatively small number of people.
Phase 2 judges the vaccine’s efficacy on the virus. Scientists would give the vaccine to a bigger group of people, usually in their hundreds and split into groups, to see if the vaccine acts differently in them. This stage is also used to further test the safety of the trial vaccine.
In Phase 3, the vaccine is introduced to thousands of participants and their blood is compared against to those who receive a placebo.
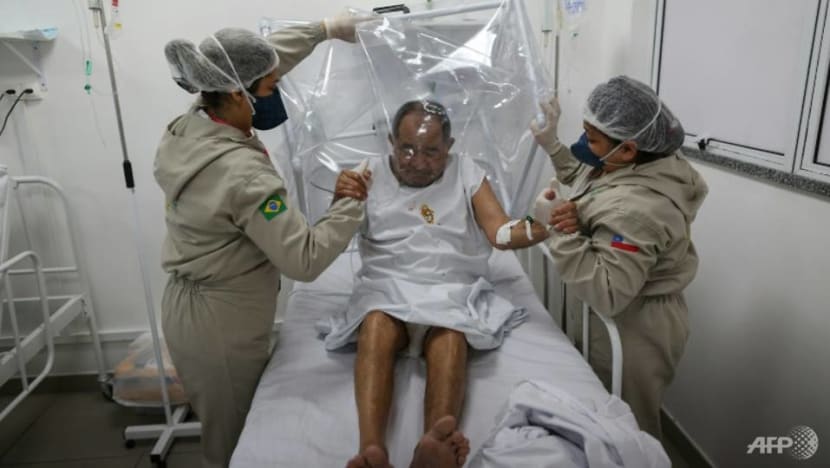
WHEN CAN WE GET A VACCINE?
There are more than 140 vaccines being tested, with 23 vaccine candidates undergoing human trials, according to WHO on Jul 15.
Two are in the final Phase 3 trials while one more will begin the final stretch later this month. China’s state-owned Assets Supervision and Administration Commission said a Chinese-made vaccine could be ready as early as the end of this year.
The World Health Organization meanwhile said in June that a few hundred million COVID-19 vaccine doses could be produced by the end of the year - and be targeted at those most vulnerable to the virus.
"If we're very lucky, there will be one or two successful candidates before the end of this year," WHO chief scientist Soumya Swaminathan told a virtual press conference.
READ: WHO eyes hundreds of millions of COVID-19 vaccine doses before 2021
Currently, several potential vaccines are in Phase 3 of development. A vaccine being developed by the British-Swedish company AstraZeneca and Oxford University is among them.
Data released on Jul 20 showed it induced an immune response in all study participants who received two doses without any serious side effects. Reports suggest emergency vaccines may be delivered by October.
CanSinoBiologics from China and the country's military research unit have also produced promising results. Researchers said their trial vaccine showed it appears to be safe and induced an immune response in most of the 508 healthy volunteers who got one dose of the vaccine.
About 77 per cent of study volunteers experienced side effects like fever or injection site pain, but none considered to be serious.
READ: Wave of promising study results raise hopes for COVID-19 vaccines
Vaccines usually take a number of years if not decades to produce - because several rounds of testing are required before they can be approved for use on humans. Given the enormity of the current health crisis, scientists are racing against time to try to produce a vaccine in a matter of months.
They will however have to prove they are safe and effective in trials involving thousands of subjects before final approval is given for their use. Given the amount of time and resources required, it comes as no surprise that developing vaccines is a costly affair.

WHICH COUNTRIES ARE INVOLVED?
Dozens of countries are involved in this project, including the United States, United Kingdom, China and Singapore.
More than 75 countries have also expressed interest in joining the COVAX financing scheme designed to guarantee fast and equitable access to COVID-19 vaccines, the GAVI vaccines alliance said on Jul 15.
“The 75 countries, which would finance the vaccines from public budgets, will partner with up to 90 poorer countries supported through voluntary donations to GAVI's COVAX Advance Market Commitment (AMC),” the alliance said in a statement.
READ: Vaccine alliance says 75 countries keen to join 'COVAX' access facility
Several of these efforts are transnational in nature. For example, AstraZeneca’s vaccine is now in a Phase 2/3 trial in England, as well as Phase 3 trials in Brazil and South Africa.
China’s state-owned company Sinopharm launched Phase 3 trials in July in the United Arab Emirates, where 15,000 people were scheduled to participate.

HOW LONG DID IT TAKE TO DEVELOP OTHER VACCINES?
Here is a look at how long it took to develop vaccines for some infectious diseases.
CHICKEN POX: Also known as primary varicella infection, it was only distinguished from herpes zoster (shingles) in the 1950s, and the first vaccine was developed in Japan in the 1970s.
YELLOW FEVER: This disease has plagued humans for more than 500 years, and a vaccine was finally created in 1937 by Nobel laureate Max Theiler, which is used to this day.
INFLUENZA: During the 1918 influenza pandemic, there were no known cures for the virus, and the first vaccine appeared only in 1945.
Just two years later, however, researchers concluded that seasonal changes in the composition of the virus meant existing vaccines became ineffective. They discovered that two main types of influenza viruses occur, along with multiple new strains, each year. For this reason, scientists have had to tweak the vaccines every year.
SARS: The virus first infected humans in China’s Guangdong province in 2002 and was identified in 2003 as an animal virus from possibly bats, before spreading to other animals and then humans.
Two SARS vaccines were evaluated in humans, said Professor Kanta Subbarao from the University of Melbourne.
“A number of promising candidates were tested in pre-clinical studies, but they weren't pursued because SARS didn't re-emerge," she said.
BOOKMARK THIS: Our comprehensive coverage of the coronavirus outbreak and its developments
Download our app or subscribe to our Telegram channel for the latest updates on the coronavirus outbreak: https://cna.asia/telegram














