FAQ: What cancer patients need to know about changes to treatment claims under MediShield Life

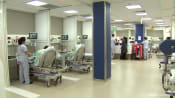
File photo of a woman taking pills. (Photo: iStock/diego_cervo)
SINGAPORE: The Ministry of Health (MOH) announced on Tuesday (Aug 17) that the design of the MediShield Life scheme will change for outpatient cancer drug treatment claims from September next year.
The changes come after the Government accepted the recommendations from the MediShield Life Council.
The council recommended that the authorities create a list of clinically proven and cost-effective outpatient cancer drug treatments, allow these cancer drug treatments to be claimable under MediShield Life, and set more granular claim limits to provide better coverage based on the cost of each treatment.
These are the new terms, according to MOH:
How much can I claim from MediShield Life?
Cancer patients can claim between S$200 and S$9,600 per month based on the cost of their treatment, if the treatment they are receiving is on a "positive list".
The current limit is S$3,000. The new MediShield Life claim limits for cancer drug treatments will be set based on post-subsidy bills.
What is covered by the 'positive list'?
The list will cover 90 per cent of existing treatments in the public sector. Among these treatments, most are deemed to be clinically proven and cost-effective.
However, some commonly used treatments that do not meet the clinical and cost effectiveness criteria will also be included. Such treatments will be assigned a claim limit similar to their subsidised alternatives.
You can find the list of drugs on MOH's website. The list will be updated every four months.
How about those undergoing treatment that is not on the "positive list"?
"There is a small proportion of patients who may find that their current treatment will either no longer be claimable or have the claim limit lowered with no subsidy extended," added the Health Ministry.
The changes will be implemented in September next year to "allow sufficient time" for existing patients to complete their current course of treatment and adjust their treatment plans, where needed, to another treatment that is "efficacious, cost-effective and eligible" for MediShield Life claims and subsidies, said MOH.
How much can I claim from MediSave?
The MediSave withdrawal limits for outpatient chemotherapy and outpatient cancer scans will be adjusted in tandem with the MediShield Life changes.
Patients may claim S$1,200 per month for cancer drug treatments with MediShield Life claim limit above S$5,400, and $600 per month for other treatments on the "positive list".
They may also claim an additional S$600 per year for cancer drug services and/or other cancer scans, including post-treatment monitoring and radiotherapy.
How many treatments will be subsidised?
Subsidised patients in public healthcare institutions currently receive up to 75 per cent subsidy for drugs under the Standard Drug List and Medication Assistance Fund.
Following price negotiations with drug manufacturers to achieve better drug prices and cost-effectiveness, 55 more cancer drugs qualify for such subsidies.
This will increase support for about 150 cancer drug treatments.
Who can get subsidies?
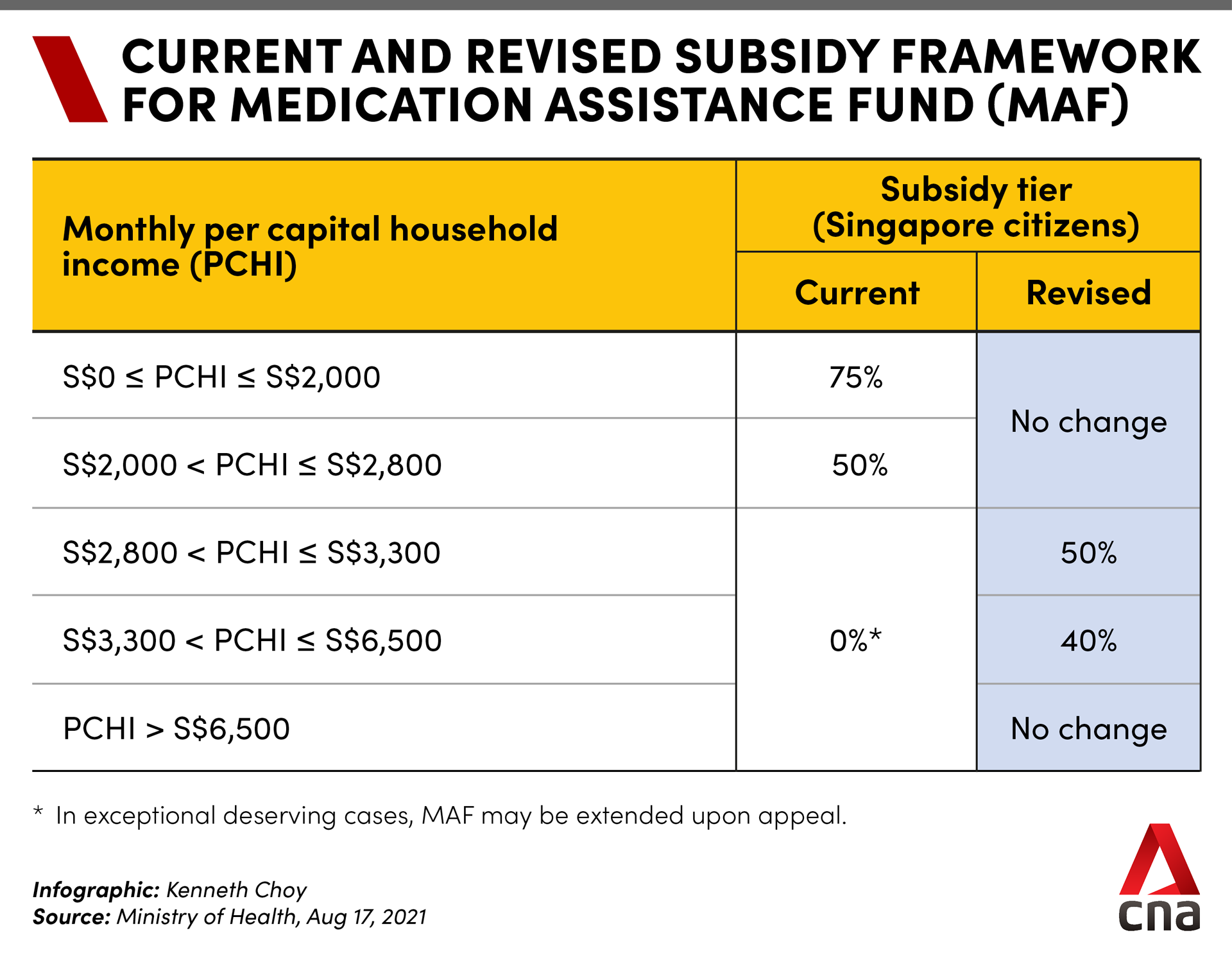
The Government will subsidise more cancer drug treatments and extend Medical Assistance Fund subsidies to more Singaporeans by raising the eligible income criteria, said MOH.
Medication Assistance Fund subsidies of up to 50 per cent will be extended to Singaporeans with monthly per capita household income of between S$2,800 and S$6,500, who currently do not enjoy subsidies.
This subsidy will apply to both cancer and non-cancer drugs listed on the Medication Assistance Fund.
How will Integrated Shield Plans be affected?
Currently, most IPs provide as-charged coverage for outpatient cancer drug treatments, subject to an overall policy year limit.
To ensure that Integrated Shield Plans are "aligned in encouraging the use of clinically proven and cost-effective cancer drug treatments", they will be required to only cover treatments that are on the MediShield Life "positive list" and set claim limits for each cancer drug treatment.
These changes will apply to all Integrated Shield Plans sold or renewed from April 2023 onwards. These changes do not affect Integrated Shield Plan riders, which are paid for fully in cash.