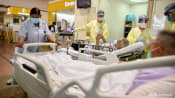
Singapore's COVID-19 death rate 'very low'; healthcare system stressed but not overwhelmed: Dr Puthucheary

SINGAPORE: Singapore has managed to keep the number of COVID-19 fatalities "very low", with a death rate of 0.2 per cent compared to 3 per cent or more in countries that experienced a surge in cases before vaccination, said Senior Minister of State for Health Janil Puthucheary on Monday (Nov 1).
The COVID-19 death rate of 0.2 per cent is “comparable to catching pneumonia”, he said in a ministerial statement in Parliament on the country's ICU and hospital capacity.
"But it does mean that over time, the absolute number of deaths from COVID-19 will rise despite the best possible medical care, and we could have 2,000 deaths per year. Most of these will be the elderly and already unwell," he added.
In comparison, about 4,000 patients die as a result of influenza, viral pneumonia and other respiratory diseases annually, Dr Puthucheary noted.
He said this is why the Government keeps emphasising the importance of vaccination and booster jabs.
“We must make sure that everyone who is infected with COVID-19 will receive proper medical care by our healthcare workers and hospital system, and be given the best chance to fight the disease,” he said.
DEATHS “VERY LOW”, HIGH VACCINATION COVERAGE
Singapore has had 407 COVID-19 fatalities as of noon on Sunday – 395 died in a hospital, eight at home and four at care facilities.
Dr Puthucheary noted that the number of deaths has increased in the past two months as the overall case count rose.
But Singapore has managed to keep fatalities "very low", he said, adding that about 99 per cent of the country's COVID-19 cases have had mild or no symptoms because of the high vaccination coverage.
Seniors who are unvaccinated and have underlying medical conditions are at “much greater risk” of severe illness and death, he said.
"Close to 95 per cent of those who died in the last six months were seniors aged 60 and above. Seventy-two per cent of all deceased cases had not been fully vaccinated,” he added.
“Almost all of the remaining 26 per cent who were fully vaccinated suffered from underlying medical conditions such as high blood pressure, diabetes, cancer, and heart, lung or kidney diseases. Underlying conditions add risks, even if the conditions are well controlled before the patient encounters COVID-19, especially if the patient is elderly.”
“WE CANNOT JUST OPEN UP”
Singapore's healthcare system is currently "stressed, but it has not been overwhelmed", said Dr Puthucheary. This is unlike the situation last year in many countries which experienced "excess mortality" and patients had to be turned away, he said.
"Excess mortality is when a lot more people than you expect die in a year, he said. "We are trying hard to avoid that, by keeping restrictions tight last year when our population was vulnerable to the disease, and then cautiously opening up after we vaccinated the vast majority of our population."
Although Singapore is trying to live with COVID-19, it "cannot just open up" and risk having cases shoot up, said Dr Puthucheary.
“We are trying to get to the point where the combination of high vaccination rates, booster jabs and even more boosting from mild infections means that COVID-19 will no longer spread as an epidemic in Singapore. And we are trying to get there without excess mortality,” he added.
“In other words, though we will have fatalities as a result of COVID-19, we will not see more overall deaths than we would in a normal non-COVID year. Nearly every other country that has arrived at that destination has paid a high price in lives.”
More cases will result in more ICU beds being used. Beyond a certain point, that will “force us to accept a lower standard of care” and result in more deaths that could have been prevented, said Dr Puthucheary.
“If despite our caution, ICU cases rise sharply, we will still do our very best to look after every patient. But at what level of care? I would strongly prefer if we can avoid that dreadful scenario,” he added.
“We need to continue to manage the overall number of cases in our population, even as we continue to increase our hospital capacity.”
“THERE IS HOPE”
Nonetheless, Dr Puthucheary acknowledged that "there is hope", calling on everyone to do their part.
“MOH and the healthcare teams will continue to train staff, increase beds and expand ICU capacity, he said.
“All of us can continue to play our part. Vaccination remains critical, every single extra person who gets vaccinated makes a difference, to themselves and for all of us. Getting your booster shot as soon as you are eligible makes a difference,” he added.
“Following the safe management measures makes a difference. Regular testing makes a difference. Using the right health care resources appropriately makes a difference.”
The current situation will “not last forever”, added Dr Puthucheary.
“Eventually enough of us will be vaccinated or will have been infected, that we will see the case numbers come down and the situation stabilise. But in getting there, we should try to keep the number of deaths as low as possible.”
He stressed that having one of the lowest fatality rates in the world is “a small miracle”, which didn’t happen by chance.
“It happened because Singaporeans stood together, looked out for each other, did their duty, and put the interests of others ahead of their own," he said. "And the healthcare workers of Singapore have done all this and much much more, caring for us all.”

MANDATORY VACCINATION "SHOULD BE CAREFULLY CONSIDERED"
In response to Dr Puthucheary’s ministerial statement, several MPs raised questions about Singapore’s COVID-19 efforts thus far.
MP Lim Wee Kiak (PAP-Sembawang) asked if there were plans to make vaccination compulsory for the population.
"Making COVID-19 vaccinations compulsory is a significant (move); it should be carefully considered," said Dr Puthucheary.
There are a few factors that would need to be considered, such as the vaccine coverage, international practice and the availability and performance of fully registered COVID-19 vaccines.
"In terms of making a mandate compulsory, it is also quite difficult in terms of the execution. You can imagine that for something like childhood vaccines, you may say that you can't have access to playgroups or certain school environments and so forth. There is a specific thing that you need to do or that you want to do, and for that you're getting the vaccine," said Dr Puthucheary.
"But really, here we're talking about all the normal activities of life. And so policing it, executing it, implementing it is not without challenges. And the question is how much benefit will there be? So I think it's something to consider, but there are a whole lot of complications associated with that."
LOOSEN MEASURES, INCREASE DINE-IN CAPACITY
MP Yip Hon Weng (PAP-Yio Chu Kang) asked whether the Health Ministry would consider “loosening safe management measures for the rest of the country”, if seniors who are unvaccinated and more susceptible to COVID-19 are identified and isolated.
“In a way, that is what we are trying to do with our (vaccination) differentiated measures. Expose some people to a lower level of risk, while allowing other parts of our population to do the things that make life a bit more bearable. But there's only so far that we can go,” said Dr Puthucheary.
Even someone who is senior, unwell and unvaccinated “can’t be locked up and isolated completely”. They need fresh air, food and contact with other people, he added.
“It's part of our human response. Our grandparents want to see their grandkids. We want to go and look after our parents. And each of those interactions poses a very small but measurable risk to them as well.”
As a result, the Government’s COVID-19 efforts, such as the vaccination-differentiated measures, “must treat the population as one”.
Leader of the Opposition Pritam Singh noted that there has been “significant public feedback” that dining-in capacity should be increased to five per group, instead of the current two per group ruling.
He added that since the Government is opening up more vaccinated travel lanes (VTLs), “there is a view that can’t quite connect” why dining-in capacity cannot be increased.
“We wish to get there ... We were even at eight at one point. It is important to the F&B industry, it is important to Singaporeans. It's important for families to get together. But I think the time is not yet,” replied Health Minister Ong Ye Kung.
“Because when you (group) in fives, as explained by SMS (Senior Minister of State) Janil, you do increase risk of transmission.
"If it’s transmission within vaccinated individuals, it may not be that serious. But we also live with older people, with seniors who may be unvaccinated, and we can inadvertently bring the virus to them."
Mr Ong acknowledged the comparison between opening VTLs but restricting dine-in capacity.
"The difference is this: That in the initial stage, Singapore has very low infections, and around us and around the world, have very high infection rates. So when you open up borders at that time, you're opening up the floodgates," he said.
"Today, the situation is entirely different. Our infection rates and the outside infection rates are similar. And in fact, they may be lower than us because they went through huge waves. And we are still going through ours. Furthermore, we limit travel or SHN-free travel to only vaccinated individuals. And at the border, you're subjected to tests."
However, Mr Ong added that theoretically, having a bigger event, like a wedding, where everyone is subjected to tests, is a "similar concept" to dining in fives.
"So I think this also presents possibilities ... for the MTF to think about, whether through tests, through vaccination, we can allow gatherings that are a bit more free."
BOOKMARK THIS: Our comprehensive coverage of the COVID-19 pandemic and its developments
Download our app or subscribe to our Telegram channel for the latest updates on the coronavirus pandemic: https://cna.asia/telegram