'I was going to die': Unvaccinated COVID-19 patient urges others to get jabbed after near-death experience
Lee Sock Lee, a 43-year-old mother of four, was unvaccinated when she caught the coronavirus, and her condition deteriorated quickly after she received a positive ART result.

Mdm Lee Sock Lee urged others to get vaccinated, and hopes they can learn from her experience with the coronavirus. (Photo: Marcus Mark Ramos)
SINGAPORE: When Mdm Lee Sock Lee tested positive for COVID-19 using a self-administered antigen rapid test (ART) kit on the morning of Sep 13, she had no idea that a near-death experience was looming.
Although she was unvaccinated, the 43-year-old was relatively young and had no pre-existing health conditions.
She tested herself for COVID-19 because she felt tired and fatigued for a few days. After a positive result from the ART kit, she walked to a nearby swab and send home clinic with her husband to take a polymerase chain reaction (PCR) test.
She thought she would only get mild symptoms from her bout with the disease.
"Most people have mild symptoms. I know I'm not vaccinated, but I did follow through with all the precautions and stuff like that. I have no pre-existing medical conditions, so I didn't believe I would be so sick," she said, speaking to journalists on Thursday (Oct 28).
"I wasn't aware I was so badly ill. I wasn't aware I was going to die."
But less than 24 hours later, she was lying unconscious in the hospital on life support because her heart was failing.
ON THE VERGE OF CARDIAC ARREST
Mdm Lee barely remembers anything after she was taken to Ng Teng Fong General Hospital in an ambulance from the clinic. One of her last memories on the way to hospital was calling her husband to settle some financial issues.
"I (also) recall a conversation between the hospital nurse and the ambulance paramedic. After that it's kind of fuzzy, I was in and out," she added.
Doctors made the call to hook her up to an extracorporeal membrane oxygenation machine, or ECMO machine, which eventually saved her life.
The machine removes blood from the patient, removes carbon dioxide and adds oxygen, and then pumps the blood back in. This is a form of life support used for patients with heart or lung failure that can function as an artificial lung or heart.
There are just two ECMO sites in Singapore for adult patients, and one resides with the team at the National University Hospital (NUH).
Mdm Lee was referred to the team for ECMO support after she reached the emergency department at Ng Teng Fong hospital, when she was "on the verge of cardiovascular collapse", doctors said.
"She got worse clinically and had to be rushed to the intensive care unit (ICU). In the ICU, her condition worsened that she needed to be put on a ventilator," said Assistant Professor Ramanathan K R, senior consultant at the National University Heart Centre's department of cardiac thoracic and vascular surgery.
"And despite being put on a ventilator, her heart function was so poor that she started accumulating acids in her blood, to the point that despite being on medications for her so-called heart failure, the heart wouldn't improve."
On the verge of cardiac arrest, Mdm Lee's prognosis was bad, he added.
"She would have otherwise died, had it not been for ECMO. I think that ECMO was life-saving in her instance," said Asst Prof Ramanathan.
TREATMENT AND RECOVERY
A doctor on the team arrived at Ng Teng Fong hospital to put her on the ECMO machine soon after, and she was then transferred to NUH's ICU.
"We figured out that the heart was barely contracting, essentially the heart was beating very poorly, and the ECMO support was helping her meet the oxygen requirements for her body's tissues," said Asst Prof Ramanathan.
After some tests, the team concluded that her heart problem was a result of the COVID-19 infection, which is "quite rare", he added.
The ECMO machine needs a team to manage it, including specially trained intensive care nurses and physicians, and surgeons to put the machine in and take it off, said Associate Professor Graeme MacLaren, director of cardiothoracic intensive care at the National University Heart Centre.
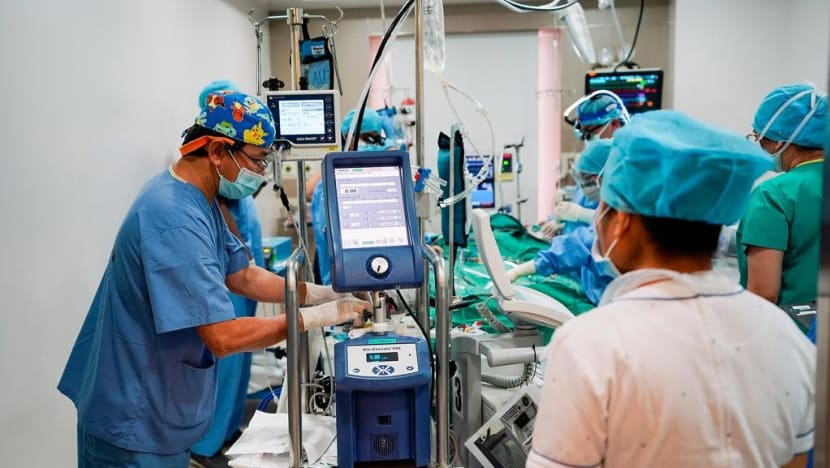
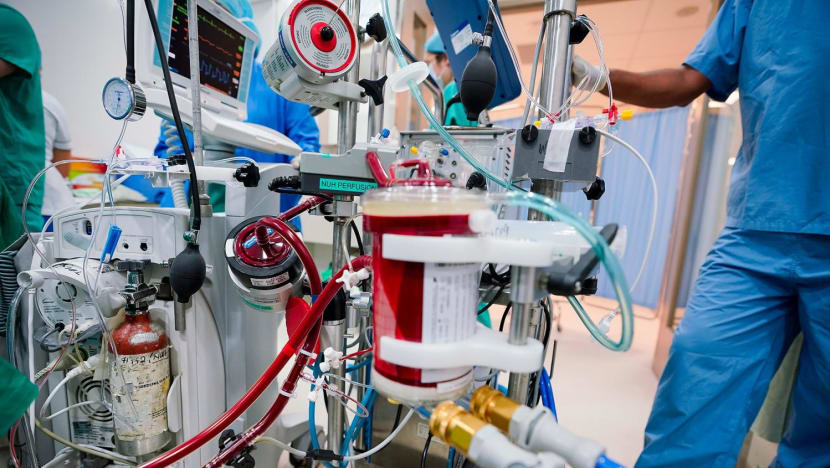
Mdm Lee remained on the ECMO machine for four days, as her heart started to recover.
The hospital continued to treat her for COVID-19, and she eventually regained consciousness on Sep 18; she stayed in hospital for a total of 22 days.
When she woke up, she coughed up a lot of blood in her phlegm. "Tissue after tissue, you see a lot of blood," she said.
Staying in the ICU also took a toll on her motor skills and functions, and she was unable to move around and do things herself.
"I can't really move and I had to relearn everything, even learning to swallow and eat," she said.
"I remember I asked for water because my throat was very dry, and they tried to give me one small teaspoon, 5ml, and I couldn't even swallow."
Mdm Lee, who is self-employed, also underwent speech therapy, physical therapy and occupational therapy to relearn how to eat, shower, walk, and do things like folding clothes, she recalled.
No one mentioned her treatment with the ECMO machine until she was much better, and she was "quite shocked" to hear about what happened to her.
"The nurses told me this is my second chance in life, especially those who witnessed how weak I was," said Mdm Lee.
"It was quite scary to learn that I almost died. Because if I died, I will only have my husband to take care of my four kids, and they are still very young.
"That was my immediate concern. If I had died, who would take care of my family? That was a very worrying and scary thought."
When she regained consciousness, the nurses asked Mdm Lee if she wanted to do a video call with her family, but she rejected the idea because she was still surrounded by tubes.
"I had phone calls with my husband before that, but I refused to do a video call with my children until I was left with maybe the feeding tube and the oxygen so it wouldn't scare them off," she added.
While she was in the hospital, her husband took care of their children as all five of them served out their isolation orders at home, supported by their families and neighbours.
They also did not tell their children about Mdm Lee's near-death experience in the hospital.
"When I did the first video call with my husband, he was hiding it but I can tell he was so relieved - he was crying," she said.
Mdm Lee will be going for her follow-up appointment with a cardiologist in November.
Her heart will be scanned to see how it has recovered or whether the scarring is persisting, which will impact her long-term recovery, said Assistant Professor Lin Weiqin, a consultant with the cardiology department.
"The heart can recover or it can remain weak. For Mdm Lee, she has recovered her heart function, that's very good," he added.
"But let's say you have a scar in your heart that doesn't go away with time, there's always a chance in the future this scarring can give problems," said Asst Prof Lin, adding that this depends on the size of the scar.

URGING OTHERS TO GET VACCINATED
At NUH, six COVID-19 patients have been put on the ECMO machine so far. All of them were unvaccinated, and one of them eventually died, the doctors said.
"That's primarily because the vaccine is protecting patients from getting very sick," said Assistant Professor Somani Jyoti, senior consultant with the hospital's infectious diseases division.
"We do have vaccinated patients in the ICU... but they are primarily older and their immunity has waned and they didn't have their boosters yet.
"But generally, vaccines are protecting patients from getting sick enough to really get to the point where they need to go to the ICU and certainly not to the point where they need ECMO."
She added: "ECMO is really the last ditch effort just to keep a patient alive, if they qualify."
Mdm Lee is the first COVID-19 patient who needed the ECMO machine for heart failure in Singapore, noted Assoc Prof MacLaren.
"I think it's something which is slightly worrying. You saw how fast she got sick. She woke up feeling fine, had a positive ART, and less than 24 hours later, she was on ECMO," he added.
"That severity of illness can be somewhat frightening for everybody, including healthcare workers."
Mdm Lee was initially hesitant to take the COVID-19 vaccine because she has severe seafood and drug allergies.
She had already booked her first dose of the Pfizer vaccine for Sep 10, but decided not to go in the end because she was not feeling well.
Aside from her ordeal, her husband and all four of their children, aged three to 13, all ended up testing positive for the virus.
Her oldest child is fully vaccinated, and her husband had taken one dose of the Pfizer vaccine the week before she was due to take hers.
All four of them had mild symptoms, like a slight fever and headaches. "But other than that, they were fine," Mdm Lee recalled.
Urging others to get vaccinated, she said she was motivated to share her story to help others learn from something from her ordeal.
"I would like to encourage everybody, if they can take the vaccine, please take the vaccine so they do not become seriously ill," Mdm Lee said.
"If they're not seriously ill we do not have to burden our doctors and nurses who have to work 12 hours or even longer just to take care of us," she added, recounting seeing doctors and nurses urging each other to take their long-overdue toilet or meal breaks during her stay in the hospital.
Unvaccinated patients who recover from COVID-19 are recommended to take a booster shot three months later, said Asst Prof Jyoti. Mdm Lee will be taking her booster shot in January.
She also cautioned others against thinking that severe COVID-19 illness would never happen to them.
"We really do not know how much our body can take the virus, and the virus from COVID is actually quite smart and quite interesting - there are a lot of variants," Mdm Lee said.
"Really do not take the chance, I would rather encourage everybody to just take the vaccine. If it can help lessen your symptoms and make you less sick, I think that is good enough."
BOOKMARK THIS: Our comprehensive coverage of the COVID-19 pandemic and its developments
Download our app or subscribe to our Telegram channel for the latest updates on the coronavirus pandemic: https://cna.asia/telegram














