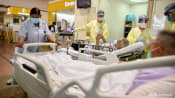
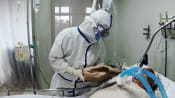
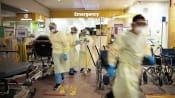
Why some healthcare workers in Singapore’s hospitals have quit — and others soldier on
The mental health of healthcare workers has recently been a topic of concern. Are things changing for the better? (File photo: iStock)
- Manpower shortage and lack of protected time off amid the pandemic are key factors that led to burnout.
- Those who left public hospitals also cited reasons beyond COVID-19, such as lack of recognition and protection against abuse.
- More nurses are turning to agency work, which one expert said could be a cause for concern.
- Salaries overseas are more competitive, and one foreign health professional said ‘it’s raining green cards for nurses’ in the US.
*Names have been changed.
SINGAPORE: It was early 2021. Lisa*, then a senior staff nurse at a public hospital in Singapore, received news that her father had contracted COVID-19 in Malaysia amid the Delta wave.
She would have gone home straight away, but her nurse manager’s response to her leave request shocked her.
“She told me that with the manpower shortage, I shouldn’t be so selfish and (should consider) my other colleagues,” said the Malaysian in her 30s who had worked here for 12 years at that point.
The hospital relented only when she said she would quit. She considers herself “very lucky” that she was granted a month’s no-pay leave: Eventually, her father’s condition deteriorated, and he needed intensive care.
“The saddest part about being in healthcare is when you spend so much time taking care of patients and their families, but you end up neglecting your own,” she said.
CNA Insider could not get the hospital to verify her account without identifying her. But she said it was the last straw in a series of events that had “drained” her. She realised that the long shift hours and lack of rest was taking a physical and mental toll.
She left the hospital last August but is still in public healthcare: At a polyclinic, where she works more regular hours. She is only the tip of the iceberg.
In November, the Ministry of Health (MOH) released statistics showing that about 1,500 healthcare workers resigned in the first half of last year, compared with 2,000 annually before the pandemic.
Last month, Senior Minister of State (Health) Koh Poh Koon elaborated on these numbers in Parliament: In 2019, the overall attrition in the healthcare workforce was 9.6 per cent. It dipped to 6.8 per cent in 2020, but then the two-year average attrition reached 9.8 per cent last year.
Two of the public healthcare clusters approached by CNA Insider did not share their attrition rate. The third, the National Healthcare Group (NHG), said last year’s rate was “higher than pre-COVID periods (2018 and 2019)” but “manageable”.
WHAT’S HAPPENING ON THE GROUND
But even as the Omicron wave wanes, healthcare workers CNA Insider spoke to say manpower shortage remains a concern.
More than 20 nurses, doctors and allied healthcare workers were interviewed and spoke on condition of anonymity, as they were not authorised to speak to the media.
About half of them had left their jobs in public and private acute hospitals or have tendered their resignation.
When James*, a mid-career nurse in a public hospital, tendered his resignation in January, he realised that at least five colleagues from his renal ward had done the same that month. Another nurse from the ward, whom CNA Insider spoke to, corroborated this.
The departures this year were “more pronounced” than last year, he felt. “(With) the third year of the pandemic, I guess most of them had enough. There was uncertainty over when their next break would come.”
A speech therapist in another public hospital said she has not seen this number of resignations in her 10 years there: This year alone, seven people in her department left, though not all owing to burnout or stress, she noted.
“Usually, about three, maximum four, people leave in a year,” she said.
Senior pharmacist Dean*, who has been in a public hospital setting for four years, said that in his section of about 150 staff, the resignations are most notable among pharmacy technicians. They number more than pharmacists and assist with pharmacy operations such as dispensing of medication and inventory-related matters.
About 30 to 40 per cent of them, mostly foreigners, left between the end of last year and early this year during the height of the Omicron wave, when the impact of departures was most acute, he said. Pharmacists like himself had to fill the gaps.
“Pre-COVID, if people left, (the hospital) would just hire people from overseas to replace them, so nobody really felt the pain. But with COVID and the borders closed, it wasn’t so easy to plug the holes,” he added.
For David*, a nurse in the emergency department with 10 years’ experience, the fact that experienced workers are quitting is a deeper concern than the numbers alone.
His colleague, Yvette*, agreed. “The need to retrain new nurses — which takes time — will increase the burden on the experienced ones, which gives these remaining experienced nurses even more of a push factor for leaving, like a vicious circle,” said the emergency doctor.
The mental health of healthcare workers has recently been a topic of concern across different platforms, from social media posts to authored studies.
In late February, an Instagram post from @thehonesthealthcareworker on how nurses were “not coping well” did the rounds. It said that the healthcare system was on a “slow road to collapse”, that working conditions have “worsened significantly” with no increase in practical support and that many workers were leaving.
The nurse-patient ratio has also increased “from 1:6 to 1:12 or more”, wrote the author, who later told CNA Insider he saw this happening in his hospital — although this could not be verified officially.
A study published in the same month by the Saw Swee Hock School of Public Health, Tan Tock Seng Hospital and the National Centre for Infectious Diseases highlighted the burnout brought on by overwork, emotional exhaustion and inability to take adequate leave as a “morale breaker” among healthcare workers.
There may also be pull factors at work, particularly among foreign nurses who may be attracted to other countries. According to MOH figures in Dr Koh’s parliamentary speech, last year’s attrition rate among foreign nurses was 14.8 per cent, double the 7.4 per cent among local nurses.
As the Omicron wave wanes and Singapore regains a semblance of normality, is there respite in sight to stem the flow, particularly for healthcare workers in acute hospitals? It may not be a given.
“It was never only about the pandemic,” said Tina*, a former senior staff nurse in her 30s who left her post in a renal ward at a public hospital. “This pandemic only brought more attention to healthcare workers and the issues we face at work.”
WHAT THEY’RE LEAVING FOR
Sunlight. That was the first thing that came to mind for Lisa when asked what marks her polyclinic job out from her previous one in an acute stroke unit.
“You’re always in the building throughout the day. You don’t get to see the little, simple things that tell you it’s going to be a good day,” she said, tears welling in her eyes at the memories.
She also worked night shifts (9pm to 8am). For every three of these shifts, she used to get a “sleeping day” to readjust her body clock, on top of her regular days off. But this was removed even before COVID-19.
“You didn’t get to rest and recharge before your next shift starts,” she said.
She often worked overtime. As a senior staff nurse, she oversaw 12 to 14 patients and had to manage complaints. She was also a clinical instructor mentoring nursing students.
Today, she often leaves work at 5.30pm. Her mood is “much better”, and she is “energised” for the day, she said.

Besides polyclinics, other job options for nurses include dialysis centres, nursing agencies, community nursing in long-term care settings like hospices, and lecturing in polytechnics or the Institute of Technical Education.
While facilities like HCA Hospice and the National Kidney Foundation Singapore said the number of nurses joining them has been “stable” over the past few years, three nursing agencies that recruit on a freelance basis cited an increase in applications.
Carelink Home Nursing Services estimated the increase at 40 per cent, compared with before the pandemic. Common reasons include flexible working schedules and more balanced pace of work, as well as higher compensation and recognition, said agency director Vikki Tan.
At caregiving start-up Homage, nurses can take up stints in various settings, whether in a home, community hospital or a facility. This is what James the mid-career nurse has done, citing the ability to have “more control” over his work.
“I try to achieve a bit more work-life balance … If I need more money, I’ll take on more jobs,” said James, who now also works at a private clinic.
This contrasts with his experience in a COVID-19 ward, where he was deployed in the early days of the pandemic and during the Delta and Omicron surges.
At one point, he was taking care of eight to 10 patients — his previous “worst-case scenario” was six to seven patients. After months of “repetitive” work and “this vicious cycle of non-stop working”, he reached “breaking point”, he said.
If this trend for nurses going to nursing agencies continues, there is cause for concern, said Associate Professor Jeremy Lim of the National University of Singapore’s Saw Swee Hock School of Public Health.
“Staffing becomes more difficult and expensive, which cascades into higher costs for patients and, potentially, safety issues due to staff turnover and unfamiliarity,” he said.
Higher pay outside public hospitals was a strong pull factor for some. Farez*, a staff nurse who left a general ward last August for a private dialysis clinic, said he is earning more while the workload is less.
“(People who quit) don’t feel like they were paid for the amount that they worked,” he said.
Occupational therapist Ryan*, who left public healthcare last month after six and a half years of service, was offered a 20 per cent pay increase in the private sector. He was also told he would be “chased home at 5.45pm”.
“I now see about 10 patients a day. I get to spend quality time with them. I’m able to relate better, understand their needs more thoroughly and assist them throughout the recovery process so much more,” he added.
Before he made the switch, his daily case numbers during the pandemic had risen to about “19 to 20”, as there were more elderly patients whose physical function “fell quite a bit” after they contracted COVID-19.
There are others who have quit just to rest. One of them is Tina, who has eight years’ experience. She said her patients’ growing demands, especially during the pandemic, had drained her.
For example, when visits were not allowed, her ward provided video calls as an “extra service” — which, in turn, patients “demanded”. “If we were busy, you had to wait a while. But there’d be people … shouting at us just to get the video-call phone to call their family,” she said.
She also felt recognition for nurses was lacking. Pandemic notwithstanding, Tina said she had patients asking her, “Do you even earn S$2,000 a month? You’re just a missy. You’re just wiping buttocks. Why do you need a degree for that?”

GOING OVERSEAS
Some healthcare workers are drawn to opportunities overseas, and even private hospitals are not immune. Filipino nurse Chris*, for example, left his private employer for the United States in April last year.
“It’s raining green cards for nurses,” he said, referring to the card that allows holders to live and work permanently in the US. It would have taken years to obtain before the pandemic, but it landed in his lap in less than a year, he added.
Two other Filipino nurses CNA Insider spoke to made similar points.
Chris loved his job here and Singapore too. He lived with his sister and had “a lot of opportunities” at the hospital he worked at — he said he was promoted every two years and was offered a scholarship.
But his application in 2013 for permanent residency was rejected — twice in his sister’s case.
In the US, Chris is paid thrice his salary in Singapore, has an apartment to himself and owns a car. When applying for a car loan, he noticed how different things were as a nurse in the US vis-a-vis Singapore.
“People here really appreciate nurses. They have high respect and high trust,” he said. According to him, even though he had no credit history, the moment he said he was a nurse, his loan was approved, no questions asked.
According to a Singapore Nursing Board report in 2019, Filipino nurses number about 7,600, or 18 per cent of Singapore’s nursing workforce.
Citing these figures in Parliament last July, Dr Koh said the MOH was working with healthcare employers to ensure the adequacy and sustainability of the nursing workforce. “Healthcare employers should also diversify their recruitment sources,” he added.
With greater competition for nurses worldwide, however, Assoc Prof Lim said Singapore would “remain uncompetitive” if it does not “unlock” the permanent residency and citizenship lever for foreign staff.
“If we don’t change, we then become the training stop for nurses,” he said. “(They) come here for a couple of years, get trained and then head to Australia or the United Kingdom.”
Last month, Dr Koh said the MOH is working on retaining foreign nurses by “keeping their remuneration competitive”. It has also worked with other agencies on “factors that are important for their retention”.

WHY THE REST ARE STAYING
Despite the overall challenges, many healthcare workers have soldiered on — together.
In her two and a half years in the oncology department of a public hospital, staff nurse Kelly* has had her share of bad days, but what has kept her going is her colleagues.
“That motivates me to come to work every time, knowing that I’m well supported by others working on a shift with me, regardless of the situation and demands of the day,” she said.
Sometimes they help to answer call bells from her patients on her behalf or start medications that doctors have ordered for her patients.
When manpower is lacking, especially with nurses coming down with COVID-19, her supervisors step out of their offices and work with them on the ground — helping with dressings and even feeding or showering the patients, she added.
This is a view echoed by Alex*, a medical officer in the emergency department of another public hospital.
“Sometimes when I’m unable to (fill in) a certain form or talk to a patient’s family, my nurses will say, ‘Don’t worry, I’ll help you.’ Or sometimes when nurses are busy and can’t check (patients’) blood pressure, I’ll tell them, ‘Don’t worry … I’ll do it,’” he said.
“Everybody is in one team helping to solve the problem … It’s a far nicer feeling than feeling isolated … facing all this shit yourself.”

Indeed, in the recent study on burnout cited above, many healthcare workers had mentioned being “motivated and inspired by strong leadership and supportive colleagues”.
Other morale boosters included having pride in being healthcare workers, and those on the front line expressed their appreciation for being thanked and supported at work.
This included kind words and tokens of appreciation distributed to all healthcare workers, as well as more tangible support such as the provision of interim staff housing and the ability to take consecutive days of leave once again.
The aim of the study was to explore the effects of Singapore’s pandemic response on healthcare workers’ morale and commitment, and to identify ways of enabling operational safety and functioning.
To this end, the researchers identified workers’ “stoic acceptance to fight, adjust and hold the line”, characterised mostly by a sense of devotion to service — “we have to work under such conditions” — and the expression or inference that “fear is for the weak”.
But the researchers concluded that this attitude, though necessary in the eye of the storm and indeed the biggest morale booster at the height of Singapore’s first COVID-19 wave, can last only so long before causing chronic and systemic problems, such as entrenched burnout.
Both Alex and Kelly attest that the latest wave has taken a toll. Kelly, for example, is “more burnt out than ever”.
“Imagine working tirelessly for five months and finally (taking) a week of leave, only to be called back four times during the week,” she said.
We’re allowed to reject those calls, but inevitably, I’d feel guilty about resting while my friends are working very hard to cover the shortage.”
WHAT’S BEING DONE
In response to CNA Insider’s queries about the attrition rate, manpower shortage and nurse-patient ratio, the MOH pointed to Dr Koh’s parliamentary speech last month.
The three public healthcare clusters, meanwhile, outlined efforts on the ground to retain staff and ensure their well-being.
The NHG said it aims to help staff achieve higher job satisfaction by automating manual tasks and empowering them to make decisions when redesigning roles. It added that it has stepped up efforts to monitor the well-being of staff, including their psychological health.
Staff at SingHealth have access to experienced medical social workers, counsellors and psychologists, coordinated by the SingHealth Staff Care Centre, “whenever they may feel distressed or simply want someone to talk to”, highlighted group chief human resource officer Esther Tan.
The cluster also has about 500 peer supporters who are “trained to extend emotional support to their fellow colleagues in times of need”.
The National University Health System (NUHS) has rolled out meetings in certain specialities whereby senior and junior staff can have “frank discussions about their emotions and feelings of vulnerability” in the clinical environment.
On the issue of leave, the NHG said staffing needs are managed through “advance planning and staggered rostering of leave”.
“This ensures that staff are able to go on leave by turns to rest and recharge or to return to their home country,” said Olivia Tay, its group chief human resource officer.
SingHealth, meanwhile, said the prevailing guidelines on overseas leave applications are largely “no different” from usual leave applications.
“As the Omicron situation in Singapore eases further, more staff will be able to resume some pattern of time away from work to rest and recharge, and for our foreign staff, the opportunity to return home to spend time with their families,” said Ms Tan.
As for recruitment, the NUHS is stepping up efforts locally and internationally, to “combat exhaustion”, and has introduced flexitime opportunities and part-time nursing schemes “where appropriate”.
Returning staff are also valued, said its group chief human resource officer, Priscilla Teo.
For example, some locum nurses who worked at its Community Care Facilities have joined the cluster full-time. There is also an “alternative workforce” comprising basic care assistants and student nurses who support its nurses in patient care.
At SingHealth, while recruitment efforts are in place, the cluster devotes “much more attention” to staff development, especially with the “insatiable global demand” for healthcare manpower.
LIGHT AT THE END OF THE TUNNEL?
Now with the Omicron wave waning, some healthcare workers said their working conditions have improved.
Janine*, a senior staff nurse in her 30s, told CNA Insider earlier this month that morale in her department, an intensive care unit, was “rather low”. But since then, things have started to look up — the lifting of restrictions has helped “in a big way”.
Some of her colleagues have taken leave and even travelled, including foreign colleagues off to see their families. “We have sufficient manpower now, so that means … no one’s getting a call back on their days off,” she said.
She had also been hoping that training opportunities would resume — in particular, courses to help her specialise in trauma. And she got her wish: Training sessions that were on hold for months have recently resumed.
In senior pharmacist Dean’s case, while the COVID-19 workload is decreasing, there is little respite. Manpower has yet to be replaced, and patient cases and projects that were postponed over the past two years are coming back “fast and furious”.
Since January, he has been able to take up to two consecutive days off. Anything longer than that, he said, is subject to balloting. And overseas travel requires approval from his head of department.
Still, he remains hopeful and looks forward to a time when the manpower issues can be resolved.
As for doctors, those CNA Insider spoke to welcomed the recent news about a national wellness committee for junior doctors, which will review and recommend changes to existing healthcare practices and guidelines to improve the well-being of junior doctors.
Singapore Medical Council guidelines stipulate that junior doctors may work up to 80 hours a week. But surveys showed that 20 per cent of them exceeded this stipulation, possibly owing to “the nature of clinical work in certain departments or exigencies of service”, Dr Koh said last month.
Now that the ministry is involved, Terry*, a medical officer in the general medicine department of a public hospital, is “hopeful that the committee will make a difference”.
“But with regard to whether (the recommendations) will be adopted and whether they’ll be enforced properly … only time will tell,” he said.
He listed two things that would help significantly: Mandated rest days that are strictly enforced and a “nationwide effort to move away from 30-hour calls”. This refers to doctors having to stay through the night at the hospital after their shift and continue the next working day.
ONCE BITTEN, TWICE SHY
Those who have left acute hospitals, however, said it is unlikely that they will return. “It’s a fulfilling job, but the amount of recognition doesn’t reciprocate the amount of hard work,” said Tina.
With plans in the pipeline to start a family, Lisa, too, is unwilling to endure irregular hours and shift work once again. “The hours aren’t friendly to working mothers,” she said, adding that as her husband is also a nurse, it would mean days when they barely see each other.
Farez is another who is contented where he is, at the private dialysis clinic.
“I might go back only if the hospital has a better staff to patient ratio and more protection for nurses,” he said, highlighting multiple occasions of “verbal abuse” from patients as one of the triggers for his departure. Some allied healthcare workers CNA Insider spoke to echoed this view.
Indeed, the NUHS said that besides the workload and working hours, a “significant part of staff burnout” is due to abuse, in person and online, and that it has “increased measures to mitigate risks”, without elaborating on these protective measures.
One way to take this forward, suggested Assoc Prof Lim, is to “very publicly punish” the people who abuse healthcare professionals.
“Yes, you’re under emotional stress,” he said. “But so are the nurses, and so are the doctors. I think people can take a lot more when they feel that their bosses have their backs.”
Another way to improve matters is to raise wages, he added. “We agree that nursing, physiotherapy and so on create a lot of societal value — then society should be prepared to pay.”
Last year, the MOH announced a salary increase of up to 14 per cent for nurses in the public healthcare sector, phased over two years. For allied health professionals, pharmacists and administrative and ancillary staff, the increase was 3 to 7 per cent of their monthly base salaries last year.
What is important, stressed Assoc Prof Lim, is that nurses’ salaries be benchmarked to their peers in other essential public services.
“For new recruits to any profession, it’s not what you’re paid relative to three or five years ago if you’d been (in that profession),” he said. “It’s the opportunity cost: If I wasn’t in nursing, would I be a teacher?
“Is a nurse with 10 years’ experience similar to a police officer with 10 years’ experience? A Singapore Armed Forces officer? That’s the sort of equilibration we should be looking at.
“And if the pay goes up, respect goes up.”

In the meantime, he sees one other way to retain staff or entice those who have left to return: To increase public awareness of the “nobility of the profession”.
“It’s not that people don’t want to be nurses. People want to save lives (and) do good,” he said.
“How do we, as a society, make it easy for people to do the right thing and sign up for the caring professions? Because, trust me, we and our families will need to use the health system.”
For folks like Kelly, there is still job satisfaction. “Nursing is my passion, and I’ve never regretted joining the industry,” she said.
“As cliched as it sounds, I chose this profession with the intention of helping others in need. And by doing so, it helps me keep … my humanity and humility.”