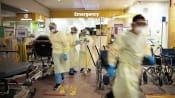
Healthcare workers describe struggles as patients flood emergency rooms amid Omicron wave
CNA speaks to public hospitals as well as four healthcare workers to get a sense of the situation on the ground as Singapore rides the Omicron wave.
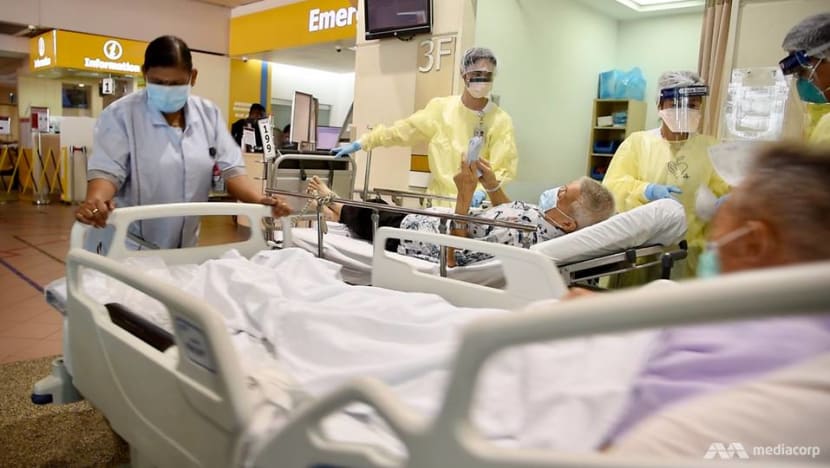
Patient care in the Emergency Department at Tan Tock Seng Hospital.
SINGAPORE: Stretchers filled with patients. Doctors and nurses testing positive for COVID-19. Long shifts with no toilet breaks. Fatigue.
Healthcare workers at several hospitals across Singapore are feeling the strain amid a flood of patients seeking treatment at emergency departments, leading to long queues and waiting time for a ward placement.
“It’s like Tetris blocks except it’s stretchers filled with patients,” said Jessica (not her real name), who works as a doctor at a public hospital.
“When you bring a patient in, you just have to find an empty spot to just push them there. It can be very confusing and hard to find them sometimes because it’s just so crowded, so we end up having to shout their names to try and find them,” she added.
Healthcare workers interviewed for this story were not identified as they were not authorised to speak to the media.
Over the past week, hospitals across the island said they have seen a higher number of patients seeking medical attention at their emergency rooms.
Khoo Teck Puat Hospital told CNA that the average daily attendance at its emergency department rose by 20 per cent in the first week of February compared with January.
Of the patients who walked into its emergency room that week, 66 per cent were discharged without being hospitalised, said its spokesperson.
At Singapore General Hospital (SGH), the emergency department is seeing a “higher than usual” daily patient average than in the past two years, said Associate Professor Kenneth Tan, head and senior consultant at SGH’s emergency medicine department.
Patients with symptoms of acute respiratory infections doubled during and after the first two days of Chinese New Year, of which more than 60 per cent were either eligible for the home recovery programme, sent to isolation facilities in the community, or discharged after their visit.
The Ministry of Health (MOH) over the weekend urged the public to seek emergency treatment at hospitals only for serious or life-threatening emergencies, amid a rise in the number of such patients.
Most of the patients who visited hospital emergency departments in recent weeks did not require emergency care, it added.
Hospitals that CNA spoke to urged patients with mild symptoms to visit their nearest clinics instead of jamming up emergency departments.
“Only people with serious or life-threatening emergencies, such as chest pain, breathlessness and uncontrollable bleeding, should visit the hospital’s emergency department as this allows those in need of emergency care to be attended to quickly and helps to preserve the hospital’s capacity for those who truly need acute hospital care,” said Associate Professor Thomas Loh, group chairman of the medical board for the National University Health System (NUHS).
NUHS manages National University Hospital (NUH), Ng Teng Fong General Hospital and Alexandra Hospital.
INCREASED WAITING TIMES
Emergency department staff that CNA spoke to said waiting times have increased by at least 20 minutes to a few hours for mild cases. In some instances, patients have had to wait as long as 20 hours to get a placement in a ward.
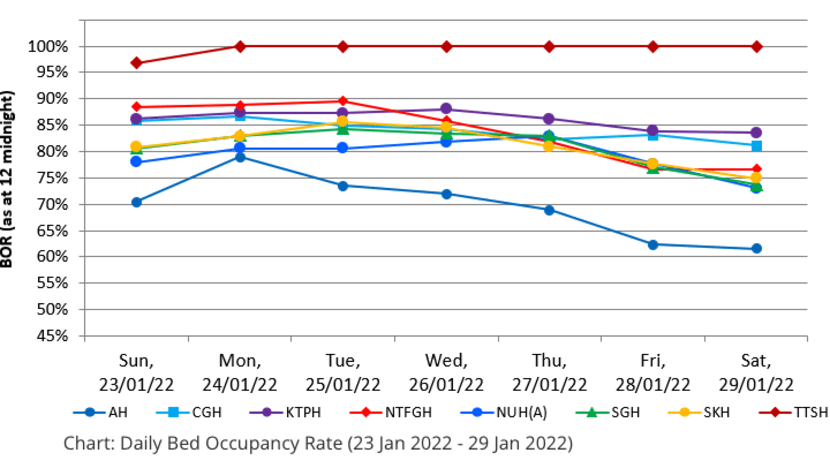
Among hospitals tracked by the Ministry of Health (MOH), latest figures show that daily bed occupancy rates ranged from 61.5 per cent to 100 per cent between Jan 23 and 29.
“It’s just chaos, with all the patients just waiting there and hospital staff members having to run around to check on everybody, while trying to keep up with the incoming patients,” said Ada (not her real name), a doctor who works at an accident and emergency (A&E) department in a public hospital.
With space filled up inside the A&E department, it is also common to see a large pool of people waiting outside to get updates on their family members.
“It’s very overwhelming,” said Jessica.
“Whenever I go out ... everyone is looking at me and asking if their family member is my patient and whether I have updates for them,” she added.
MORE PEOPLE TESTING POSITIVE FOR COVID-19
The growing strain on hospital emergency rooms comes as community infection rates continue to rise amid the Omicron wave.
Singapore reported 10,686 new community COVID-19 cases on Thursday, the third day in a row that daily cases came in above the 10,000 mark. The weekly infection growth rate jumped to 2.26, up from 2.0 on Wednesday.
A total of 1,212 COVID-19 patients are currently in hospital.
A&E doctors CNA spoke to said they have seen the number of COVID-19 walk-ins at their hospitals more than double, some of whom have mild or no symptoms.
“They are only coming in because they tested positive on their antigen rapid test (ART) self-test, or they might have something very minor like a runny nose or slight fever,” said Ada (not her real name), a doctor working at a public hospital.
Under current health protocols, those who are well but test positive for COVID-19 are required to isolate at home for at least 72 hours, and can exit isolation once they test negative on their self-administered test and are feeling well.
As for those who are not feeling well and require COVID-19 testing, they can visit Public Health Preparedness Clinics (PHPC) for further assessment.
However, with many general practitioner (GP) clinics closed during the Chinese New Year period, hospitals said this might have resulted in more people turning to emergency departments.
"Generally, after long public holidays such as Chinese New Year, our hospital tends to experience a higher number of admissions," said a spokesperson for Tan Tock Seng Hospital (TTSH).
With reduced GP operations and people seeking medical attention only after the festivities, coupled with the surge in COVID-19 transmission, the hospital is seeing more patients at its emergency department.
"This is a trend seen annually," the spokesperson added.
HOW HOSPITALS ARE RESPONDING
To cope with the surge in cases, some hospitals have set up additional waiting areas at their emergency departments or hired extra manpower.
At SGH, locums have been hired to augment the manpower at its emergency department.
This is to ensure that there is no compromise to patient care, said SGH’s Assoc Prof Tan.
Meanwhile, NUH’s children’s emergency department and the NUHS hospitals have redeployed staff and increased manpower to support their emergency departments.
The hospitals are also referring stable patients to home recovery or community sites like COVID-19 treatment facilities where appropriate.
NUHS has set aside existing beds that can potentially be converted to isolation beds for COVID-19 cases, as well as more holding facilities for suspected cases waiting for their results, said Assoc Prof Loh.
“There are also dedicated facilities and manpower to support the care of COVID-19 patients. We are also offering alternative arrangements where clinically appropriate, including teleconsultation, tele-rehabilitation, tele-monitoring, remote prescribing, and delivery of medication,” he added.
At NUH's children emergency department, the team is also taking on extra shifts to augment shortfalls where needed, said Professor Lee Yung Seng, head of the Khoo Teck Puat - National University Children's Medical Institute.
John (not his real name), a doctor in the children’s emergency department in a public hospital, said most emergency departments in Singapore have set up a temporary tentage area because there is no capacity for the additional patients within the building.
“Everything inside there looks very rudimentary. The laptops are temporary, the fax machine is temporary. And then now we’re seeing a huge number of patients in this area, it just looks very… not something you’d expect in a country like this,” he said.
“This surge should’ve been seen coming. The resource allocation has been dismal."
Rachel (not her real name), a nurse at a public hospital, said all the rooms in the emergency department where she works at are always occupied and manpower is stretched.
To cope with the inflow, the hospital set up an open area for mild and suspected COVID-19 cases.
She said that when it was first set up, there was just one nurse manning the area with about 30 patients. Now there are about three healthcare workers manning the area, which can hold up to 50 patients.
“It’s not an ideal ratio, it’s very stretched. My other colleagues from other areas will come and help but ultimately if they have their own patients in their area they still have to go back,” she said.
She also said that she has seen more doctors and nurses test positive for COVID-19 themselves, leading to a further shortage in staff.
“Quite a few of my colleagues tested ART positive. If they’re ART positive, they also have to be quarantined at home or in the isolation facilities. Because of that, we have quite a number of staff down,” she said.
Hospital protocols have also been in a constant state of flux, leading to confusion among healthcare workers themselves, said John.
“I lose track also. We just wait for our department’s bulletins on the official workflow and just follow that on a day-to-day basis,” he said.
OMICRON VS DELTA
Despite climbing infections, Jessica noted that the proportion of COVID-19 patients developing severe illness at her hospital appears to be lower than what was observed during the height of the Delta wave in October last year.
When CNA interviewed her last year, Jessica - who works in the COVID-19 ward at her hospital - had described being pushed to her limits, with the situation so bad that she had to work for three weeks straight with no breaks.
“If you compare the Delta wave to the Omicron wave, it’s slightly better because the proportion of patients who become so ill that they need ICU care is (lower),” she said. “It's an important distinction because you can have some severe symptoms, but you're well enough to be the general ward.”
“The concern is always ICU capacity. It’s a problem (if it gets too full) because that requires very specialised care, and not every doctor or nurse can do ICU,” she said.
“When it becomes too full, you have to get other doctors and nurses to come in, and that's when the standard of healthcare really starts to drop and people may die.”
BURNT OUT
More than two years into the pandemic, the current wave of infections is adding to the strains on healthcare workers, who are already exhausted and burnt out, they said.
“We've seen huge loss in nursing manpower and I can see my colleagues are struggling because (nurses) now have to take care of 12 patients each, which is double of what they used to handle,” said Jessica.
“They have to wear full personal protective equipment while doing a lot of physical tasks like walking patients to the bathroom or feeding them, so you can imagine how hard it is to do that for so many patients, ” she said.
“Sometimes the nurses may not have time to change a patient’s diaper or help them go to the toilet because they are busy with another person, and that’s when they are accused of providing poor care and get harassed or shouted at by the patient.”
The constant stream of COVID-19 patients also means fewer opportunities for doctors like John to see other kinds of patients who come to the emergency department, compromising on their training.
“This adds to the whole feeling that we’re burnt out. There’s also a lot of talk about everyone just saying they want to quit, because the opportunities outside are so much better,” he said, adding that many of his colleagues have already left the hospital.
His sentiments were echoed by other doctors CNA spoke to, who shared experiences such as working up to 13 hours with no toilet breaks or having only a few minutes to grab something to eat.
“I’ve been on the frontline for nearly two years, so I’ve gained a lot of experience and feel more confident in managing the medical aspect of it now,” said Jessica.
“But that doesn't take away the physical nature of a job and how fatigued you can get.”
BOOKMARK THIS: Our comprehensive coverage of the COVID-19 pandemic and its developments
Download our app or subscribe to our Telegram channel for the latest updates on the coronavirus pandemic: https://cna.asia/telegram