Commentary: How to live with long COVID if we don’t understand it?
Much is unknown about the long term effects of a COVID-19 infection, but new research continues to emerge at an unparalleled pace, say David Matchar and Emily Matchar.

SINGAPORE: There are surging cases, concerns about ICU bed shortages, the constant threat of new variants and vaccination stragglers, not to mention ever changing restrictions and economic woes for the last 20 months.
As if COVID-19 has not given us enough to worry about, we must also now focus our attention on its long-term effects.
Commonly referred to as “long COVID,” these most often present themselves some time after a patient recovers as fatigue, headache, memory difficulty and shortness of breath but could also lead to diarrhoea, rashes and even changes in menstrual cycles.
Long COVID can be debilitating even when the original infection was asymptomatic or mild. It can last for months, to the point that afflicted patients don’t really feel like they have recovered at all.
Worse, since some long COVID symptoms are also common among people who have never been infected, they could be easily missed or dismissed.
With the recent surge in community cases, including about 100 cases daily among those aged 18 years and below, this is especially frustrating for parents with children who experience difficulties after a COVID-19 infection.
MUCH WE DON’T KNOW
Having a better understanding of long COVID can help us learn to live with it. So, what causes long COVID and how common is it? The short answer: We are not sure.

Different estimates put the prevalence of long COVID anywhere from less than 1 per cent to nearly 70 per cent.
A study by the National Centre for Infectious Diseases (NCID) last year found that one in 10 recovered patients in Singapore had persistent symptoms even after six months. But since the study was conducted before vaccines were widely available and the Delta variant reached our shores, these numbers will likely change over time.
One major challenge is that there is no standard definition and diagnostic test for long COVID. Most medical providers consider a patient to have long COVID when they’re still unwell three months after their initial infection.
Medical staff employ a wide variety of responses to long COVID, including multiple diagnostic studies and best-guess treatments of uncertain effectiveness and cost. Treatments depend on symptoms, and may include respiratory therapy, physical therapy, medication and counselling.
But since reported symptoms can vary so widely, it’s hard to know which can be attributed to infection or to the isolation and stress of the pandemic itself.
Some symptoms may be effects of the initial COVID-19 infection, such as shortness of breath from residual lung damage or loss of sense of smell from effects on the nerves and brain.
But other symptoms can be seemingly unrelated. Many researchers suspect an overactive immune system may continue attacking the body even after the initial infection clears up.
What does the data say about COVID-19 booster shots and why the mixed scientific views? Experts weigh in:
Some suggest fragments of virus may “hide” in the body, causing an inflammatory reaction. Genetic factors and stress could also be part of the picture.
WHAT WE DO KNOW
But what we do know can already inform some current policies and actions.
We know that vaccinated people are less likely to get long COVID, even if it remains possible.
One study in Israel suggests that only about 5 per cent of people with breakthrough infections report long COVID. Some studies, including in the United Kingdom, suggest vaccinated individuals are half as likely as unvaccinated ones to report long COVID symptoms.
Thankfully, children are less likely than adults to contract COVID-19 and are dramatically less likely than adults to become severely ill. Children under the age of 12 account for 0.6 per cent of all local cases and none have developed serious illness requiring oxygen supplementation or ICU care so far, according to the Ministry of Health.
But they are not immune from long COVID. UK data suggests that 7.4 per cent of children aged 2 to 11 and 8.2 per cent of those aged 12 to 16 report continued symptoms after their initial illnesses.
What is clear is that vaccination is effective in reducing COVID-19 infection - in addition to reducing the severity and lethality of the infection. Vaccination also reduces the risk that breakthrough infection will lead to long COVID. So, Singapore’s high vaccination coverage is a hopeful sign.
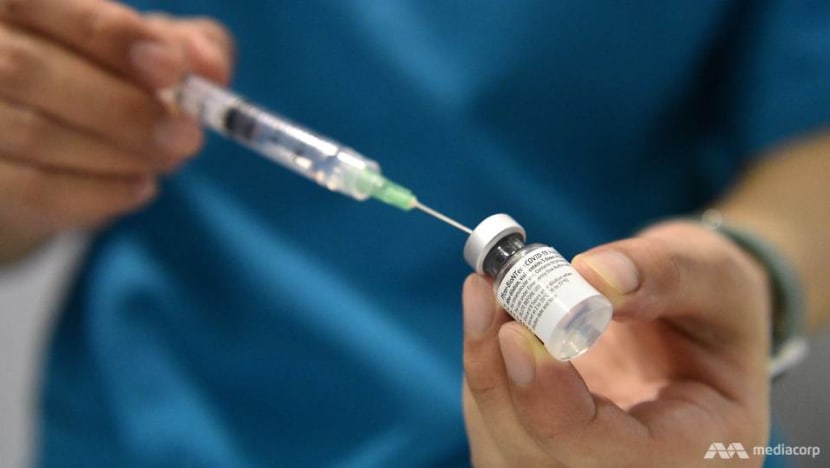
Interestingly, some unvaccinated people with long COVID report their symptoms improve after vaccination. According to a UK survey of more than 800 people with long COVID by a patient advocacy group, 57 per cent experienced an improvement in symptoms after the first vaccine dose.
A WAY FORWARD
Singapore is preparing to live normally with an endemic COVID-19. Such plans should include means to build up the healthcare system and community resilience against the long tail of COVID-19 infection as a matter of good clinical care and public health.
Aggressive efforts are needed to understand long COVID and to develop treatments to alleviate its effects. The healthcare community must develop basic guidelines on how to care for individuals with symptoms, including support for their psychological and social well-being.
Access to specialty clinics for individuals with prolonged and severe long-term symptoms should be provided, so healthcare staff can better evaluate and treat patients, and in the course of documenting their recovery, inform research into the causes and treatment of long COVID.
There are examples of healthcare organisations setting up clinics specifically attending to the needs of individuals with long COVID that can serve as models.
In the United States, grassroots groups have emerged to direct people towards dedicated post-COVID clinics, such as the Survivor Corps. Others, like the multisectoral COVID Patient Recovery Alliance, promote coordinated policy and research to inform national approaches.
Since June, Britain’s National Health Service has given funding to a number of specialist clinics to treat long COVID. Patients are referred by General Practitioners to these centres, where they are assessed by teams of doctors, nurses, physiotherapists and occupational therapists. They are then referred to the appropriate treatment and rehabilitation services.
Britain’s National Institute for Clinical Excellence has issued official guidance on best practice for diagnosing and treating patients with long COVID, which helps create consistency of care nationwide.
Here in Singapore, the Health Ministry has said it had not received reports of long COVID in November 2020. Its director of medical services Kenneth Mak told news outlets the NCID is studying the matter and following up with recovered cases from hospitals.
Long COVID may carry a silver lining - an opportunity to pay more attention to the issue of post-viral syndromes in general. The well-known chronic fatigue syndrome, also known as myalgic encephalomyelitis, may be caused by a virus in many cases.
Post-viral syndromes broadly describe fatigue, exercise intolerance, muscle pain, and cognitive difficulties following acute viral illnesses, and affect millions globally yet remain poorly understood.
While much is still unknown about long COVID, new insightful research is emerging at an unparalleled pace. As we prepare to live with COVID-19, the impetus to study long COVID may end up helping many more patients.
Dr David Matchar is a Professor at the Health Services and Systems Research Programme at Duke-NUS Medical School, Singapore. Ms Emily Matchar is a science writer based in Hong Kong.