Commentary: Dismissing those hesitant about COVID-19 vaccination as anti-vaxxers is short-sighted
Understanding the reasons behind vaccine hesitancy and what shapes these worldviews hold the best chance of changing people’s minds, say Edson C Tandoc Jr, Goh Zhang Hao and Kim Hye Kyung.

People walk during their lunch break in the financial business district of Raffles Place in Singapore on Jan 11, 2021. (Photo: AFP/Roslan RAHMAN)
SINGAPORE: Singapore has reached a target of getting 76 per cent of its population fully vaccinated against COVID-19.
With one of the highest vaccination rates in the world, it has also rolled out “vaccination-differentiated measures”.
Dining-in at restaurants has resumed capped at five per group — all diners too must be fully vaccinated. Those not fully vaccinated may be allowed entry if they have recovered from COVID-19 or tested negative within the last 24 hours.
These differentiated measures are meant to slow down the transmission of the virus and protect the unvaccinated who are more prone to getting seriously ill.
But they have also sparked debate: While some think them crucial, a few argue that differentiated measures run contrary to earlier declarations that vaccination will not be made mandatory.
TEMPTING TO DISMISS VACCINE HESITANCY
Indeed, despite the availability of COVID-19 vaccines in Singapore, some remain hesitant, while others refuse to get vaccinated.
For those who view getting vaccinated as a moral responsibility, it may be tempting to lump together all who are still refusing or holding off vaccination and regard them as being in the same group as notorious, ideological anti-vaxxer movements seen in countries like the United States or France.
However, even leaving aside those who cannot take the mRNA vaccines for medical reasons, deciding to get vaccinated may not be straightforward for some people.
Numerous academic studies have examined factors leading patients to comply with recommended treatments and procedures.
At the Centre for Information Integrity and the Internet (IN-cube) at Nanyang Technological University (NTU), we have collected survey data from 6,000 respondents across 10 cities in Asia, including Singapore, in early June, to understand vaccine attitudes in the region.
Of the 600 participants in Singapore, 287 were still unvaccinated. Of these unvaccinated participants, 61 per cent were willing to get vaccinated, 20 per cent were unsure, and 19 per cent were unwilling.
IDENTIFYING REASONS FOR VACCINE HESITANCY TO TACKLE CONCERNS
Our preliminary analyses find that being exposed to cues to action, such as messages encouraging people to get vaccinated, significantly increases the willingness to get vaccinated.
Cues originating from the government and health experts specifically are strongly related to willingness, more than reading about pro-vaccination messages on social media or in the news.
This is consistent with our earlier findings that exposure to health advisories on mask-wearing in the earlier stages of the pandemic in Singapore had increased public compliance, by informing individuals about how such actions curb the spread of the virus.
Believing that getting vaccinated will protect themselves and the community, or that vaccination is an easy process, also increases willingness to get vaccinated.
Those who perceive themselves as susceptible to COVID-19 are also more willing to get vaccinated. The recent spike in COVID-19 cases in Singapore and in many other countries may have increased perceptions of the severity of the COVID-19 threat and how vulnerable people are to the virus, nudging them to get vaccinated.
However, perceived barriers exert strong but negative effect on willingness. Those concerned over risks and dangers from getting vaccinated are less willing to go for vaccination.

A yet-to-be-vaccinated healthcare professional at a clinic we came across clarified that she was not against vaccination. She was simply afraid of the implications vaccination might have for someone like her with prediabetes.
PERSONAL NETWORKS SHAPE WORLDVIEWS
Interviews by our academic collaborators in the US with vaccine-hesitant individuals highlight the important role of interpersonal networks in reinforcing vaccine refusal. Some were concerned about the safety of available vaccines, citing conversations with family or friends that raised questions about the associated risks and dangers.
In Singapore, our preliminary analyses show those unsure or unwilling to get vaccinated tend to be older; they also consume news less frequently.
It is important to examine how the unwilling and the hesitant get information about COVID-19 vaccines. Some studies have demonstrated that vaccine-hesitant individuals are not necessarily uninformed — on the contrary, some of them obtain lots of information, hoping to resolve their hesitancy.
The more important question is where were they getting information about COVID-19 vaccines?
(Are COVID-19 vaccines still effective against new variants? And could these increase the risk of reinfection? Experts explain why COVID-19 could become a “chronic problem" on CNA's Heart of the Matter podcast.)
PROLIFERATION OF DIGITAL PLATFORMS A KEY CHALLENGE
Access to digital and social media has empowered users to actively select their information sources, and many individuals tend to gravitate to those providing reports consistent with prior beliefs.
For example, social media and messaging app groups have sprouted, where members contribute anecdotes of side effects and injuries supposedly incurred after vaccination against COVID-19.
But these anecdotes rarely include evidence and are difficult to verify due to anonymity - and yet they may be reinforcing the attitudes of some users against vaccination.
One such Telegram group based in Singapore we are studying has about 10,000 members
While some side effects have been documented by medical experts, they represent a tiny fraction of all those who got vaccinated and the majority of those vaccinated experienced mild or no side effects. And yet, reading one anecdote after another might skew the perception of some individuals that serious side effects are more commonplace.

Our survey also found that the unsure and unwilling also tend to come from lower-income households while the willing tend to have higher educational attainment.
Those unwilling to get vaccinated also have the lowest trust in the media, government institutions, and health experts — but of these three, they tend to trust health experts the most.
THE REAL ANTI-VAXXERS
In countries such as in the US, studies have found that the few individuals who hold deep-seated stances against vaccination are very difficult to persuade — this small group has voiced vehement, consistent refusals against any vaccination.
As countries race to reach herd immunity, vaccine refusal is starting to become a serious threat. The rise of the Delta variant, the impact of long COVID and the waning efficacy of vaccines over time all point to the importance of maintaining as high a vaccination rate as possible.
Anti-vaccination groups subscribe to false conspiracy theories about the dangers of vaccines, and the supposedly nefarious motives by governments and pharmaceutical companies.
In a previous study where we interviewed Singaporean parents reluctant to vaccinate their child against human papillomavirus (HPV), many revealed concerns associated with the novelty of the HPV vaccine.
Some parents, for example, highlighted the unknown side effects of vaccination in the long term. One parent shared a “wait-and-see” attitude, hoping that her child naturally benefits from the herd immunity without taking the risk of vaccination.
A similar uncertainty surrounding novel vaccines is present with COVID-19 vaccines, which were developed in a very short period.
TARGET STRATEGIES TO COUNTERACT VACCINE RELUCTANCE
More studies to understand this small segment of the population concerned about vaccination are needed to address refusal rather than to dismiss or shame such people outright as conspiracy theorists or uninformed “covidiots”.
Changing the attitudes of the vaccine-hesitant and vaccine-refusers is a challenging task when attempts to correcting strongly held beliefs can backfire.
Scientific studies have shown that pro-vaccine messages delivering facts and images of disease-sickened children can increase fears on the side effects of vaccine among parents. Using threatening or depressing images may inadvertently turn off and alienate people.
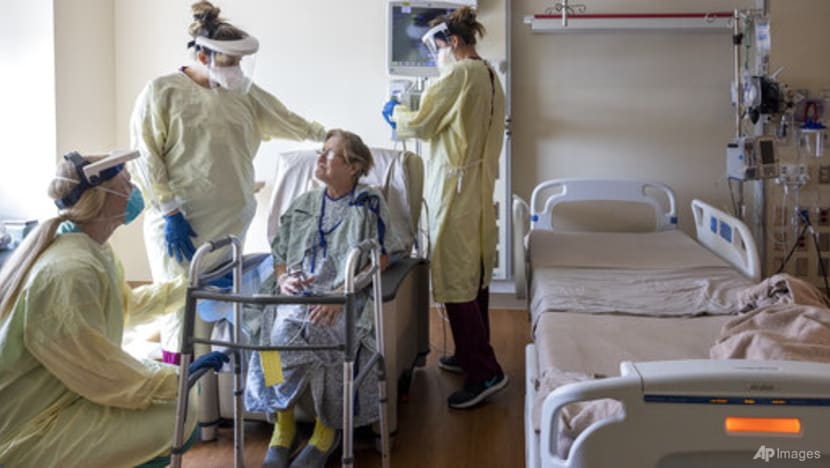
Vaccine advocates should appeal to these groups with caution and avoid mocking or downplaying their concerns over safety.
A slew of targeted strategies can be employed to counteract reluctance. First, enlist the help of physicians and family doctors as these health experts are among the most trusted, unbiased and apolitical source of information for this group of people. They should focus on reassuring patients of the safety of the vaccine.
Second, tackle contradictory messages that arise from health experts. These may also cause confusion and risk pushing the vaccine-hesitant to refrain from taking the vaccine. Encourage those with immunocompromised systems to see their own specialist to determine suitability for vaccination instead of listening to hearsay.
Scientists and medical experts too can be more proactive in engaging the public through social media, where anti-vaccination messages and conspiracy theories are circulating.
Third, the media should be careful when reporting cases of side effects supposedly caused by vaccination and avoid unnecessarily alarming the public.
There is a natural tendency for negative events to catch attention when the causal effects have not been investigated or established, such as the claim an 81-year-old here had died of an allergic reaction to the COVID-19 vaccination in April. The Ministry of Health clarified that the man died of heart disease and not because of the vaccine.
Videos from around the world linking vaccination to deaths have also gone viral and had to be corrected, but the resulting public fear over vaccines was hard to rectify.
In one example, a video circulating in January showed a young man in Israel supposedly fainting at a vaccination site with the caption alleging he died 15 minutes after receiving his second dose. Fact-checkers later verified the man was treated, sent home, and was alive.
Fourth, the Government should continue with messages highlighting the costs of not being vaccinated to both individuals and the community.
The vaccine-hesitant may internalise better the importance of vaccination by hearing personal stories of those who suffered from vaccine-preventable diseases.
This is one strategy many governments have adopted by making public information how many new COVID-19 cases have been vaccinated and how many have not, showing that not only do unvaccinated people account for the majority of new infections, but they also tend to be more seriously ill.
The differentiated measures being rolled out for those vaccinated and unvaccinated are also a type of nudge to get those who are not yet vaccinated to consider getting the vaccine.
Studies have demonstrated how providing incentives can encourage particular behaviours, and we will soon find out whether the differentiated measures for the vaccinated can get more of the unvaccinated to consider taking the vaccine.
Edson C Tandoc Jr is an Associate Professor at WKWSCI and the Director of the Centre for Information Integrity and the Internet (IN-cube).
Zhang Hao Goh is a Post-doctoral Research Fellow at IN-cube at WKWSCI specialising in human cognitive responses and their coping behaviours toward threats.
Kim Hye Kyung is an Assistant Professor at WKWSCI, specialising in health communications, and a collaborator for IN-cube.