commentary Commentary
Commentary: Variants versus vaccines is becoming the new COVID-19 race
New variants emerge from large, uncontrolled outbreaks. This is why vaccinating people is an urgent priority, says Duke-NUS Medical School’s Professor Gavin Smith.

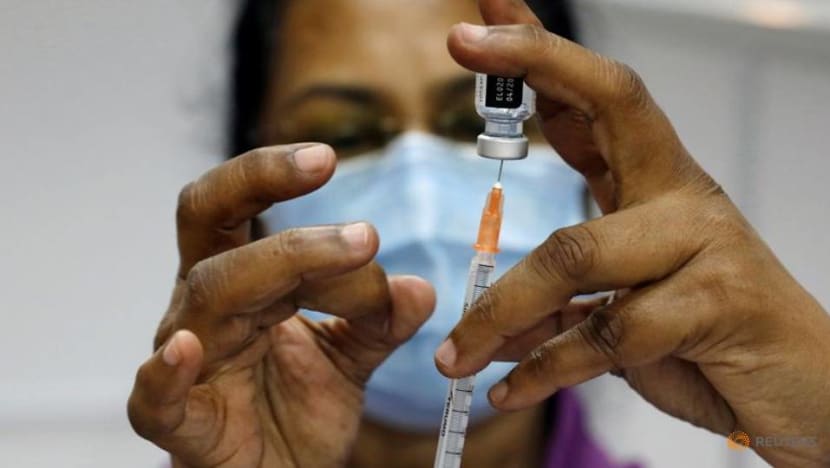
People wearing protective face masks while crossing a road on May 24, 2021, during Phase 2 (Heightened Alert). (File photo: Marcus Mark Ramos)
SINGAPORE: Variants of SARS-CoV-2, the virus that causes COVID-19, may be outpacing vaccination progress in many parts of the world, fuelling fears of new outbreaks.
Scientists around the world are tracking these variants to understand whether some spread faster than others, how they might affect our health and how effective current vaccines might be against them.
Evidence is now emerging that some mutations can make a virus spread more easily, while other mutations are associated with a reduction in how effective a vaccine might be in preventing infection.
But even if vaccine efficacy is lowered against certain variants, the vaccine will still protect against infection, hospitalisation and death.
Some variants are more deadly but others, like the B117 first identified in the UK, look the same as the parent in terms of fatality.
READ: Commentary: Some pain even as Singapore rises to the challenge of tighter COVID-19 measures
READ: Commentary: We have to live with an endemic COVID-19. Here's what that could look like
VARIANTS A NATURAL RESULT OF VIRUS EVOLUTION
Variants emerge because viruses like SARS-CoV-2 are constantly changing or mutating as a normal part of the virus’ evolution.
Mutations occur when the virus makes a mistake while copying itself (called replication) during an active infection. Most mutations have no effect on virus behaviour, but some can make the virus more transmissible.
For example, a mutation might allow the virus to grow better in the nose and throat compared to deep in the lungs.
You would expect the virus variant growing in the nose to be more easily spread because it is more likely to be expelled during sneezing and coughing.
This is just one example of how a mutation can change the behaviour of a virus, in this case transmissibility. But at the moment, we still can’t say much about the effects of most mutations we observe in SARS-CoV-2 with great certainty.
READ: Commentary: Why is COVID-19 surging in the world’s most vaccinated country?
SCIENTIFIC ACHIEVEMENTS IN SEQUENCING HELPS US DEAL WITH VARIANTS BETTER
The unprecedented amount of virus genome sequencing conducted in this pandemic, however, has been a major scientific achievement, giving us an overall view of how this virus is changing over time.
Since the start of the pandemic, more than 1.5 million SARS-CoV-2 genomes have been sequenced. To put this in context, during the first year of the 2009 influenza pandemic less than 10,000 genomes were produced and that was a huge achievement at that time.
The sequencing data provides an opportunity to scrutinise every small change in the virus genomes, and to identify variants through laboratory study and clinical correlation, though this alone can’t tell us what effect a mutation might have.
Out of all this sequencing data, the World Health Organisation (WHO) distinguishes Variants of Interest (VOI) if they show some sort of changed behaviour, such as causing more severe disease, or if they possess mutations known to change the nature of the virus, such as how easily the virus can be transmitted.
Variants must cause a community outbreak or circulate in multiple countries before they are flagged as a VOI.
A VOI gets upgraded to a Variant of Concern (VOC) if there is substantial evidence for higher virus transmission or virulence, or if there is an impact on vaccines and drugs used to treat COVID-19.
(Are COVID-19 vaccines still effective against new variants? And could these increase the risk of reinfection? Experts explain why COVID-19 could become a “chronic problem" on CNA's Heart of the Matter podcast.)
NEED TO CONTROL OUTBREAKS TO PREVENT MORE VARIANTS FROM EMERGING
Mutations occur naturally during an infection. Hence, it is unsurprising these variants of interest and concern have all emerged from large, uncontrolled outbreaks.
When a new virus enters humans with no existing immunity, the virus can run rampant, infecting millions of people.
This has happened in many countries, and we have seen new variants discovered in the United Kingdom, South Africa and the United States when they were experiencing unchecked epidemics, and more recently from Brazil, India and Vietnam.
We can expect to see more variants emerge over time before enough of the global population are vaccinated or immune from previous infection.
READ: Commentary: Why many under 45 are hoping vaccination slots open in June
READ: Commentary: New Yorkers are defying advice and keeping their masks on
The good news is that the vaccines are still working so far even against the new variants, and we can expect them to remain effective for the foreseeable future.
A recently published study shows that the Pfizer-BioNTech vaccine is still 88 per cent effective against the B16172 variant associated with the outbreak in India, down from 93 per cent effectiveness against the earlier B117 variant.
The effectiveness in preventing hospitalisation and death would be even higher.
CONTROLLING INFECTION THROUGH VACCINATION
The only way we can move out of this pandemic is when the population globally has some level of immunity against the SARS-COV-2 virus. There are two ways to achieve this – through natural infection or through vaccination.

Natural infection runs the risk of severe sickness and death. COVID-19 kills 2 per cent of infected people globally, which would equate to more than 100,000 people in Singapore. These numbers might seem small but imagine if one of those people was your loved one.
The good news is that we now have not just one but a whole range of safe and effective vaccines.
These vaccines represent our best chance of getting out of this pandemic without adding significantly to the estimated 3.5 million deaths that have occurred globally.
READ: Commentary: Booster shot for COVID-19 - not everyone needs it
READ: Commentary: Indonesia’s company-funded vaccination drive boosts the national rate but has limitations
While vaccines are very effective at preventing infection, in the event that a vaccinated person is infected, being vaccinated will protect him from dying or getting very sick and reduces the risk of transmission.
So the best way to stop new variants emerging is to stop people from getting infected. And currently the best chance we have to stop infection and reduce transmission is to get as many people vaccinated as quickly as possible.
Dr Gavin Smith is Programme Director (Interim) and Professor in the Emerging Infectious Diseases Programme at Duke-NUS Medical School Singapore.














