commentary Commentary
Commentary: Hard to grapple with dementia when early signs are often neglected
Most people with the illness don't get medical attention because they are not aware that they even have a problem, says one expert at the Institute for Mental Health
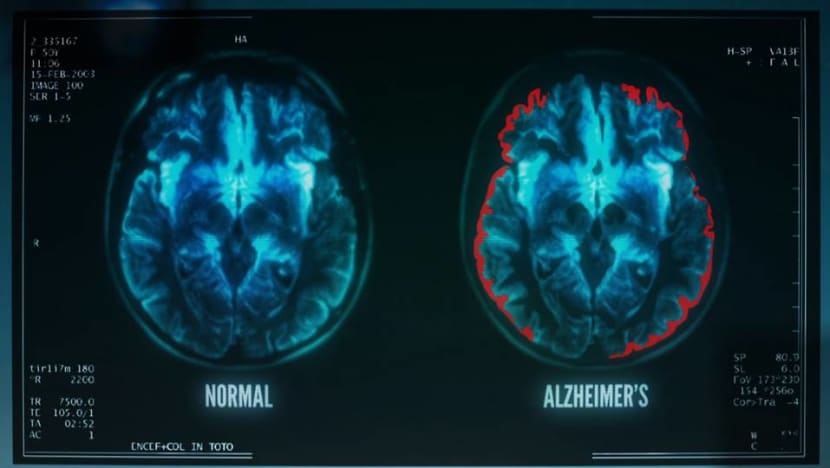
A screengrab from an episode of Channel NewsAsia's Talking Point, Alzheimer's At 46: Living With Young Onset Dementia. (Photo: Mediacorp)
SINGAPORE: The World Health Organisation (WHO) estimates that dementia currently affects 47 million people worldwide resulting in US$818 billion (S$1.12 trillion) in cost, which is mostly borne by the families of those affected. It is also the seventh leading cause of death in the world.
Last year, the WHO called for a global action plan on the public health response to dementia.
In Singapore, one in 10 elderly above the age of 60 has dementia, according to a Well-being of the Singapore Elderly (WiSE) study conducted by the Institute of Mental Health published in 2015.
READ: He’s 48, and already grappling with dementia
HELP IDENTIFY DEMENTIA EARLY
Dementia is a group of disorders which interferes with how the brain normally functions, with the most common and well-known being Alzheimer’s disease.
The severity of problems faced by a person with dementia directly correlates with the degree of damage to the brain cells.
So, identifying this condition early through a general practitioner or polyclinic doctor should become one of the priorities for an individual or their family. Early identification of dementia can help slow down the progression of the condition.
In the early stages, patients can make decisions, allowing healthcare professionals to involve them in the planning of their future care, address legal matters like making a will and drawing up a lasting power of attorney.
The latter enables the family to act as a legal deputy to safeguard the patient’s personal welfare, property and affairs as the condition progresses and he or she is unable to make decisions.
READ: Singaporeans plan our whole lives, so why not our deaths? A commentary

The medical community can also work with patients and caregivers on the support they require and link them up with resources in the community that they can tap on, like day care centres.
But most people with the illness do not come to medical attention as they are not aware that they have a problem, and may be contented with their situation. Some are just unwilling to go to the doctor for a check-up.
Their reluctance to accept help can cause a lot of stress for caregivers.
DEMENTIA CAN’T BE PREVENTED, BUT CAN BE DELAYED
I wish I could say that dementia can be prevented but the short answer is no, because the single most important risk factor for developing the disease is increasing age.
Compared to elderly aged 60 to 74 years, the likelihood of dementia for those aged 75 to 84 years is 4.3 times higher, and for those 85 years and above, it is 18.4 times higher.
But several things can delay the onset or slow down the progression.
Advice given for chronic diseases like diabetes, high blood pressure and cholesterol holds good for dementia as well. This includes adopting a healthy lifestyle with regular mental and physical exercises and a well-balanced diet, stopping smoking, reducing alcohol intake, reducing life stressors and improving the quality of social relationships.
It is also important to go for health checks at least once a year even if no medical problems are encountered and more frequently as suggested by the doctor for existing illnesses.

BEWARE DEPRESSION, PARANOIA, ANXIETY
People who suffer from dementia will become increasingly dependent on family members. They can develop depression and other psychological problems that include paranoia and anxiety.
They may also develop behavioural problems such as agitation, aggression, disinhibition, shouting and sleep disturbances.
If such behaviours are present then family members need to bring them to the attention of the doctors as early as possible as these symptoms tend to progress and can cause caregivers more stress.
Fortunately, most can be effectively managed with a package of care which includes medication, day care, structured routines and home help to assist in activities of daily living.
READ: Dementia caregivers put on a brave front – while watching loved ones fade away, a commentary.
KEEP DEMENTIA PATIENTS ACTIVE
All is not lost when someone is diagnosed with dementia. Keeping people with dementia occupied and engaged can help maintain their quality of life.
Learning a new skill can be difficult for them, so caregivers should encourage them to do things they are familiar with and keep up with daily activities.
If they used to enjoy doing crossword puzzles, get them to pick it up again. They may not be able to do complex puzzles like before, but they can try their hand at simpler ones.
Having a daily routine and sticking with it will also help both the patient and caregiver. Adapting to changes in routine requires the use of short-term memory, which is impaired for those with the condition so they’ll have a problem coping and may feel distressed and confused.

A LITTLE CAN GO A LONG WAY
Dementia is a chronic illness which progresses over several years, so timely support and assistance to the caregiver is of vital importance.
The patient may eventually need 24-hour care in a nursing home but this does not imply that the family has failed, but more a recognition that their care needs have progressed beyond what can be provided at home.
Even if the patient resides in a nursing home, this does not prevent the family from visiting and collaborating with the staff in providing optimum care.
The world is grappling with the problems of an ageing population including dementia.
There are international collaborations in research to find a drug to prevent dementia. Governments are building dementia-friendly communities. Hospitals are providing early diagnosis, treatments and advice on optimum care, and welfare organisations are providing help, advice and support to patients and caregivers.
However, each one of us can also make our own little contribution in combating this disease. In the end what really matters is the quality of life one has.
Dr Richard Goveas is consultant at the department of Geriatric Psychiatry at the Institute of Mental Health in Singapore.















