Attrition rate among local, foreign nurses in public sector went up between 2020 and 2021: MOH
The increase followed a drop between 2019 and 2020.

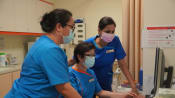
File photo of a nurse tending to a patient at a hospital in Singapore.
SINGAPORE: The attrition rate among local and foreign nurses in the public sector increased last year compared to 2020, Parliamentary Secretary for Health Rahayu Mahzam said in Parliament on Tuesday (Aug 2).
Among locals, the attrition was 7.4 per cent in 2021, up from 5.4 per cent the previous year. For foreign nurses, attrition more than doubled year on year to 14.8 per cent in 2021.
The increase in attrition rates followed a drop for both local and foreign nurses in the public sector between 2019 and 2020.
Attrition rate refers to the pace at which employees leave a company.
"For foreign public sector nurses, international competition has been more intense and attrition rate has increased more significantly," said Ms Rahayu, in her response to several questions on nurses and their welfare from MP Louis Ng (PAP-Nee Soon).
Responding to Mr Ng's question on a salary comparison between private and public hospital nurses, Ms Rahayu said: “We are reluctant to provide this so openly, as we know that both sectors compete for manpower.”
Ms Rahayu said that MOH does not have data for the private sector, although she provided some pay figures for staff nurses and senior staff nurses, who form the largest proportion of Singapore’s nursing workforce.
The median annual salaries for staff nurses ranged from S$42,800 to S$53,700 in 2017, and rose to between S$46,300 and S$58,500 in 2021.
For senior staff nurses, median annual salaries ranged from S$65,000 to S$79,700 in 2017, and increased to between S$71,200 to S$87,600 in 2021, Ms Rahayu said.
She added that in general, it takes an average of four to six years for a fresh graduate to move up to a senior staff nurse role. This means that an employee who was a staff nurse in 2017 may be drawing the annual salary in the senior staff nurse range by 2021.
The key issue is retention, Ms Rahayu said.
Outlining the strategy MOH has put in place to achieve this, she said the ministry reviews nurses' scope of work to enable them to spend more time on direct patient care and ensures remuneration is competitive locally and internationally.
In terms of scope of work, public healthcare institutions reduce the administrative workload by, for instance, introducing innovations in automation, technology, robotics and AI-enabled technology.
The ministry has also streamlined care processes and deployed dedicated administrative and support care staff to assist nurses, she added.
WELFARE OF NURSES
Mr Ng also asked if the National Wellness Committee for Junior Doctors could broaden its scope of work to include the working hours and conditions of nurses.
In response, Ms Rahayu said that issues related to junior doctors need to be tackled differently because of their regular rotations across the public healthcare system, compared to other employees who are hired directly by public healthcare clusters.
She noted that while the ministry does not impose a minimum number of rest hours, duty rosters for nurses are planned in advance to ensure staff have “adequate” rest between shifts.
“Even as we prioritise the well-being of our nurses, we appreciate the reality of their work, which is to deliver timely and quality patient care,” she said.
Mr Ng asked for a definition of adequate rest. He said that some nurses finished their shift at 9pm or 10pm and are back at work at 7am the next day, which, he pointed out, results in insufficient rest.
In response, Ms Rahayu said that there are many different arrangements within the public healthcare institutions on how they manage their employees' rest hours. In some clusters, rest is ensured through rotating shifts, she said.
However, she noted that the realities on the ground may be "challenging" and that nurses may have to go beyond their "call of duty".
MOH is working to ensure there are sufficient nurses on the ground, Ms Rahayu said, noting that the number of nurses over the past few years has remained stable.
Local nursing intakes have increased from about 1,500 in 2014 to about 2,100 in 2021, she noted.
Given the growing demands on healthcare manpower as the population ages, Ms Rahayu urged families and caregivers to be a partner in the care journey of their loved ones to alleviate workers’ workload.
“We understand the importance of recognising nurses’ contributions and the ministry has worked on reviewing their salaries and allowances,” she said.
Over the last five years, the annual salaries of local nurses in public healthcare institutions – which comprise base salary, allowances and bonuses – have increased, she noted.
She added that with the easing of COVID-19, public healthcare institutions have been allowing nurses to take time off work to rest and recover, including allowing foreign nurses to return home.
Data shows that leave is being approved and allowed, Ms Rahayu said.
“MOH remains committed to providing support to the public healthcare clusters in our efforts to ensure that there is sufficient manpower on the ground, and look after the well-being of our nurses as they continue to face pressures from COVID-19 surge waves and an ageing population,” she said.
Editor's note: An earlier version of this story said the attrition rate among local nurses was 7.4 per cent in 2012. The correct year should be 2021. We apologise for the error.