Eye injections help property agent to save her sight
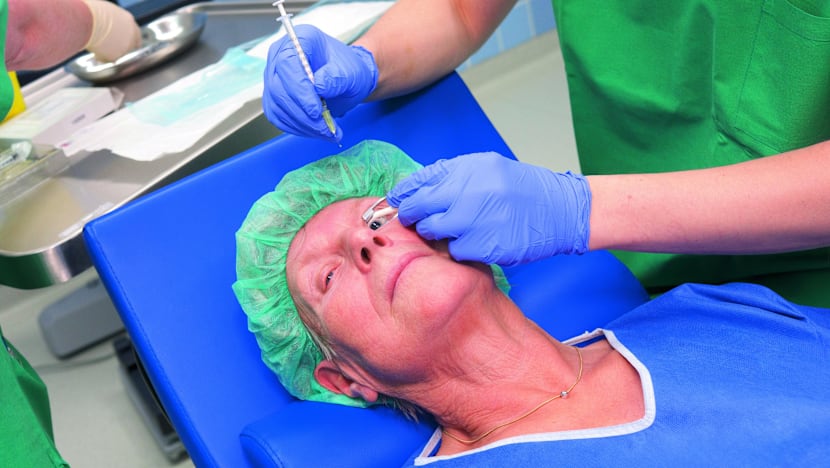
A patient about to receive an injection into the eye. Photo courtesy Bayer
SINGAPORE — Although she initially balked at the thought of “scary” injections in her right eye to treat age-related macular degeneration (AMD), the prospect of losing her sight was even more frightening for Ms Evelyn Yeo, 58.
The progressive eye condition is the leading cause of blindness in people over the age of 60.
Six months after she was diagnosed with AMD in 2016, the real estate agent enrolled in a clinical trial at the Singapore National Eye Centre (SNEC)’s Singapore Eye Research Institute to assess the efficacy and safety of a drug, which is injected into the fluid within the eye.
“Initially I was fearful and worried that my eyesight would be worse off with treatment than without it,” said Ms Yeo, who suffers from a subtype of “wet” macular degeneration known as polypoidal choroidal vasculopathy (PCV).
There are two basic types of AMD, wet and dry. Wet AMD occurs when abnormal blood vessels weakened by lesions or polyps leak fluid or blood into the macula (a small spot in the retina, the light-sensing nerve tissue at the back of the eye), causing vision deterioration, said Professor Wong Tien Yin, medical director and senior consultant ophthalmologist at the SNEC.
A genetic variant of AMD, PCV is common among Asians and makes up half of all AMD cases here, said Prof Wong. SNEC sees around 150 cases of PCV each year.
Sufferers experience blurred, distorted vision or a dark spot in their centre of vision.
Ms Yeo discovered her condition after experiencing blurred vision in her right eye which could not be rectified despite several trips to the optician.
“The vision blurring was getting from bad to worse. As I needed to drive a lot for my job, I became quite concerned that I could be a danger to myself and other motorists,” said Ms Yeo, whose condition appears to have stabilised after the treatment.
A GROWING BURDEN
Singapore’s eye disease burden is set to grow. All chronic eye conditions including AMD, glaucoma and cataract are estimated to increase significantly by 2040 due to an ageing population, according to a study published in January by the journal Annals by the Academy of Medicine, Singapore.
The study looked at the burden of eye diseases by age and ethnicity, and AMD is one of the eye conditions projected to see the greatest increase among Indians, by about 100 per cent, between 2015 and 2040.
Visual impairment from AMD can interfere with patients’ ability to recognise faces, as well as carry out everyday tasks like reading and driving. Left untreated, it can eventually cause blindness, said Dr Wong Chee Wai, consultant at the Cataract and Comprehensive Ophthalmology Department at SNEC.
In the elderly, poor vision is linked to other health issues. For instance, a 2007 study published in JAMA Ophthalmology found that elderly AMD sufferers were twice as likely to suffer from falls and four times more likely to require assistance with daily activities compared to those without AMD. They also reported 42 per cent more symptoms of depression.
The cause of AMD is presently unknown. However, the risk of developing it gets higher with age. About 8 per cent of Singapore adults aged 60 to 69 have AMD, and this risk rises to 16.3 per cent for those aged 70 to 79, said Prof Wong. PCV sub-types make up half of these cases.
According to Dr Wong, PCV is more common among men than women. Other known risk factors include obesity, diabetes and cigarette smoking.
“There also seems to be a genetic factor as it is more common among Asians and people of African descent than Caucasians although what the genetic factors might be, have not yet been identified,” he said.
INCURABLE, BUT TREATMENT CAN PRESERVE VISION
While there is currently no cure for AMD, early detection and proactive treatments can help preserve vision, experts say.
AMD and PCV patients have to remain on medications for life, but if treated early, regression without severe vision loss is possible, said Dr Wong.
“The amount of vision regained depends on how much vision was lost. But on average, patients can regain one to two lines of vision (on the vision chart).”
A key component of AMD and PCV treatment is the use of anti-vascular endothelial growth factor (VEGF) drugs, which are injected into the fluid within the eye and reduce the formation of abnormal blood vessels that damage the retina (the light-sensitive tissue lining the back of the eye), said Prof Wong.
VEGF drugs are usually used as a follow-up after patients undergo a type of treatment known as photodynamic therapy (PDT), said Dr Wong. PDT involves the use of a photosensitive intravenous drug (injected into a vein in the arm) and a low-power infra-red laser.
PDT causes damage to cells to kickstart the body’s own repair system to replace damaged cells with healthy ones, said Prof Wong. But it is not suitable for long-term therapy as studies suggest the treatment itself can result in permanent visual impairment after three or more sessions. PDT should be used judiciously, and usually in combination with anti-VEGF injection therapy, he added.
A new study offers hope for PCV patients like Ms Yeo, who now have the option of using a single anti-VEGF drug called aflibercept as a viable first-line treatment. Aflibercept has been available in Singapore since 2013, said Dr Wong.
The randomised two-year study, in which Ms Yeo participated, involved 333 patients aged 50 and above from 62 study sites, mainly in Asia Pacific, including Singapore, Japan, South Korea, Taiwan and Australia.
Findings have shown that early detection and regular treatment with (aflibercept) can preserve vision and inactivate polyps (seen in PCV), said Prof Wong, the principal investigator of the study.
The study also found that for up to half of the patients, the interval between the injections could be extended from one or two months in the first year, to four months in the second year – and possibly even longer as time goes on, said Dr Wong.
Although there is no guarantee that her vision will not deteriorate in the future, Ms Yeo considers herself “fortunate” to have caught her AMD before it caused further damage. She is due for a follow-up checkup next month.
“I feel relieved because my eyesight has stabilised and it is not getting worse. Many of us maintain our skin and hair, but we often take our eyes for granted. After this incident, I treasure my vision even more,” said Ms Yeo.
The only way to protect vision is through regular eye examinations as many eye diseases have no early symptoms, said Dr Wong. He advised adults above 60 to have an eye screening once a year, which can be done at a community eye screening event or with their optometrists.
“Between eye examinations, if you notice a change in your vision, see a doctor immediately. People who have been identified to have an eye problem should see an eye specialist, and the frequency of visits will depend on the severity of their eye condition,” said Dr Wong.
CLARIFICATION: In the previous version of the story, we quoted Professor Wong Tien Yin saying photodynamic therapy is not suitable for long-term therapy as the treatment itself can result in permanent visual impairment after three or more sessions. Prof Wong has clarified that studies suggest it to be so.












