Heart failure killed his father and baby sister, but this teen is fighting for a chance at life
At 14, Jovan Ho became the youngest person in Singapore to have a heart pump implanted, after he was found to suffer from a genetic heart disease.

(From left) Jovelynn Ho and her father Jason Ho, Javier Ho and his mother Cindy Lim, and Jovan Ho pose for a family photo. (Photo: Cindy Lim)
SINGAPORE: Some of Jovan Ho’s fondest memories with his father are of staying back after his school football practice for a kickabout of their own. The Chelsea fan has played football since he was five.
But after a genetic heart condition developed into advanced heart failure last year, the teenager had to hang up his football boots.
At the age of 14, Jovan became the youngest person in Singapore to have a type of heart pump called a HeartMate 3 left ventricular assist device (LVAD) implanted in June last year.
Now 15, he is back to most of the usual pursuits of adolescence – schoolwork, fast friendships and video games.
The heart pump is giving Jovan another shot at life. At the National Heart Centre Singapore (NHCS), patients with advanced heart failure see their one-year survival rate rise from less than 50 per cent to about 86 per cent after getting the pump fitted.
The 5cm-wide metal contraption has improved Jovan's quality of life, but it is only a bridge to what he truly needs – a heart transplant.
IN THE FAMILY
Jovan suffers from cardiomyopathy, a disease where he has a weakened heart muscle that affects the organ’s ability to pump blood around the body and can cause heart failure.
There is a growing trend of heart failure in Singapore according to Associate Professor David Sim, director of the Heart Failure Programme at NHCS.
The NHCS is the only place in Singapore where heart transplants are performed, and the only public hospital where patients can get an LVAD implanted.
The centre treated 3,157 patients for heart failure in 2022, an increase from the previous two years when numbers stayed under the 3,000 mark.
Assoc Prof Sim said the rising numbers are due to Singapore’s ageing population and ironically, better medical outcomes. People who suffer heart attacks can now live longer lives, during which they have a chance of developing heart failure because of previous damage to the organ.
Chemotherapy also contributes to heart failure because some of the agents used to treat cancer are toxic to the heart, he explained.
Listen: Dealing with worsening heart failure
In Jovan’s case, his condition is genetic, afflicting both his paternal grandmother and father.
Years before Jovan became the youngest person to receive the heart pump, his father Jason Ho was the youngest person in Singapore to have a heart transplant, at the age of 19 in 2006.
After that life-changing procedure, Mr Ho went on to marry his wife Cindy Lim and father three children with her – Jovan, Javier and Jovelynn. He lived 15 more years after the transplant, before dying in 2021 at the age of 34.
Ms Lim said that while her husband’s death was sudden – he collapsed at home without any warning signs – his general life expectancy was always known.
What the family was utterly unprepared for was the death of their two-year-old daughter, Jovelynn, from the same disease in 2018.
CODE BLUE
When Jovelynn started feeling lethargic one day in 2017, her parents thought it was the stomach flu. They gave her medicine and let her stay at home.
After she felt better, they sent her back to infant care. That morning, the teacher called her parents to inform them that their daughter did not wake up from her nap to drink milk.
Later that afternoon, the teacher called again. This time, Jovelynn was not well and seemed to be turning blue.
Ms Lim immediately took her daughter to the hospital. The girl appeared fine when her mother picked her up from infant care and was also fine when examined by a triage nurse at the hospital.
But when they were about to leave, Jovelynn turned blue again. Ms Lim ran back to the triage nurse. Her daughter received immediate medical attention and was admitted.
“In less than one hour, all of a sudden, they announced her bed, her room and mentioned a code blue,” said Ms Lim. Code blue refers to a situation where a patient is in cardiac or respiratory arrest.
In just a few hours, the once happy and healthy baby girl was a patient in the intensive care unit (ICU).
The next day, the parents received more bad news – Jovelynn’s heart function had dwindled to 20 per cent. The only treatment option was to put her on medication.
“The first thing (that) came to me was like, 20 per cent? How long can it last? It’s not like a battery that we can recharge or anything,” said Ms Lim, tearing up.
After a week in the ICU, Jovelynn’s condition improved and doctors moved her to a step-down unit. She stayed there for another week before being discharged.
But this was not the end of the family’s ordeal. In the ensuing months, the hospital’s cardiac unit followed up closely with Jovelynn, who was intermittently warded whenever she suffered symptoms.
Eight months after suffering her first bout of illness during infant care, she died.

JOVAN’S DECISION
When Jovelynn fell ill, doctors advised her parents to get their two older sons scanned for heart disease as well. Genetic testing in 2017 showed that Jovan suffers from the same condition, while Javier is healthy.
As Jovan’s heart disease was caught at an earlier stage, he was given medication, and was able to continue staying active by playing football.
But at the end of March last year, his condition took a sudden turn for the worse when he became pale, developed a cough and broke out in a cold sweat, Ms Lim recalled.
He was admitted to a hospital, but when his condition continued to worsen, doctors referred him to the NHCS. He was transferred to the centre on Jun 17, 2022.
With no time to lose, Assoc Prof Sim and his team, including clinical coordinator Sharon Neo and medical social worker Lim Jing Kai, rallied together to present Jovan and his family with a course of action.
If a heart pump was to be implanted, it would have to be done in a matter of days, said Ms Neo. The team took a few hours one evening to explain to Jovan how the device would work and the lifestyle changes it would entail.
When the LVAD is implanted, blood bypasses the weakened heart muscle and is diverted into the pump, which delivers the blood to the aorta.
The only part of the pump that remains outside the body is the driveline, which extends out from the abdomen and transfers power and data between the pump and an external controller.
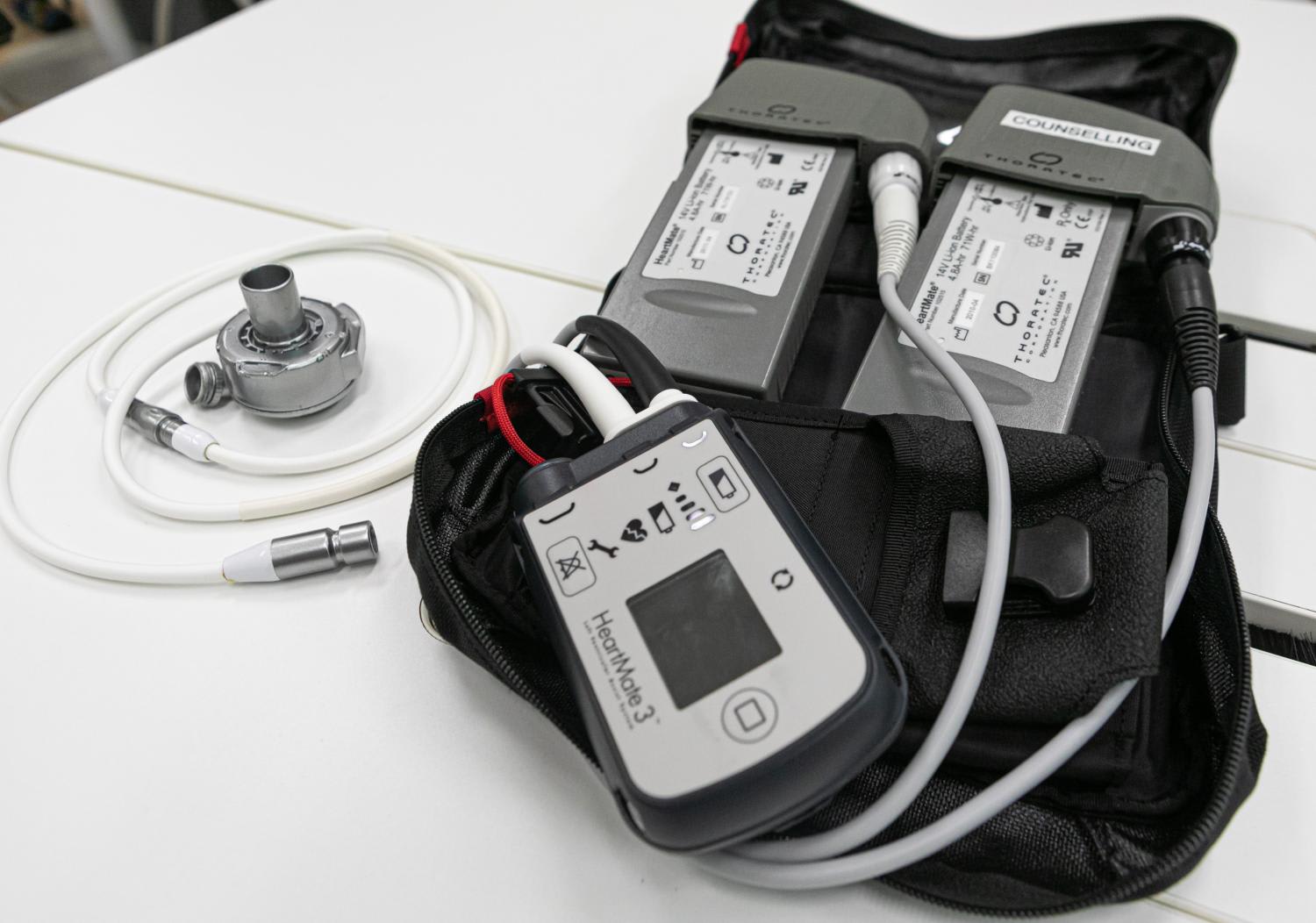
While patients with the pump can lead active lives and go back to school or work, they should avoid water sports and contact sports in case of infection or disturbance of the driveline. To prevent blood from clotting around the pump, they must also regularly take blood thinners.
All of this means that aside from being medically suitable, patients must meet psycho-social requirements to be considered for the pump, said Assoc Prof Sim.
They must be able to keep their medical appointments, take medication regularly and avoid activities that are not recommended. They must also have social support, as living with the pump requires the help of a caregiver.
It typically takes about a week for a caregiver to master the main task of changing the dressing around the driveline, which must be done every day, said Assoc Prof Sim.
The choice was clear for Jovan, who immediately decided to get the heart pump. Despite his young age, he has proven to be a very mature patient, said his clinical coordinator Ms Neo.
His choice was enabled by financial assistance. The LVAD costs S$167,000 before subsidies but most patients do not have to pay the full amount after means testing, said Assoc Prof Sim.
Aside from government financial aid, Jovan received assistance from NHCS’ Heart to Heart Fund. This helped to ease the burden on his mother, who works as a patient services associate.
Since NHCS’ Heart Failure Programme started in May 2009, it has treated 132 patients and implanted 153 pumps, including pump changes. The average age of a patient is 51 years.
“As long as you’re Singaporean, nobody will be denied the appropriate treatment due to financial concerns,” said Assoc Prof Sim.

HOPE FOR A TRANSPLANT
For Jovan and other heart patients below the age of 65, the pump is implanted as a “bridge to transplant”, a hopefully temporary measure before the desired organ transplant.
Under the Human Organ Transplant Act, enacted in 1987, all Singaporeans and permanent residents aged 21 and above are deemed donors unless they opt out. Their heart, kidneys, liver and corneas can be harvested for transplantation when they are declared brain dead.
In Singapore, the typical waiting time for a heart transplant is just under two years. As a matter of luck, waiting times can vary wildly – one patient spent just a day on the list before getting a transplant, while another waited as long as eight years, recalled Assoc Prof Sim.
Over the last decade, an average of five heart transplants a year were performed in Singapore.
The prognosis for those on the waiting list is generally dim. “If they’re still alive at the end of two years, we would not have called it advanced heart failure in the first place,” said Assoc Prof Sim.
But the situation is still better than before technological advancements like the heart pump came along, when heart failure was a “death sentence”, he said.
After recovering from the surgery, Jovan resumed lessons at Westwood Secondary School in September last year.
Since then, Ms Lim has noticed changes in her son. “Nowadays (he) knows how to make friends, to go out and play already,” she said.
For now, Jovan continues to await a heart transplant. Though disappointed that he had to stop playing football, he has found new ways to spend his free time at home.
The teen has started cooking for his younger brother Javier, now eight, and the rest of his family whenever he has time, his mother said proudly.