Inside Singapore's first specialised children's burn centre
Each year, KK Women's and Children's Hospital sees up to 400 new cases of children with burn injuries.
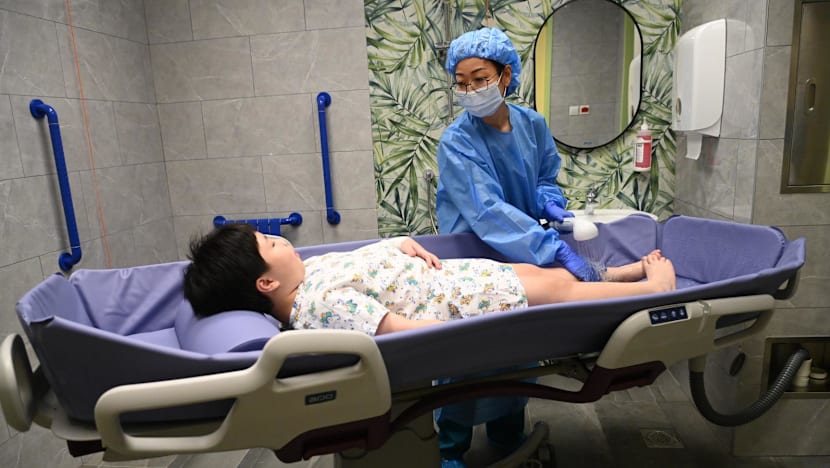
A specialised shower bed is used to clean and dry a patient with burns. (Photo: KK Women’s and Children’s Hospital)

This audio is generated by an AI tool.
SINGAPORE: More than a decade ago, a girl no older than 10 was rushed to the children’s emergency department at KK Women’s and Children’s Hospital (KKH).
Earlier in the day, her clothes had caught fire and by the time help reached her, the fabric had melted onto her skin.
Her tiny frame was scorched, across the shoulder and chest, with burns so severe that they had burnt through all layers of her skin.
Burns as large and deep as those the girl endured are classified as a major burn, with multiple surgeries required.
Layers of skin in the affected areas had to be reconstructed, and she spent weeks in the intensive care unit, followed by many more in hospital.
Even after practising as a plastic surgeon for decades, it was a memory KKH's Dr Kong Tze Yean carried like a scar.
While burns of such severity are uncommon, burn injuries among children remain a steady concern and many can be prevented, said Dr Kong, senior consultant at the department of plastic, reconstructive and aesthetic surgery.
Burn injuries often have a long and complex care journey, requiring close coordination across multiple medical specialties – from emergency treatment through rehabilitation.

In October 2025, KKH opened its first specialised burn centre for children, located next to the hospital’s children's intensive care unit.
The centre is staffed by a multidisciplinary team of plastic surgeons, nurses and allied health professionals, offering a full range of care from acute treatment to rehabilitation.
It also has features that speed up recovery and improve patient comfort, such as consultation rooms connected to treatment rooms, specialised shower beds and a dedicated procedure room.
Each year, the hospital sees up to 400 new cases of children with burn injuries, a number that has remained consistent over the past five years.
Infants and toddlers aged two and below are the most vulnerable group, accounting for half of all burn cases. Children aged five to 10 form another high-risk group, making up about 17 per cent of cases.
In 2024, scalds from hot liquids made up the majority of preventable burn injuries in children at 71 per cent, followed by contact burns at 19 per cent and friction burns at 5 per cent.

ASSESSMENT
When a child is taken to the children’s emergency department at KKH with a burn injury, the triage nurse first checks three critical aspects to ensure the child is stable: the airway, breathing and circulation.
Burns, especially around the face or neck, can cause swelling in the upper airway, which may narrow or block the child’s breathing.
“While a change in the child’s voice can be an early warning sign that the airway is narrowing or becoming blocked, drowsiness is often a late sign that the airway is already affected,” said assistant nurse clinician at KKH children’s hospital emergency department, Hafizah Kamil.
To assess breathing, the nurse looks for signs of respiratory distress, such as rapid breathing, unusual breathing sounds, or abnormal body positioning that a child may adopt to help them catch their breath.
Severe burns can also cause significant fluid loss, which may weaken circulation and lead to shock. The nurse will closely monitor the child’s heart rate, blood pressure and skin colour.
The nurse also checks how quickly colour returns to the skin by pressing on the skin or nails, to ensure that the child’s vital organs are receiving enough blood and oxygen.
Once the child's airway and blood circulation have been assessed to be stable, nurses will look at the burn location, size and depth.
"They look for burns wrapped entirely around a body part, such as a limb or the chest, that may affect circulation or chest movement, and monitor the child’s vital signs closely," said Ms Kamil.
Nurses will ask parents or caregivers questions to better understand the circumstances of the injury and guide treatment.
These include the cause of the burn, how the wound was sustained, whether the burn was cooled with running water, and whether any substances were applied to the wound.
Easing the child’s pain is a key priority.
"When a child suffers a burn, the excruciating pain can be overwhelming and terrifying. These sensations can make it difficult for a child to cooperate for subsequent procedures that address the injury," Ms Kamil said.
The child's pain will be assessed using an age-appropriate pain scale and nurses will review regularly to see if the pain level changes.
If the pain score is high, the team will act quickly and prioritise the patient for further assessment and treatment. Following the assessment, the patient will be provided with pain relief and the dose will be adjusted according to the severity.
Children with mild pain from the burns will be given paracetamol and ibuprofen, while intramuscular or intravenous morphine is used if they are experiencing moderate to severe pain.
If the wound was not run under water at home, or done incorrectly, the nurse will wash the burn area with sterile water for about 20 minutes.
"This helps to remove the remaining heat, preventing the burn from continuing to damage the skin, and reducing pain caused by the burn," said Ms Kamil.
As daunting and frightening as it may be for parents to see their child in pain, nurses encourage them to stay close and offer comfort.
"Whether it is holding the patients’ hands or simply being nearby, having a familiar face often helps a child feel more at ease in an unfamiliar environment."
Listen:
INSIDE THE BURN CENTRE
Once the young burn patients have been triaged at the hospital's children's emergency department, they are taken to the burn centre, where their injuries will be more closely examined.
The first round of dressing can be done at the centre, sparing the patient from having to return to the hospital over the next two days for wound reviews and dressing changes.
"Depending on the severity of the child’s burn injuries, each visit can look different for every patient," said Ms Joanne Jovina Cheng, an advanced practice nurse and assistant director of the division of nursing at KKH.
Unlike a general ward in the hospital, the burn centre offers specialised and integrated features that speed up recovery and improve patient comfort for the young burn patients.
Several key features are aimed at making the experience safer and less distressing for children and their families.
One of these is a specialised shower bed that allows wounds to be cleaned and dried under anaesthesia in a single location.
Ms Cheng said that this eliminates the need to move young burn patients between rooms, minimising infection risks.
"In the past, children had to remain awake during this process with some degree of pain."

The facility also includes consultation rooms that are directly connected to treatment rooms, ensuring seamless care from assessment to treatment.
This layout improves infection control and enables a faster response during emergencies.
The burn centre is next to the Children’s Intensive Care Unit, allowing for rapid access to critical care when needed.
In addition, there is a procedure room designed specifically for burn cases, which can be adapted for non-burn mass casualty incidents.
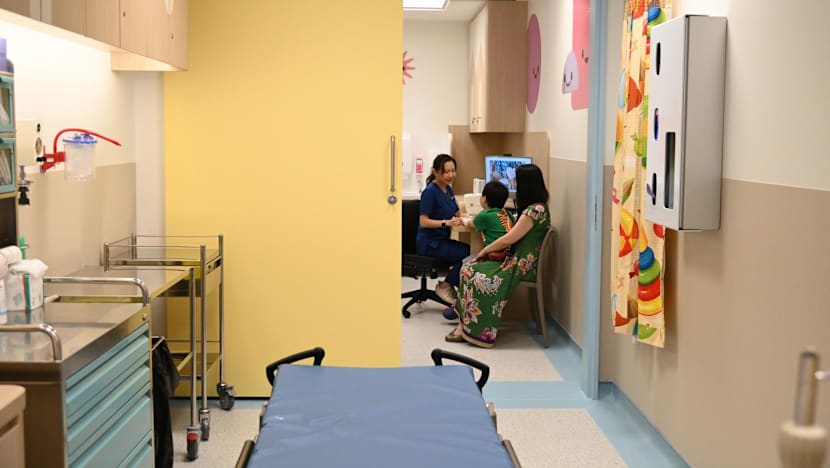
But care does not end when the child leaves. Young burn patients would often have to return to the burn centre for follow-up visits to have their wounds reviewed and dressings changed.
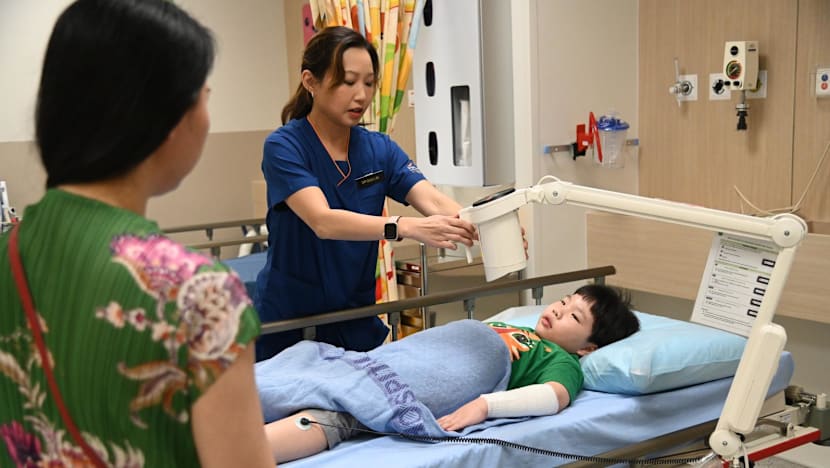
At the burn centre, wound care includes procedures such as changing dressings, wound cleaning and wireless microcurrent stimulation therapy to quicken burn healing.
"The road to recovery after a burn injury can be daunting for any child. Whether they are staying in the hospital or visiting for outpatient treatment, their greatest fear is often the same - the intense, sometimes excruciating pain associated with wound care for their burn injuries," Ms Cheng said.
"These young patients often experience pain more intensely due to underdeveloped coping skills."
Nurses use various distraction methods, from cartoons to music, to help calm and comfort the child.
"We also prioritise clear communication, providing parents with updates on how the wound is healing and walk them through simple steps for burn care at home," Ms Cheng said.
BURN INJURIES
While scalding is the most common type of burn injury, Dr Kong said most of such incidents treated at KKH are minor, with burns often smaller than the size of a person’s palm.
Doctors use the size of a patient’s palm as a guide, with each palm representing about 1 per cent of the body’s surface area.
Dr Kong described minor burns as “shallow” and “not so shallow”, intentionally avoiding common phrases such as first or second-degree burns, as they can frequently be misinterpreted.
Shallow scald burns often cause temporary redness that clears within 24 to 48 hours, allowing the skin to heal back to normal. Less shallow ones are known as superficial burns.
“That means only the top layer of the skin has been burnt,” Dr Kong said. “These are the ones where you might see blisters, or you might have the top layer of the skin coming off, revealing a kind of pink, slightly wet surface underneath.”
These are the most common types of burns that KKH’s paediatric burn centre sees. They do not require surgery and would usually heal on their own in about two weeks.
With advanced technology, such as a wireless microcurrent simulation therapy, healing of shallow burns is sped up from eight-and-a-half days to about five-and-a-half days.
“What it does is it delivers a very low electrical current - you can't feel it - that encourages the wound surface to heal faster,” Dr Kong said.
Major burns, which are those that affect more than 15 per cent of the body, or roughly 15 palm sizes, typically require admission to the intensive care unit or high-dependency unit.
Apart from surface area and depth of burns, Dr Kong said some “special areas” that are burnt would make the burn severe, such as what he called an “inhalation of injury”.
This happens from inhaling hot fumes or smoke in a closed environment.
“That’s where the internal surface of the respiratory tract, your throat and into your lungs, that inner surface, has been burnt.”
Taking precautions
While education about avoiding burns is important, both Dr Kong and Ms Cheng agree that greater attentiveness to one’s surroundings can help reduce risks.
“With scalds, it is often a typical story where a toddler who can now walk goes and pulls things from the top of the stove and spills hot drinks on themselves,” said Dr Kong.
“Parents, you really want to avoid having hot drinks or hot liquids anywhere near your children,” he said.
Even when a table is higher than a child’s reach, parents should not make the mistake of thinking children would not tug at tablecloths.
“You may want to choose kitchen appliances with child safety locks, and keep them out of the kitchen, perhaps using safety gates or even keep them in play pens.”
Dr Kong has treated children who suffered from electrical burns after sticking their hands in electrical sockets.
“Supervision is very important. You always want to have at least one parent, one caregiver to be supervising toddlers at all times.”
While most burns are preventable, cases still occur despite precautions.
One of the first and most important steps parents should take if their child gets burnt would be to remove the item that is burning the child, Dr Kong said.
“If this is (a piece of) clothing, you’d want to take off that clothing with the hot liquid and immerse or run the burn under cool tap water for at least 10 to 20 minutes.”
Dr Kong explained that this method is most effective within the first hour and can significantly reduce the severity of the burn.
It is also important that parents avoid applying household remedies or "grandma remedies” such as toothpaste or other oils and creams to the burn.
Burns that need to be covered should be done so with materials that would not stick to the skin, such as cling wrap.
“In fact, we do use that in the emergency department as a temporary measure while assessing these burns in order to stop the moisture loss as much as possible from the burn,” Dr Kong said.
Parents are also advised to monitor their child’s pain levels. Painful burns often indicate that the skin is still alive and the nerves remain intact, while deeper burns may be less painful.
On caring for the wounds, Ms Cheng advised that moisturising is important to ensure that the scars heal properly.
After patients get discharged, they come back for annual check-ups so the team can assess if the scar is healing properly.
“However, there are cases where the scar is not well managed, because it's so severe that they have very bad scars. So we would work with them, both medically or surgically.”
One common question Ms Cheng often gets from parents is whether water can touch the scar despite it still looking “raw”.
“We reassure them very confidently that it’s okay to do that and it helps the recovery.
“It encourages them to get back into normalcy and get back to their life and forget all about the things that happened,” she said.
WORKING WITH THE FAMILY
Recovery after a burn is different for every patient. Physical wounds may heal with time, but emotional ones can linger.
Beyond treating physical injuries, nurses at the hospital’s paediatric burn centre also assess how a child is coping emotionally and may recommend support such as music therapy or art therapy.
“If these don’t work, we usually push them to see a psychologist so they can cope with the challenges that are happening,” said Ms Cheng.
“Most of the time, the children and parents benefit from this. But of course, there are times when medication is needed.”

"Often times, parents are overwhelmed by guilt, fear and helplessness when they arrive with their children who have burn injuries," said Ms Cheng.
"They may feel responsible for the injury, terrified of the pain their child is enduring, or simply lost in a complex hospital environment."
One of the most critical aspects is teaching parents to be a “team player” who can best help comfort and encourage the young patient through procedures.
"We also acknowledge their feelings and reassure them that they are not alone in this process," she added.
"Additionally, involving them in assessment and treatment wherever possible promotes partnership in caring for their child."














