Why wiping out smallpox has stoked risk of monkeypox
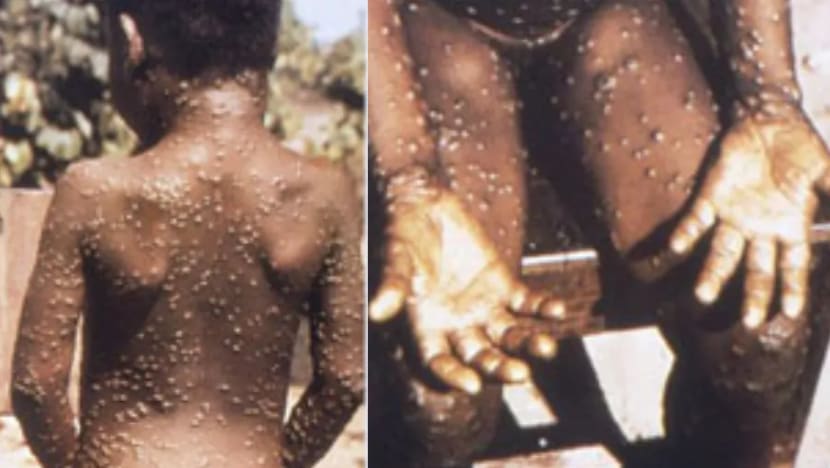
A child infected with monkeypox. (Photo: Wikimedia Commons/United States Centers for Disease Control and Prevention)
The global eradication of smallpox more than 40 years ago was one of the greatest achievements in public-health history, vanquishing a cause of death, blindness and disfigurement that had plagued humanity for at least 3,000 years.
But, on the downside, it led to the end of a global vaccination programme that provided protection against other pox viruses. That includes monkeypox, which has been spilling over from its animal hosts to infect humans in Africa with increasing frequency since the 1970s.
More recently, monkeypox has sparked outbreaks in Europe and North America, demonstrating again how readily an infectious agent that emerges in one country can become an international concern.
What’s monkeypox?
“Monkeypox” is a misnomer resulting from the fact it was first discovered in 1958 when outbreaks of a pox-like disease occurred in monkeys kept for research.
While monkeys are susceptible to it, just like humans are, they aren’t the source. The virus belongs to the Orthopoxvirus genus, which includes the variola virus, the cause of smallpox; the vaccinia virus, which is used in the smallpox vaccine; and cowpox virus.
Monkeypox is less contagious than smallpox and the symptoms are milder. About 30 per cent of smallpox patients died, while the fatality rate for monkeypox in recent times is around 3 per cent to 6 per cent, according to the World Health Organization.
Related:
What does monkeypox do?
After an incubation period of usually one to two weeks, the disease starts with fever, muscle aches, fatigue and other flu-like symptoms. Unlike smallpox, monkeypox causes swelling of the lymph nodes.
Within a few days of fever onset, patients develop a rash, often beginning on the face then spreading to other parts of the body. The lesions grow into fluid-containing pustules that form a scab. If a lesion forms on the eye it can cause blindness.
The illness typically lasts two to four weeks, according to the WHO. The person is infectious from the onset of symptoms until the scabs fall off. Some patients have genital lesions and the rash may be hard to distinguish from syphilis, herpes simplex virus infection, shingles and other more common infections, according to the US Centers for Disease Control and Prevention.
Mortality is higher among children and young adults, and people whose immune system is compromised are especially at risk of severe disease.
Where does it come from?
The reservoir host or main carrier of monkeypox disease hasn’t yet been identified, although rodents are suspected to play a part in transmission.
It was first diagnosed in humans in 1970 in the Democratic Republic of the Congo in a 9-year-old boy. Since then most cases in humans have occurred in rain forest areas of Central and Western Africa.
In 2003, the first outbreak outside of Africa was in the US and was linked to animals imported from Ghana to Texas, which then infected pet prairie dogs. Dozens of cases were recorded in that outbreak.
How is it transmitted?
Monkeypox doesn’t spread easily between people. Contact with the virus from an animal, human or contaminated objects is the main pathway.
The virus enters the body through broken skin, the respiratory tract or the mucous membranes in the eyes, nose or mouth.
Human-to-human transmission is thought to occur mainly through large respiratory droplets, but can also following contact with body fluids or lesion material, or indirectly through contact with contaminated clothing or linens. It may also be transmitted during sex.
Common household disinfectants can kill the monkeypox virus.
Related:
How often does it occur?
Monkeypox is endemic in many parts of West and Central Africa. Outbreaks outside the continent occur infrequently - at least eight known exported cases since 2017 - usually involving international travelers. They don’t typically cause onward transmission.
In May 2022, however, more than two dozen cases were reported in the UK, Portugal, Spain, Italy, Sweden, Belgium, Canada and the US. Australia confirmed a case on May 20 in a man who had just flown back from the UK.
What’s unusual about this outbreak?
It’s led to multiple chains of transmission in clusters in multiple countries that don’t normally report monkeypox. The cases don’t involve recent travel.
Instead, community spread is suspected among individuals who self-identify as men who have sex with men - suggesting transmission through close sexual and personal contact.
The cases are thought to have been caused by a West African “clade,” or strain, which has a case-fatality rate of 1 per cent to 3.6 per cent. (That compares with 10 per cent for a second strain called Congo Basin, which appears on the US government’s bioterrorism agent list as having the potential to pose a severe threat.)
Is monkeypox a pandemic threat?
The emergence cases involving human-to-human transmission has raised concern that the virus may undergo genetic changes and become more adept at spreading from person to person.
Still, even the Democratic Republic of the Congo, where thousands of infections occur annually, that has yet to occur.
How is it treated and prevented?
The illness is usually mild and most patients will recover within a few weeks; treatment is mainly aimed at relieving symptoms. For the purposes of controlling a monkeypox outbreak, the CDC says smallpox vaccine, antivirals, and vaccinia immune globulin can be used.
Vaccination against smallpox can be used for both pre- and post-exposure and is as much as 85 per cent effective in preventing monkeypox, according to the UK Health Security Agency. It lists cidofovir and tecovirimat as antiviral drugs that can be used to control monkeypox outbreaks.
Tecovirimat was approved by the European Medical Association for monkeypox in 2022 based on data in animal and human studies, but isn’t yet widely available, according to the WHO.
Newer vaccines have been developed, of which one has been approved for prevention of monkeypox. The main way to prevent infection is by isolating patients suspected of having monkeypox in a negative pressure room, and ensuring health staff wear appropriate personal protective equipment.
Is there a test for monkeypox?
Yes, monkeypox is diagnosed based on the detection using real-time polymerase chain reaction (PCR) tests of viral DNA in specimens collected from the scabs or swabs of a patient’s lesions. In the US, these are available at state health departments and the CDC.












