When can you get a COVID-19 vaccine? Five things you should know
Researchers are accelerating what usually takes 10 to 15 years so that a vaccine could be ready by next year. But it is no easy task, so what do the experts have to say about the hopes for success?
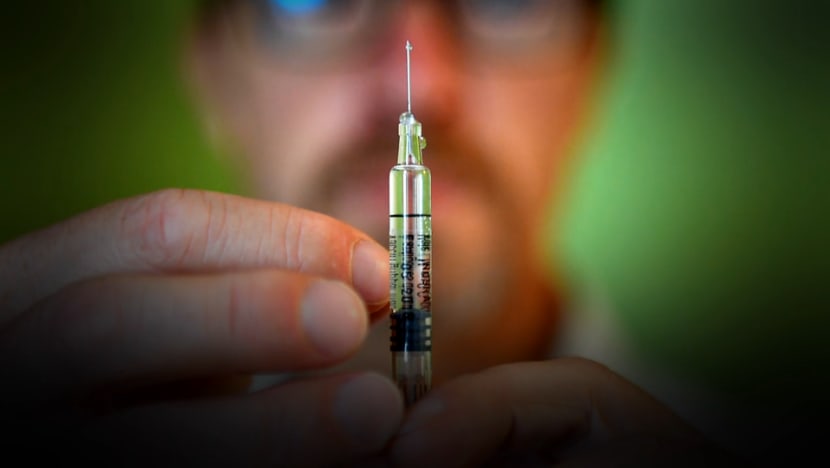
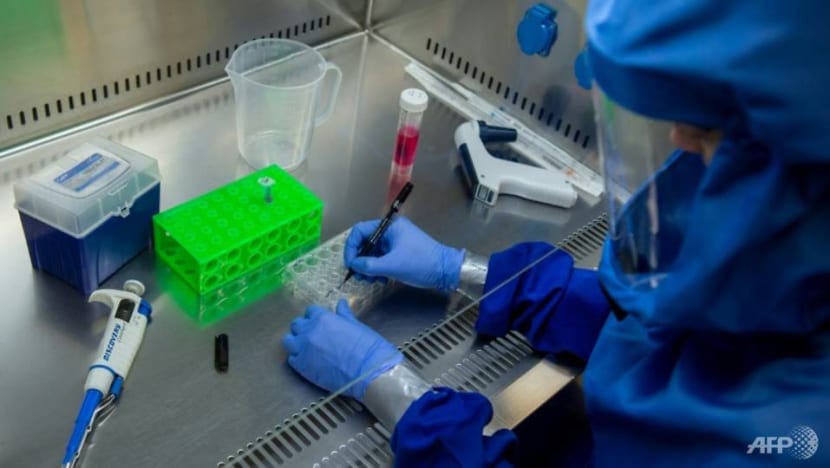
Many hope that a vaccine will be the magic bullet to fight COVID-19. What are the chances?

This audio is generated by an AI tool.
SINGAPORE: Massive efforts are underway to develop a vaccine strong enough to fight and eliminate the novel coronavirus.
Latest reports indicate that at least 165 vaccine candidates are being developed across the world, including in the United States, the United Kingdom, India, China and Singapore.
Nearly 30 projects are already in various phases of human trials, including one jointly developed by Duke-NUS Medical School and US pharmaceutical company Arcturus Therapeutics.
But developing a vaccine is no easy task. What usually takes 10 to 15 years, researchers are now accelerating so that a vaccine could be ready for emergency use by next year.
With the process on the fast track, the hope of a vaccine comes with vital questions. And here are some answers from the experts.

1. IS A VACCINE BY 2021 REALLY POSSIBLE?
Six of the vaccine candidates are now in the third stage of testing, and they “look potentially interesting”, Dr Jerome Kim, the director general of the International Vaccine Institute, said on the programme In Conversation. (Watch the episode here.)
“They make the right protective responses. They all protect monkeys against infection. ... So there’s a lot of suggestive evidence that they might protect for at least a short period of time. We don’t really know, though,” he said.
“We have to be very careful when we use animal studies. ... So now it’s (about) making sure that we can show that it actually prevents infection in humans.”
He cited the potential of the vaccine candidate from the University of Oxford and drug giant AstraZeneca as an example. Recent results of a study, involving more than 1,000 human volunteers, showed that the vaccine generated a strong immune response.
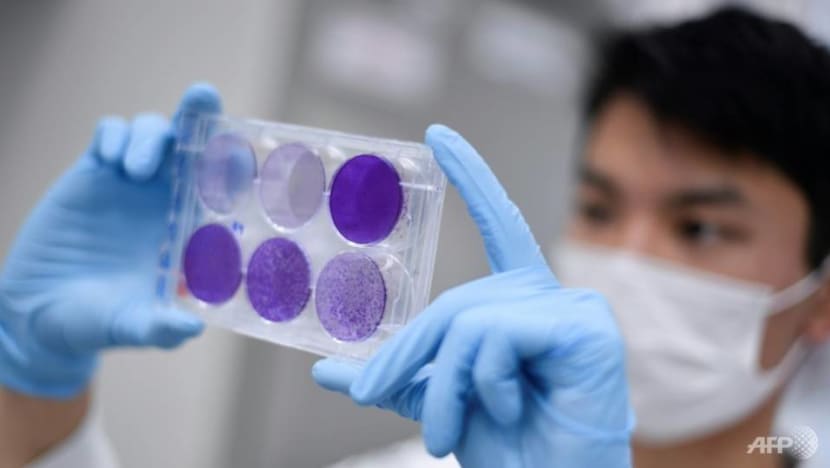
The reason this could be done at “remarkable” speed, said Professor Ooi Eng Eong, deputy director of Duke-NUS Medical School’s Emerging Infectious Diseases Programme, is that the research groups concerned have worked on other viruses before.
The Oxford group has done “a lot of work” on the Middle East Respiratory Syndrome, on Ebola and on Chikungunya, he noted on the programme Insight. (Watch the episode here.)
“So how they got this (vaccine) very rapidly into humans is they went to the regulator and said, ‘Look at our past record.’”
Mr Sudarshan Jain, the secretary general of the Indian Pharmaceutical Alliance, acknowledged that the virus behind COVID-19 is “very cunning” and “unpredictable”, which drug makers “don’t understand fully” yet.
But as the “entire pharmaceutical industry has taken up the challenge”, he said on In Conversation, “there’s a possibility” of four or five vaccines. “I’m hopeful that we should be able to reach that position towards next year.” (Watch the episode here.)
Dr Kim thinks it is possible: “If everything works as it should, by the end of the year, we may have a readout on at least one of the vaccines currently in the pipeline — that it may protect or may not protect populations.”
2. HOW SAFE WILL IT BE?
The bigger question, Dr Kim noted, is whether there will be “enough safety data”, as the final phase of human testing in the “normal development cycle” of a vaccine is five to 10 years, instead of six months.
WATCH: Is a safe COVID-19 vaccine by 2021 really possible? (6:04)
The “thousands” of safety evaluations to be done this year will be a “good amount”, although he acknowledged: “We aren’t really going to be able to tell.
“In the short term, to the point where the vaccine will either be given in emergency-use authorisation or an approval for market, we’d have less long-term safety information than we normally have.”
So vaccine developers should “follow the people who receive the vaccine and placebo for a much longer time than we normally do”, he said, suggesting “two or three years or longer”.
This is to ensure that there are no side effects “at a very low level that we should be aware of, but that we can’t because we’re pushing hard to show that the vaccine works”.
Prof Ooi stressed: “Between being the first (to develop a vaccine) and getting it right, it’s more important to get it right.”
But he does not see speed and safety as “mutually exclusive”, and thinks “we can shrink the timeline” for vaccine and drug development in general, which has been lengthened as more studies were added over the decades.

“The important thing is the body of evidence that guides the development,” he said.
“If the evidence is strong, ... then you can move very, very fast because you know what to look for ... and (have) the confidence that what we're doing is going to be safe.”
READ: 5 things you need to know about a COVID-19 vaccine
3. WILL COUNTRIES HAVE EQUAL ACCESS TO THE VACCINE?
Much is at stake in the COVID-19 vaccine race, although it has to do not only with science, but also politics.
The current US administration has already been accused of trying to monopolise first rights to vaccines being developed by a company in Germany and one in France — alleged attempts that the two European governments made sure to block.
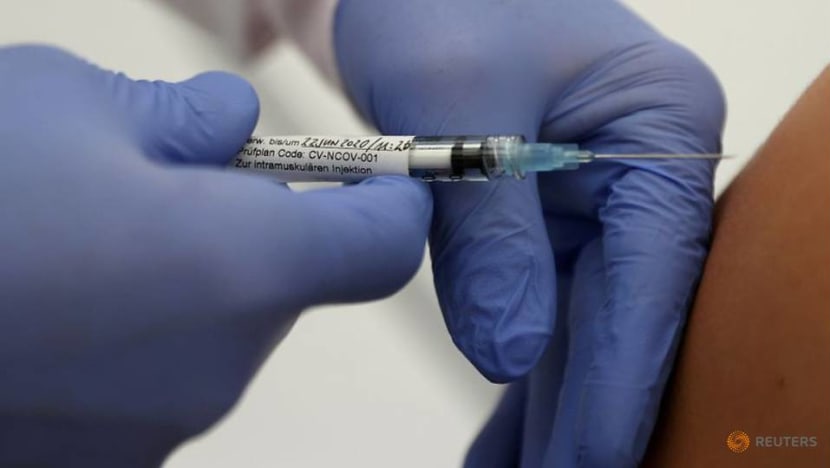
The reason for self-interest is evident, noted Prof Ooi. Countries that vaccinate first will “get out of all the lockdowns” and restrictions, return to normal economic activity and recover “much faster” than those without access to the vaccine.
There are “bound to be” politics involved, said Mr Jain. “Perhaps ... in the country where the vaccine development has taken place, the citizens of that country will demand that, first, the vaccine should be available in (their) country.”
But with the vaccine development taking place across the world, he reiterated his belief that a handful of vaccines will emerge, which will “ensure” supply. There is also “a lot of discussion” about avoiding vaccine hoarding, he cited.
“The dialogue will help us to ensure equitable distribution. It may not be 100 per cent perfect, but there’s a lot of consciousness,” he added. “At the end of the day, we’d like to find a level playing field.”
In May, Chinese President Xi Jinping committed to making a Chinese vaccine available to all.
But the question here, said Prof Joseph Liow, the dean of Nanyang Technological University’s College of Humanities, Arts and Social Sciences, is whether Beijing can win other countries’ trust and show that it is extending this help “in good faith” and with “no strings attached”.
WATCH: US-China rivalry politicises the COVID-19 vaccine race (4:59)
Even if governments map out a plan to “guarantee” vaccines for “a certain percentage of their need first”, said Dr Kim, “it may not be that much”.
“I mean, who are the people in greatest need? It may be the elderly, healthcare workers or people with underlying conditions that make them more vulnerable to severe disease or death.
“Maybe that’s 20 per cent of the population. So you don’t need all of the vaccine all at once. You may want to just vaccinate the most vulnerable people first.”
4. SO HOW SOON CAN EVERYONE GET VACCINATED?
As someone with no comorbidities, or underlying diseases, Mr Jain does not expect to be a candidate for immunisation before the end of next year. That means vaccination for everyone only by 2022.
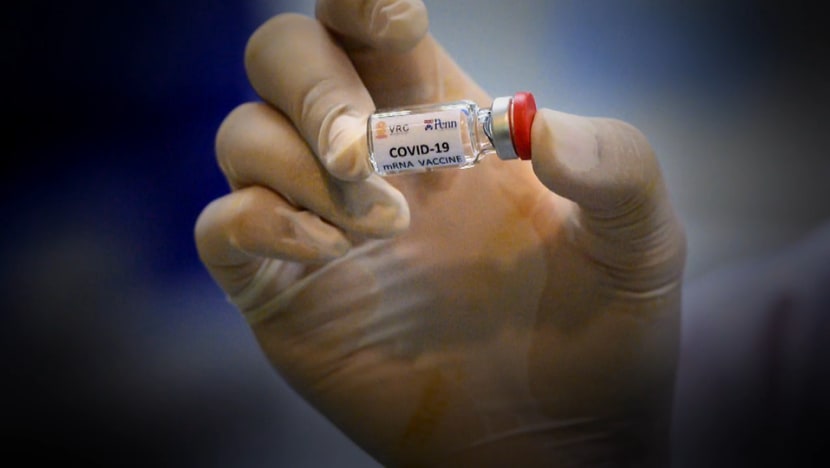
“Even if we do the best (to ramp up production), I don’t think we can see anything earlier,” he said. “The capacity at the moment is limited. ... It’ll take time for production and distribution (to be ramped up).”
Dr Kim noted that the US government is asking companies to start the manufacturing, seemingly “placing very educated bets on certain vaccines” and de-risking the projects by giving the companies funding — which he hopes will also “enable the companies to offer the vaccine at a lower cost”.
Organisations like the Coalition for Epidemic Preparedness Innovations are doing the same, including trying to secure manufacturing facilities down to the glass vials for the vaccines. The coalition has identified the need to have vaccine capacity for 10 billion doses.
“There is a manufacturing capacity out there. And the real question will be how quickly can we mobilise it,” said Dr Kim.
“Countries and companies are already making contracts with different organisations (and) manufacturers to be able to ensure that the vaccine is made, ... (but) we’ve never undertaken something like this before.”
If 60 to 70 per cent of people need to be vaccinated to achieve “herd immunity”, that may mean “vaccinating in the order of four billion to six billion people”.
“If there are two doses (per vaccination), that’s eight billion to 12 billion doses of vaccine. That’s a huge number,” he said, adding that getting up to those numbers over the next 12 months “would be a stretch”.
5. WILL A VACCINE MEAN A RETURN TO NORMAL?
All things considered, Mr Jain doubts that life will return to normal in the first year of discovering a vaccine.
“Hence it’s very important that all of us have to be cautious. All of us have to wear masks, ... behave with social distancing, and then the whole process will evolve over a period of time,” he said.
Most experts agree that a vaccine will not get rid of the coronavirus. “Too many people are now infected with Sars-CoV-2 that it won’t disappear,” said Prof Ooi.
Citing another reason the coronavirus is here to stay, he added: “It came from an animal, and we can’t vaccinate all the animals, especially the wild animals.
“So we’ll have this virus, and occasionally it’ll spill over and cause outbreaks, especially when vaccination rates are low. And that would be the challenge.”
People may have to also accept that the first vaccine put into use “might not even be able to prevent infection”, said Prof Jin Dong-Yan from the University of Hong Kong's School of Biomedical Sciences.
“But if it could prevent severe disease and ... not have a major adverse effect, that’s already good enough,” he told Insight.
Virology professor Ian Jones from the University of Reading in the UK noted that the data released so far indicates that the experimental vaccines protect against COVID-19 but may not give the “sterilising immunity” to stop an infection altogether.
“The problem with that would be that someone who’s vaccinated could still be infected and could then spread the virus, so it’s not the perfect solution,” he told Insight.
Even so, he views the development of a vaccine as “the most useful way forward”.
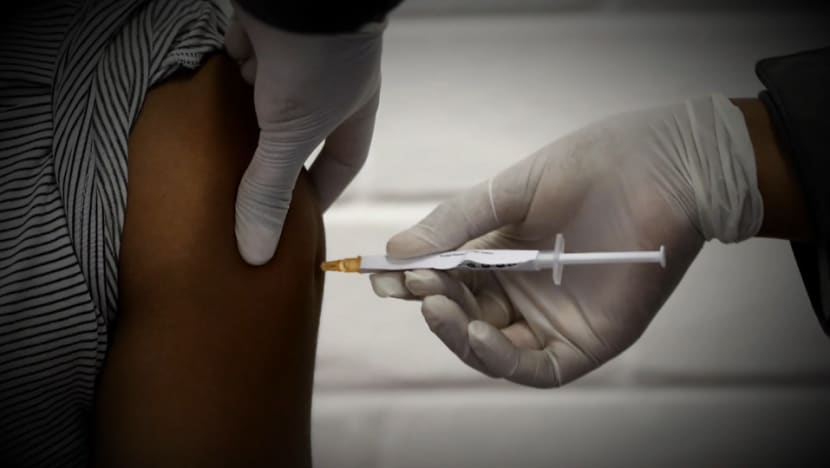
“What we're aiming for is a vaccine that takes away the fear of the disease,” he said. “If you get vaccinated, and you’re pretty confident that you're not going to die, then I don't think people will worry too much.”
And of all the solutions to the pandemic, a vaccine is “probably the most cost-effective”, believes Dr Kim. “A vaccine is the one potential intervention that’ll get us back to something similar to what we had before,” he said.
How similar will depend “a little bit on the qualities of the vaccine” and also on “several of the unknown things about the virus and viral infection in the population”.
“We’ve learned a tremendous amount in six and a half months, but it’s not enough,” he noted.
Assuming vaccination rates are at 60 to 70 per cent five years from now, however, then he would say “we’ve protected the population from the consequences of an outbreak”.
“You’ll see an occasional COVID-19 infection that’ll look like someone has a fever and maybe some cough or shortness of breath. You’ll test them, and you’ll find COVID. But it won’t spread in the population because enough people are immune.”
For now, the “bread and butter” is safe distancing, a high level of hygiene “and all that”, said Prof Ooi. “Then you overlay that (with) vaccines and drugs. Then we have a chance of really overcoming this virus.”
The programme Insight airs on Thursdays at 9pm, and In Conversation airs every Wednesday at 9pm.



















