Commentary: Anticipating COVID-19 vaccine side effects makes it likely you’ll experience one
Emphasising the side effects from the COVID-19 shot could not only increase the incidence of those responses in patients, but also contribute to vaccine hesitancy, says this professor.
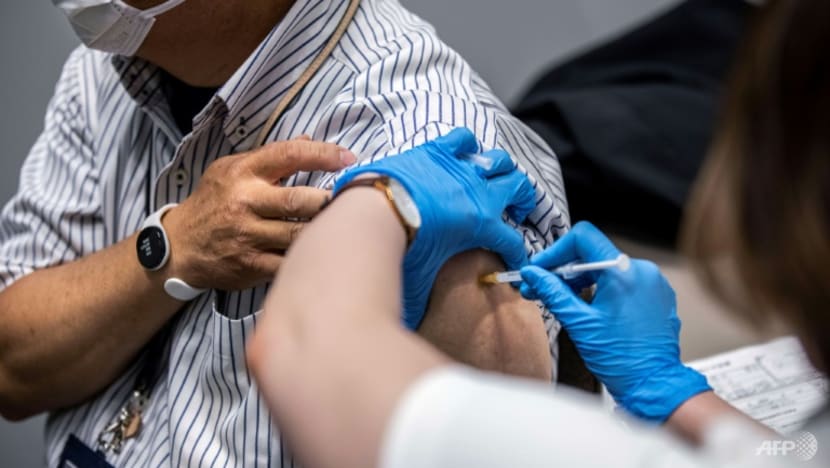
DUNEDIN, New Zealand: The COVID-19 pandemic has highlighted several interesting features of modern medical practice – most recently the “nocebo” response, which may account for a significant number of side effects people experience following vaccination.
Nocebo responses (from the Latin “noci”, which means to harm) are the opposite of the better-known placebo. While the latter describes improvements in symptoms following inert medication, the nocebo response heightens symptoms if a person anticipates them. It can increase pain if someone expects something will hurt.
A fascinating meta-analysis examined data from 12 clinical trials of COVID-19 vaccines, involving over 45,000 participants, and found that about two-thirds of common side effects people experience after vaccination could be due to a nocebo response, rather than the vaccine itself.
ADVERSE EFFECTS NOT CAUSED BY VACCINE
Nocebo responses can be troublesome and significant. They include headaches, fatigue, muscle pains, nausea or diarrhoea. Such symptoms may be related to anxiety or negative expectations, or day-to-day sensations being incorrectly attributed to treatment.
While previous analyses in other fields had already confirmed the presence of nocebo responses in randomised trials, COVID-19 vaccine research dramatically highlights its frequency.
The latest study found up to 35 per cent of patients in the placebo arm of vaccine trials had adverse events, such as headaches and fatigue. Mathematical analysis showed that 50 to 75 per cent of patient symptoms after the real vaccination (not placebo) may have been caused by those nocebo responses.
A different group of researchers from Italy reviewed other COVID-19 vaccine trials and confirmed these conclusions. These findings are potentially significant, as vaccine hesitancy and refusal have been linked to patient concerns about side effects or major adverse events.
Knowing how frequently self-limiting nocebo responses happen may reduce vaccine hesitancy.
NOCEBO RESPONSES CAN WORSEN PATIENTS' HEALTH
Together, the placebo and nocebo effects are better understood as two aspects of what medical practitioners call a “meaning response”. Both occur in relation to the importance and meaning patients place on their illness, their relationship with their healthcare providers, and their thoughts and beliefs about proposed treatments.
Nocebo responses are now being recognised as potentially important contributors to patient outcomes. For example, if a doctor or nurse gives pessimistic or negative information about pain, various studies have demonstrated that the patient’s pain can worsen, regardless of the degree of tissue damage.
Not feeling validated or respected by the doctor may also inhibit the efficacy of medications and increase side effects.
Previous research in New Zealand has also illustrated how negative media coverage may increase patients’ experiences of adverse events after compulsory changes to their medication regimes. For example, brand switches of thyroxine in 2007 and of an antidepressant in 2018 were followed by increased reporting of side effects and adverse events.
Acknowledging and publicising the potential contribution of nocebo responses may be useful for further generic substitutions.
FUELLING VACCINE HESITANCY FEARS
Vaccinators need to avoid inadvertently contributing to nocebo responses when advising their patients. They could use positive framing about the very low risk of serious adverse events. They could also briefly explain that nocebo responses are common and self-limiting.
However, my own experience as a patient receiving three COVID-19 vaccinations was disconcerting. No one in the various vaccinating teams said anything positive about the vaccine or its efficacy in preventing me or my family from catching the virus, or reducing the severity of the illness if we did.
And just after receiving the third injection, I was further disquieted by warnings about chest pain and reminders that I should seek immediate medical attention if I experienced any. This extra information on heart problems as a potential adverse event followed recent concerns about rare cases of myocarditis after vaccination.
All the vaccinating staff were conscientious and kind, but it seemed odd they hadn’t been instructed to discuss the benefits of vaccination. It might have been a useful approach to country-wide vaccine hesitancy.
While well-intended, it is possible that their emphasis on serious side effects from the vaccine may increase the incidence of nocebo responses in a population already primed for them. This could mean more patients will present to their doctors or emergency departments with symptoms unrelated to the vaccine itself.
TALKING ABOUT NOCEBO RESPONSES CAN REASSURE PATIENTS
Anecdotally, advice from vaccinators appears to be quite variable. It may be helpful if they incorporated an understanding of potential placebo and nocebo responses into their vaccination advice to each patient.
Health authorities and health professionals need to understand meaning responses and their role in clinical practice. Incorporating those insights into healthcare communication may prevent unnecessary patient anxiety, worrisome symptoms and considerable healthcare expenditure.
Respecting autonomy means patients need to be asked if they want to receive information about side effects or adverse events. The juggle is how to inform patients about the very low risk of serious harm while not increasing their apprehension.
Pandemic research is now also exploring potential parallels between long-COVID and other chronic conditions, such as Myalgic Encephalitis/Chronic Fatigue Syndrome, as well as tentative associations between adverse childhood experiences and vaccine hesitancy.
Without intending to minimise the pandemic’s devastating impact, it is providing us with useful insights into wider current medical and sociological issues.
Hamish Wilson is an Associate Professor in General Practice at the University of Otago. This commentary first appeared in The Conversation.


















