Commentary: Why do we keep going to the A&E when we don’t need it?
With the Omicron wave hitting Singapore, worried patients are flooding the Accident and Emergency Departments of local hospitals. Dr Devin Tan, an emergency medicine doctor gives an inside view.
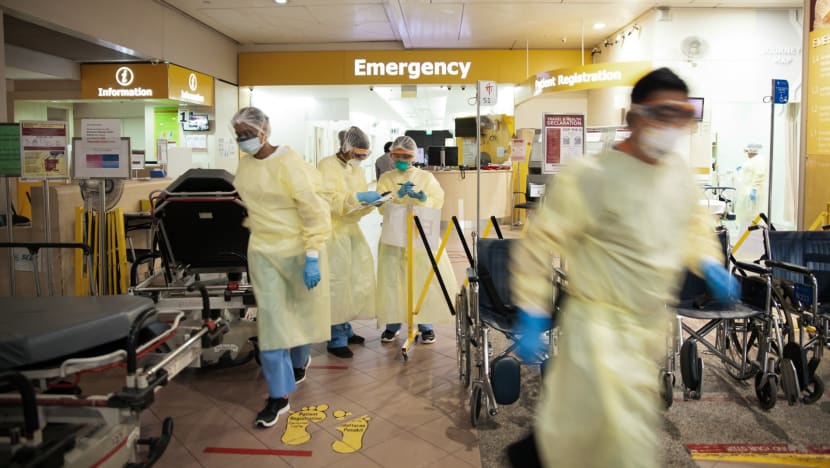
The accident and emergency (A&E) department at Tan Tock Seng Hospital in Singapore, in a photo posted on Sep 19, 2021. (Photo: Facebook/Tan Tock Seng Hospital)
SINGAPORE: These days, a regular day in the emergency department (ED) – or at least the Accident and Emergency (A&E) Department at Raffles Hospital looks like this:
Triaging the long queue of concerned patients and their caregivers, rushing to examine patients who just arrived at the ambulance bay, performing emergency procedures, and at the same time, caring for patients with non-emergency conditions.
Every second matters at the ED. With the Omicron variant, the “flooding” of patients has made triaging challenging. Triage helps the ED team decide which patient has the highest needs – for instance, someone who has had an acute stroke, a heart attack or severe trauma must be seen first.
With increased patients at the ED, triaging takes a longer time than usual. This can affect the speed at which patients with higher acuities receive medical care and disrupts the purpose of the ED – to provide timely emergency care to save lives.
“EXPERIENCED STAFF” AND PEACE OF MIND
Seeing the increasing numbers, the Ministry of Health put out an advice not to rush to see a general practitioner (GP) or visit the ED just to confirm COVID-19 test results or to get a medical certificate. But this still happens. One reason is there’s a group that still feels vulnerable.
Despite achieving a high COVID-19 vaccination rate in the Singapore population, young patients below the age of three and the elderly are generally patients classified under “Protocol 1”. This means that an antigen rapid test (ART) and polymerase chain reaction (PCR) test is recommended.
It is not surprising that parents with young children make up a certain proportion of patients that we see.
They worry about subjecting their children to the recommended PCR swab tests. When we talk to them, they tell us that they believe a hospital’s ED team is experienced and can provide their children with a more pleasant or “less painful” swab test experience.
There are also patients who face challenges with isolation with their children at home. This is especially when there are vulnerable elderly family members living in the same household.
For these patients, they would often visit the ED and may request to be transferred to a community care facility or COVID-19 treatment facility.
What about other adults who do not fall into this vulnerable category? Well, there are different motivations behind each visit.

Firstly, there is the uncertainty of post-COVID-19 conditions.
Due to a COVID-19 infection, some patients came to the ED with persistent symptoms of chest tightness, shortness of breath or lethargy. In general, their concerns are genuine as studies have shown that COVID-19 infections can lead to systemic complications.
There are also patients who would come to the ED hoping to register their COVID-19 infection in the national registry.
As we all know, one’s medical history – especially if there was a COVID-19 infection – can lead to certain implications when travelling such as the change for an additional booster injection which can affect vaccination status.
Similar to infected parents with young children, some patients are also worried about transmitting the virus to their loved ones at home and prefer to be isolated in a COVID-19 treatment facility.
There are also those who are genuinely afraid of the Infectious Diseases Act and do not want to face any offences with regards to exposing others to the disease. Although the Government has made changes to some of these rules, to them, the responsible thing to do is to seek emergency care at the ED.
DIFFERENTIATING THE WELL FROM THE UNWELL
Frontliners do understand the fears and concerns patients have when they test positive. But we also need to urge them to remain calm and assess their own symptoms objectively.
At the ED, we get patients who suffer from more severe symptoms of COVID-19 and require emergency care to cope with the illness. However, there are also cases where patients would present with a mild fever that subsides after taking paracetamol.
As has been the case even before the COVID-19 pandemic, we prescribe paracetamol to patients with fever, and if they feel better after an hour or so, they are discharged from the ED.
If the patient does not feel better, we might escalate our investigations and switch the treatment plan, or even get them admitted for observation.
For the first group of patients who do get better and are sent home, we could argue that they could have just been seen at the GP clinic and not visited the ED.
How are Singapore hospitals dealing with an unprecedented COVID-19 surge? Listen to CNA's Heart of the Matter:
However, in the case of the latter group where treatment had to be escalated and reviewed, the situation could have taken a turn for the worse if they waited at a GP clinic.
As the ED stands as the last line of defence for patients, we have to stay vigilant when observing these patients. These isolation observation beds became added physical constraints in the ED and required an increase in manpower to attend to patients.
Although the Government has since changed its stance on the guidelines to receiving medical care when one tests positive for COVID-19, we still see that the fear of contracting the disease is prevalent. This fear drives patients to seek comfort and assurance at the ED.
It will take some time for Singapore to accept COVID-19 as endemic and learn to live with it, and perhaps when they do, we might see a lesser patient load in the ED.
STRAIN ON HEALTHCARE WORKERS
As healthcare professionals, it is our responsibility to protect the acute hospital beds for patients who require admissions.
That said however, we have to attend to every patient who arrives at our door, because no health concern is considered too minor. This means spending time on firstly, treating the patient, secondly, talking to parents and explaining the situation, and thirdly, making the necessary arrangements.
The time spent doing this is amplified during the recent Omicron surge with the hundreds of patients that we face. We do our best to balance this group with those who need emergency care.
But naturally, given our resources, this results in very long waiting times. For now, when there are too many mild or generally well patients who show up at the ED, it does contribute to a strain in the healthcare system.
Waiting times in a clinic is quite different from that of an ED – here, time is critical and makes a significant difference to clinical outcomes.

SEEKING RESPONSIBLE CARE AT THE RIGHT TIME, RIGHT PLACE
We are very fortunate to be in Singapore where medical care is easily accessible. Patients can visit the ED through various means: An ambulance via the "995" emergency hotline, private transport or simply walk-ins.
Even before the COVID-19 pandemic took place, there were occasions when patients with mild flu or conditions that seem to be of lower acuity would turn up at the ED.
But during a pandemic, the act of seeking responsible care at the right place and right time becomes much more important. When the patient load is unnecessarily heavy, it can take a toll on frontliners.
Unlike other professions where working from home is possible, the increase in patient load at the ED during the pandemic means that ED staff have no choice but to double up, do back-to-back shifts or come back on weekends so we can cope with demand.
But more importantly, our ability to provide the necessary care to emergency cases is affected.
If patients understood the repercussions and accessed healthcare more responsibly, we can also ensure the well-being of our frontliners, especially those in the ED.
Much effort has been put in to educate the public not to turn up at ED in hospitals for COVID-19-related symptoms that are mild and can be treated at home.
With the advancement of technology, alternative consultation methods such as telemedicine are now widely available; allowing patients to consult a GP in the comfort of their home.
I believe we have done well as a nation over in the last two years when the Government stepped in swiftly and poured in the necessary resources to control the pandemic.
Policies such as vaccinating as many Singaporeans as possible have come a long way in containing the virus. Travel restrictions are gradually lifting, for instance. As frontliners, we hope to see the endpoint of this pandemic – and that is when we can all treat this virus as endemic.
Dr Devin Tan is a Specialist in Emergency Medicine at Raffles Hospital.
















