Delivering a baby in isolation: The challenges of getting COVID-19 while pregnant
-
If a pregnant woman contracts COVID-19, there are greater complexities, including the possibility of a premature baby if the mother develops severe pneumonia
-
SGH says it has yet to see a pregnant patient with COVID-19 who is fully vaccinated, only "very, very few" are partially vaccinated
-
Getting vaccinated may not prevent you from contracting the virus, but it will help in terms of less severe symptoms, says a mother who contracted COVID-19 when she was pregnant and unvaccinated
SINGAPORE: It began with a runny nose.
Ms Vanessa Rickard, 36, didn’t think much of it because it was like “a normal cold” that she had a few months ago. Then came the fatigue, a dry cough and losing her sense of smell.
Ms Rickard tested positive for COVID-19 when she was 37 weeks pregnant, and was admitted to the Singapore General Hospital (SGH) on Aug 17.
She was not vaccinated against the virus.
“I also had the aches and pains of being 37 weeks pregnant. You know, backaches, joint pains, heartburn … which complicated the whole thing,” she told reporters in an online interview organised by SGH on Thursday (Sep 16).
“Thankfully I had no comorbidities so my symptoms were not that severe, but I can imagine it would be more difficult for a pregnant woman with, say, asthma or some other illness. I didn't expect my symptoms and admission to last that long though. I guess with lower immunity during pregnancy this was expected,” she told CNA separately over email.
When Ms Rickard found out she was pregnant in December last year, there were “not much studies yet on the effects of the vaccine” on the foetus and pregnant mothers then, so she was hesitant to get vaccinated.
“I weighed the risks involved and just decided that maybe I’ll just wait until I give birth then get the vaccination after that. … Of course I didn’t expect to get the virus during my 37th week,” she said.
A week after being admitted to SGH, she delivered her second child in the isolation ward on Aug 24.
ISOLATION "HARDEST PART"
The hardest part of battling COVID-19 while pregnant was being isolated, said Ms Rickard.
“There was the mental (hurdle) that I had to go through with no family members, no one could visit, and being anxious and uncertain of what must happen,” she said.
“I decided to be separated from my baby. It was two-and-a-half weeks that I didn’t get to see my baby at all. It was just via FaceTime. It was really hard not seeing my family.”
Related:
On top of the mental strain, she found out her entire family (her husband, her toddler, and her helper) had also contracted the virus one day after she gave birth. Her husband and helper were vaccinated.
But even though their symptoms, including her toddler’s, were mild, it was “one of the most difficult times and experiences” she had been through.
After giving birth, it would be another two weeks in isolation before she was discharged, after testing negative for COVID-19.
DELIVERING A BABY WHILE COVID-19 POSITIVE
Ms Rickard’s stay was made slightly easier with the “smooth” delivery process in the isolation ward. She recalled about four to five people assisting with the delivery, and “everyone knew their roles”.
“I trusted the doctors that they knew what they were doing. They also spoke to me via Zoom that morning talking about the procedure that they were going to do. They did a simulation as well for the whole process. It was all like clockwork; everyone was really prepared,” she said.
Doctors who helped in Ms Rickard’s delivery explained that the simulation run involved several departments.
These included nurses who ensured no one breached safety measures that could lead to transmission of COVID-19, and the IT department which arranged the Zoom meetings with the patients.
This meant “bringing the labour ward to (Ms Rickard)”, said Dr Tan Wei Ching, senior consultant at the Department of Obstetrics & Gynaecology.
“Besides the delivery trolley, there was equipment for the delivery, medications for obstetric emergencies (and) the resuscitator that (we) had to bring. Once the labour started, we had a one-to-one midwifery care, so we parked a nurse and a doctor there all the time to assess our progress.
“We also had a dedicated operating theatre for the (COVID-19 positive) patients, and the theatre was on standby, in case there was any emergency that needed the baby to be delivered by Caesarean section.”
Dr Sridhar Arunachalam, a consultant at the Department of Neonatal & Developmental Medicine, added that isolating the baby from Ms Rickard after delivery also took much coordination.
“(The isolation ward) is a new place for us, so we need to find the ideal location where we can get the oxygen supply … and to establish all the equipment in this place is also a challenge. But our nurses and other teams helped us, so we had the set-up ready when we received the baby,” he said.
“The security was also very helpful for the transport of the baby from the isolation ward to the neonatal ICU. We had to move a few storeys down, so they got everything ready for us, including specified lifts, for transferring the baby.”
In fact, Ms Rickard's baby, Kai Cruz, was the first to be born in the hospital’s isolation ward.
CARING FOR PREGNANT WOMEN WITH COVID-19
Since August, SGH has seen more than 10 cases of COVID-19 positive pregnant women admitted to its isolation ward, up from none in July.
“Almost all of them are unvaccinated, and only very, very few are partially vaccinated. I have yet to see fully vaccinated COVID-19 positive pregnant patients in our hospital at this point,” said Dr Benjamin Cherng, senior consultant at the Department of Infectious Diseases.
Dr Cherng understands that many pregnant women like Ms Rickard don’t get vaccinated because “it is all about the baby” and they’re worried that they might harm their unborn child.
In email responses to CNA, experts from SGH elaborated that the reasons for not getting vaccinated include fear that their baby may get COVID-19 from the vaccination, and worry that the vaccination might cause miscarriages, fetal malformations, growth restriction, prematurity and stillbirth.
Some unvaccinated mothers also worry about the effects of vaccination as they have allergies and other comorbidities, like cardiac disease, hypertension and diabetes, experts added.
Finally, they worry about the symptoms of vaccination, such as fever and body aches, and how these would affect the baby.
“Decisions are all about risk versus benefit, and some are admittedly easier to make than other decisions. It’s actually a careful deliberation by the (Ministry of Health’s Expert Committee on COVID-19 Vaccination) … where there was the recommendation that pregnant patients should receive the vaccination,” added Dr Cherng.
“This is based on our current knowledge that the vaccines do work, and that they’re safe for the mother as well as for the foetus. Certainly the benefits of vaccination right now outweigh the risks of acquiring COVID-19 and its complications.”
Additionally, the Ministry of Health's website states that "there is no evidence to suggest that the Pfizer-BioNTech/Comirnaty or Moderna COVID-19 vaccine may cause harm to pregnant women or their babies".
The website adds that these mRNA vaccines are "biologically unlikely to adversely affect breastfed babies". In fact, the breast milk of vaccinated mothers "may help to protect their babies from COVID-19 due to antibodies in breast milk".
After all, if a pregnant woman contracts COVID-19, there are greater complexities.
Between non-pregnant and pregnant patients, the latter are at a higher risk of getting “more severe COVID”, said Dr Cherng.
“When they do develop complications of severe COVID pneumonia, then (we need) to consider the physiology (in) pregnant women, which is certainly different from non-pregnant patients. On top of that, there’s the all-important presence of a foetus, which needs to be considered in every treatment decision.”
Pregnant women are already at risk of getting thromboembolism – blood clots in the leg, added Dr Tan. This risk increases if the patient has COVID-19.
“The second thing is that some of these mothers, if they have severe pneumonia from COVID, there's always a consideration that we need to deliver the baby a little bit earlier. And that can result in a baby who's premature, with all the complications of prematurity,” she said.
Dr Arunachalam added that such complications are greater if the baby is “extremely premature”, such as 24 to 25 weeks old, while they might lessen if the baby is closer to the term gestation.
"ONE DOSE IS BETTER THAN NOTHING"
The three doctors from SGH concurred that all pregnant women should get vaccinated if they’re eligible.
“Anytime after 12 weeks (as that’s when foetal formation is complete), we really talk to our patients and encourage them to consider having a vaccination. It doesn’t matter at what stage of their pregnancy they are, one dose is better than nothing. Some protection is better than none,” said Dr Tan.
She added that the risk of miscarriage, premature labour or having small growth-retarded babies is not higher in vaccinated patients.
“In fact, it’s COVID-19 itself that will cause more pregnancy-related complications, whether it’s miscarriages or late miscarriages like preterm labour, as well as even stillbirth of the baby, if the mother gets very, very sick.”
After going through pregnancy and COVID-19, Ms Rickard now encourages all pregnant women to get vaccinated “as soon as they can”.
“More studies have come out now and have proven that the benefits outweigh the risks for the mother as well as the baby. It may not prevent you from contracting the virus, but it will definitely help in terms of less severe symptoms or from being hospitalised,” she told CNA over email.
Come November, three months after recovering from COVID-19, Ms Rickard will finally get her first dose.
BOOKMARK THIS: Our comprehensive coverage of the COVID-19 pandemic and its developments
Download our app or subscribe to our Telegram channel for the latest updates on the coronavirus pandemic: https://cna.asia/telegram










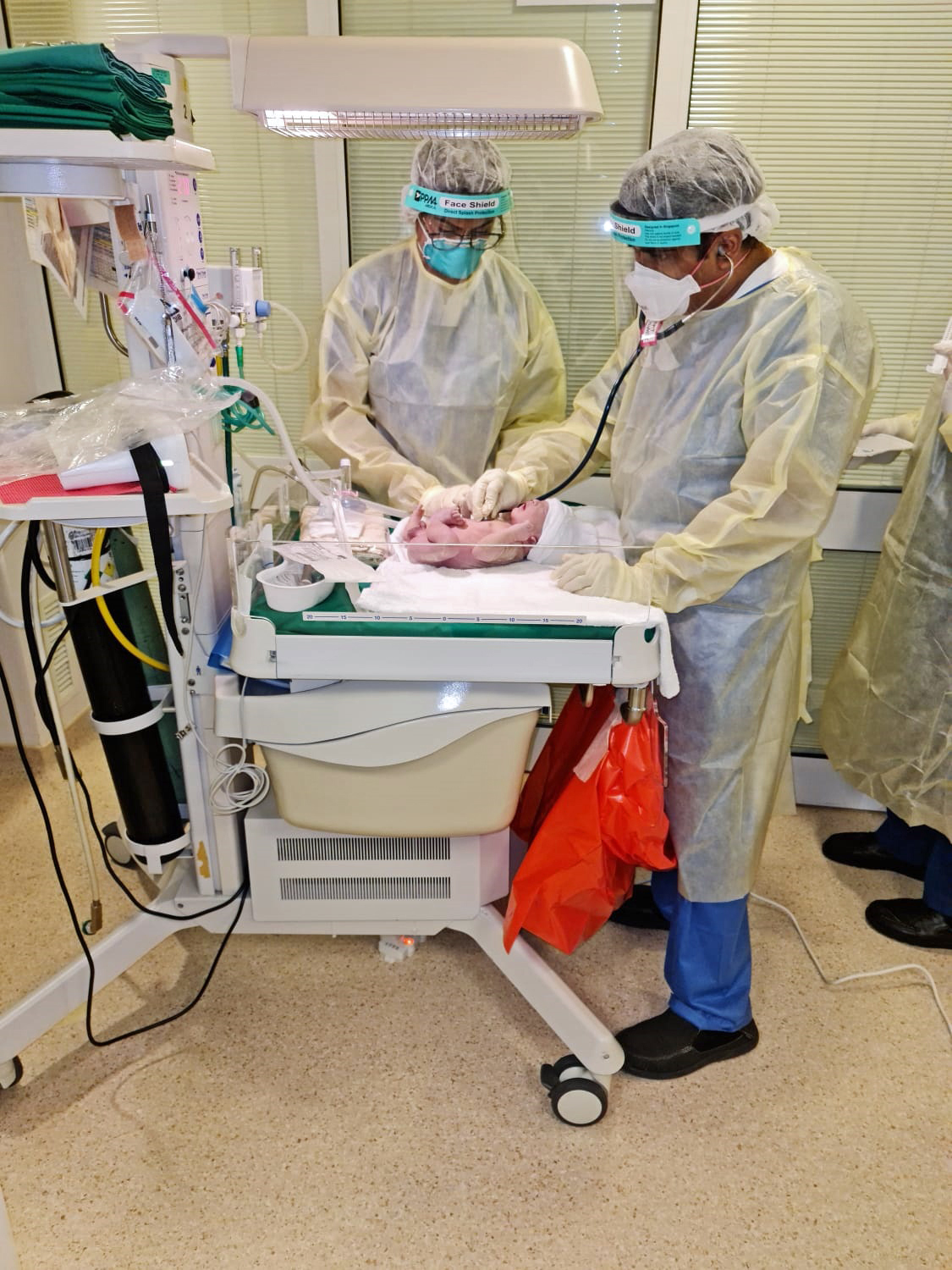 Dr Sridhar Arunachalam examining Ms Rickard's baby in the isolation ward. (Photo: Singapore General Hospital)
Dr Sridhar Arunachalam examining Ms Rickard's baby in the isolation ward. (Photo: Singapore General Hospital)  Ms Rickard and her newborn son. (Photo: Vanessa Rickard)
Ms Rickard and her newborn son. (Photo: Vanessa Rickard) 




