Indonesia’s measles outbreaks need more than mass immunisation campaigns as solutions, say experts
One of the worst-hit areas is Sumenep in Madura Island, East Java, which has recorded more than 2,000 suspected infections and deaths of 17 children.
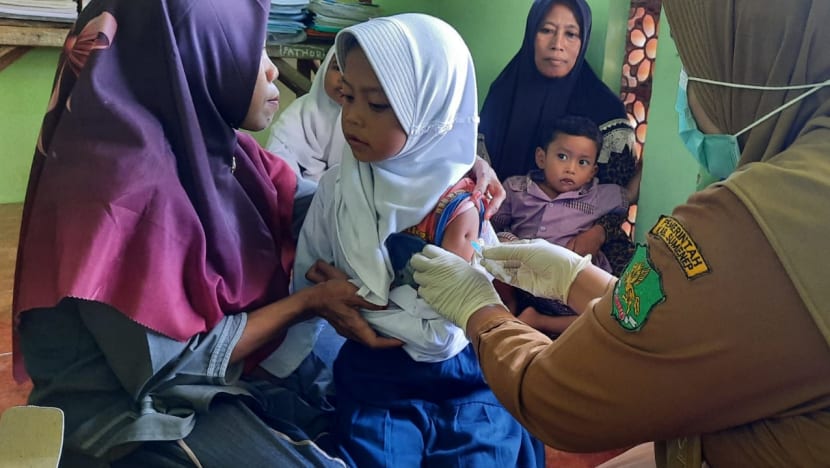
Measles vaccination in Sumenep's Bluto subdistrict Health Centre, East Java, Indonesia. (Photo: Bluto subdistrict Health Centre)

This audio is generated by an AI tool.
JAKARTA: Every time a free school vaccination drive is held, Benzema (not his real name) would keep his children at home. Sometimes the excuse is illness, but the underlying reason is always the same: distrust.
The 40-year-old small business owner from Bekasi, West Java, believes vaccines actually weaken the body’s immunity.
“None of my eight kids has been vaccinated since they were babies,” he told CNA, adding that he has done extensive read-ups about vaccines.
Health workers and experts warn that such attitudes have contributed to a steady decline in vaccine coverage in Indonesia — opening the door to the resurgence of vaccine-preventable diseases.
Over the past few weeks, Indonesia has recorded dozens of measles outbreaks.
One of the worst-hit areas is Sumenep in Madura Island, East Java, which has recorded more than 2,000 suspected infections and deaths of 17 children. The other two hotspots besides Sumenep are Medan (351 suspected cases) and Deli Serdang (154), both in North Sumatra province.
Authorities say reluctance to participate in vaccination programmes is the leading cause. In response, health officials launched a mass immunisation campaign, known as Outbreak Response Immunization (ORI), which runs from Aug 25 to Sep 6 in Sumenep.
Ellya Fardasah, Head of the Sumenep Health, Population Control and Family Planning Office (Dinkes P2KB), told CNA that vaccines will be administered to 78,569 children aged nine months to seven years.
“Our target is 95 per cent of that figure, which amounts to 70,271 children. The daily goal is 4.8 per cent or 3,346 children within that age range,” Ellya said.
But experts believe that sustainable progress in vaccination coverage requires more than campaigns — it demands community-based education, particularly from religious leaders, to counter disinformation and to convince families that vaccines are vital to children's safety.
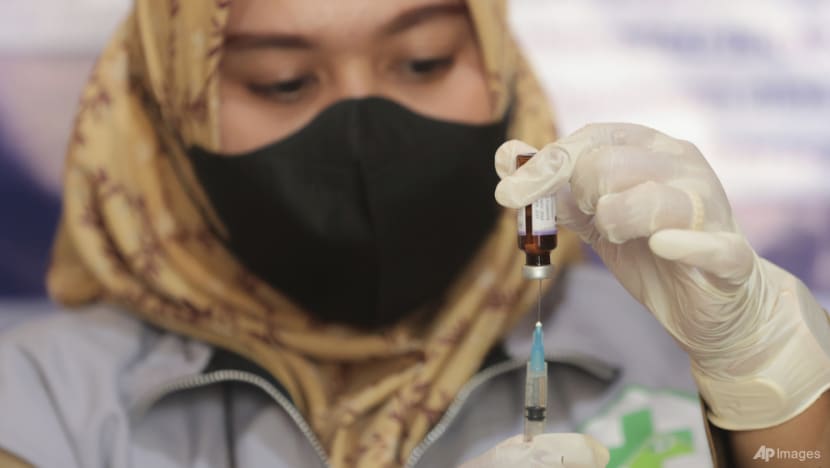
VACCINATION IN DECLINE
Measles is caused by a highly contagious virus transmitted via respiratory droplets from coughs or sneezes. Symptoms include high fever, cough, runny nose, red eyes, and a tell-tale red rash that starts on the face and spreads throughout the body.
As of Aug 24, Indonesia’s Ministry of Health confirmed 46 laboratory-verified measles outbreaks in 42 regencies and cities across 14 provinces, its director of immunisation Prima Yosephine Berliana Tumiur Hutapea said at a press conference on Tuesday (Aug 26).
Nationwide, the cumulative number of suspected measles cases recorded this year has reached 23,128 as of August 2025.
Of that figure, 20,710 samples have been examined in laboratories, with results confirming 3,444 positive cases, said the director. This marks a sharp increase from previous years, which saw 10,628 cases in 2023 and 3,520 in 2024.
This places Indonesia’s measles positive rate — the proportion of laboratory-confirmed cases among those tested — at 16.6 per cent in 2025. In comparison, Indonesia recorded 25,639 suspected cases in 2024, with 22,493 specimens tested and 3,520 confirmed positive — a slightly lower positive rate of 15.6 per cent.
Indonesia’s Ministry of Health attributes the continued spread to uneven vaccine distribution as well as low immunisation coverage.

Since 2023, Indonesia’s measles vaccine coverage has consistently fallen short of the 95 per cent threshold required for herd immunity. That year, coverage for the second dose of the measles-rubella vaccine stood at 86.6 per cent. In 2024, it dropped further to 82.3 per cent.
Authorities in Sumenep, East Java, have declared a measles outbreak after reporting 2,139 cases — including 205 lab-confirmed infections — and 17 deaths as of August 24.
In Sumenep’s Bluto subdistrict, 79 children have been infected, according to Bluto Health Centre head Rifmi Utami.
Treatment decisions are based on severity, Rifmi said. “Mild cases are treated and isolated at home with high-dose vitamin A. Severe cases require hospitalisation.”
One of the most tragic cases involved a four-year-old child who died despite being rushed to hospital. Five children are currently hospitalised, she added.
“Measles deaths are usually not from the virus alone but from complications like pneumonia, brain inflammation, or seizures,” Rifmi explained.
Ellya noted that most current patients had no history of vaccination.
“Currently, 89 per cent of suspected measles cases among one-year-olds to four-year-olds in Sumenep were not vaccinated, and none of the children who died had received the measles vaccine,” she told CNA.
Indonesia has had a national measles vaccination programme since 1984. Children are typically given two doses: the first at nine months old, and the second during the first grade of primary school under the School Children's Immunisation Month campaign.
Still, recent figures show that Sumenep’s 2024 full basic vaccination coverage is only at 84.52 per cent — well below the 95 per cent target. Ellya warned that this shortfall is directly linked to the measles outbreaks in the region.
“The high number of measles-related deaths is a consequence of incomplete vaccine coverage,” she said.
THE COVID-19 PANDEMIC AND ACCESS BARRIERS
Experts say the current situation is partly a delayed impact of COVID-19. During the pandemic, mobility restrictions prevented many children from receiving their first measles shot at nine months of age.
“All routine vaccination programmes should have continued. Now, we’re seeing a vaccine backlog,” said Windhu Purnomo, a public health lecturer at Airlangga University. “A child should be vaccinated at nine months, but many missed it. Two or three years later, they got infected.”
Dicky Budiman, an epidemiologist at Griffith University in Australia, agreed. “Health services disrupted during the pandemic have not fully recovered,” he said, pointing to missed appointments and broken vaccine schedules.
Logistical hurdles and access limitations in rural areas further complicate the situation. According to Dicky, local-level planning remains inconsistent. “Village-level micro plans are often not detailed — not by name, not by address — so dropouts went unnoticed.”
These structural issues, combined with vaccine hesitancy, are accelerating the spread of measles — a virus with a basic reproduction number (R₀) of 12 to 18, meaning one infected child could infect up to 18 others.
“This virus spreads incredibly fast,” Dicky warned, urging urgent national containment measures.
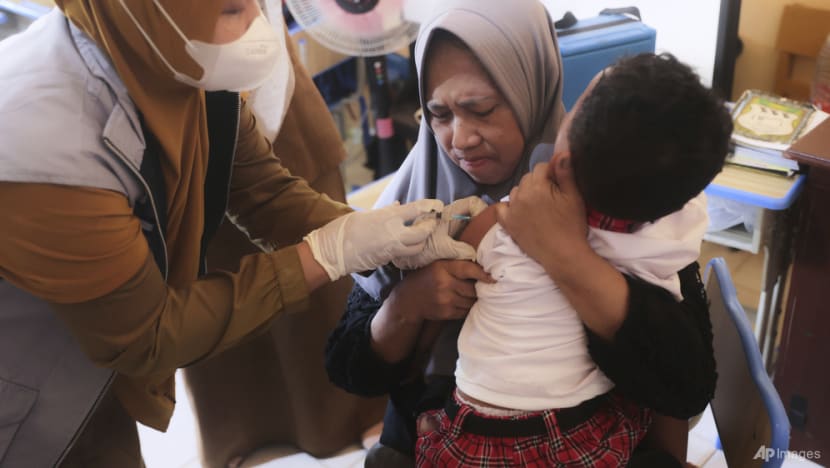
According to Ellya, a reluctance to vaccinate children is a major reason for the low coverage in her region.
The reasons vary from fear of side effects, concerns over fussiness in children, distrust in vaccine efficacy, peer influence, to widespread misinformation — especially hoaxes claiming vaccines are unsafe or religiously forbidden.
“At Bluto, one anti-vaxxer can sway many others. Some claim vaccines are haram,” said Rifmi, using the word that means forbidden in Islam, which is the majority religion in Indonesia.
Some individuals, like Benzema, reject all vaccines, including COVID-19 shots. He cited a widely circulated (but debunked) 2024 claim that the pharmaceutical company Pfizer apologised for vaccine-related deaths and paralysis.
Even after being shown a fact-check report by local media Tempo debunking the claim, Benzema stood by his view: “The point is, my family’s healthy, thank God.”
Similar sentiments come from Setiawan, a resident of Citayam, Depok.
“People in the old days weren’t vaccinated and still lived long lives.”
Rifmi clarified that vaccinated children can still get measles, but symptoms are milder and complications far less likely. “Vaccination won’t make you invincible, but it prevents severity and death,” she said.

SPREADING TRUST AND RAISING AWARENESS
Dicky from Griffith University believes hardcore anti-vaxxers are few in number. But the bigger challenge is the large group of hesitant parents.
“Vaccine hesitancy is fuelled by hoaxes and infodemic, combined with service disruptions — these are the biggest contributors to declining coverage,” he said.
In localised outbreaks, the impact is stark. “Even if just 10–20 per cent of parents in a community hesitate, measles protection drops drastically,” Dicky explained, due to the virus’s high transmissibility.
To counter this, Dicky urged culturally sensitive community outreach involving trusted local and religious leaders, including figures from the Indonesian Ulema Council (Majelis Ulama Indonesia, MUI), Nahdlatul Ulama (NU), and Muhammadiyah — three of the country’s most influential Islamic organisations.
“The message must be unified: vaccines are permitted, halal, and necessary.”
He suggested tangible messaging: “Show MUI’s statement that vaccines are halal. Share local vaccine data. Tell real survival stories. Hold public forums. Use local language and culture. Emphasise empathy and child protection.”
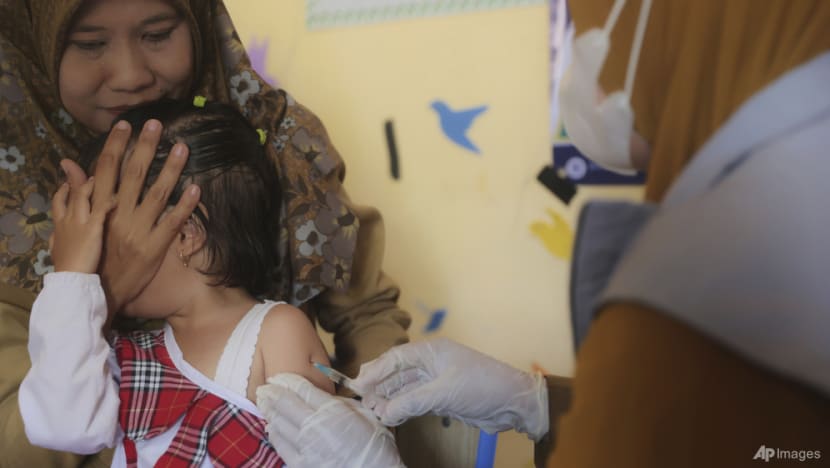
Meanwhile, Windhu emphasised that vaccines remain a personal right under Indonesian law — and cannot be legally enforced.
Still, he encouraged community pressure. “Let society create social sanctions based on local customs so those who refuse vaccination feel ashamed.”
Indonesia’s Ministry of Health has urged parents and caregivers to immediately take their children to the nearest health facility to receive measles immunisation, whether through routine vaccination or additional doses provided during outbreak response campaigns, according to the official schedule.
The ministry also called on the public not to postpone or fear immunisation. “Measles vaccines are safe, of high quality, and provided free of charge by the government to protect children from a disease that can cause serious complications, even death,” said Prima from the Ministry of Health.
“The government guarantees this, as the vaccines have already been approved for distribution. Do not believe in negative news. Consult with healthcare workers or community leaders, so hoaxes do not mislead you,” she added.
Rifmi and her team continue with door-to-door efforts, showing patience and persistence. As part of the measles response, Bluto Health Centre will also conduct a sweeping campaign to ensure no child is left out of vaccination.
“Each community is different. But we won’t give up. We’ll keep urging parents because measles is preventable,” she said.




















