Commentary: Where does traditional Chinese medicine fit into Singapore’s healthcare reform plan?
Innovation and a change in mindset are needed if traditional Chinese medicine is to be accepted as mainstream medicine, says this industry practitioner.
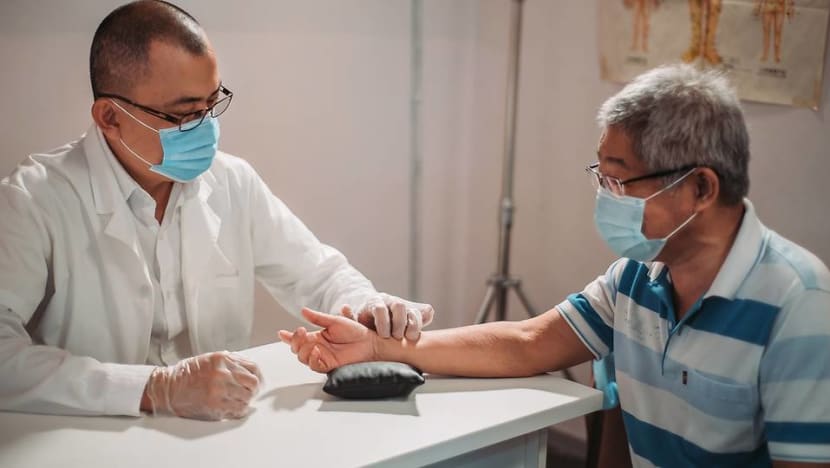
SINGAPORE: What goes through your mind when someone suggests you try traditional Chinese medicine to boost your immune system, or acupuncture to help ease your chronic pain?
Do you picture a strong-smelling herbal shop with a man reading your pulse and looking at your tongue and think, “Thanks, but I’ll stick to my vitamins”? Or do you voice doubt on how needles instead of lab-tested Western medicine will be able to take away your pain?
Interest in TCM, which has been used for thousands of years to treat and prevent diseases, is undergoing a revival given the unique health challenges of the 21st century, the World Health Organization wrote in its Global Report on Traditional and Complementary Medicine 2019.
More countries are also recognising the role of TCM in their national health systems, with around 100 member states having national policies on traditional medicine, it said.
In Singapore, about half of Singapore’s population has visited a TCM practitioner before, Health Minister Ong Ye Kung said in a speech at the World Conference on Acupuncture-Moxibustion on Nov 19.
Despite the popularity of TCM, the reality is that traditional medicine is still not on par with Western medicine in terms of official recognition.

PLANS FOR TCM IN HEALTHCARE SYSTEM
Singapore is rolling out a healthcare reform plan called Healthier SG, which focuses heavily on preventive care to tackle the challenges of an ageing population and rising impact of chronic illness.
The key features of the plan include: Mobilising family doctors to deliver preventive care for residents; developing health plans that include lifestyle adjustments, regular health screening and appropriate vaccinations; activating community partners to support residents in leading healthier lifestyles; and rolling out a national enrolment exercise for residents to commit to seeing one family doctor.
The Healthier SG plan is largely modelled upon contemporary medicine. But TCM and other forms of traditional medicine could make it a truly comprehensive and holistic system.
At the parliamentary sitting last month, Health Minister Ong Ye Kung said that the Government is exploring ways to incorporate TCM in the plan.
This is encouraging.

HOW CAN TCM COMPLEMENT HEALTHIER SG
TCM pays attention to the body constitution and manages functional disorders and sub-health conditions that can remain largely undetected with medical examination, dissection or even under a microscope.
It also emphasises harmonisation with the environment and balance of two opposing attributes called Yin and Yang. These can be achieved by adopting work-life balance, a healthy diet, exercise, food therapy, and treatment with medication if needed.
These concepts and methods are in line with the disease prevention measures covered in the White Paper for Healthier SG.
Based on the existing framework, it seems that there is room for TCM to complement it in stages.
At the initial stage, it is easier to commence with preventive healthcare as it does not involve the issue of TCM complicating the medical intervention for serious and acute illnesses.
For example, individuals can be given opportunity to be exposed to the fundamental concepts of harmonisation, body constitution and Yin-Yang balance. The opportunity is there for this information to be disseminated via the Health Promotion Board and community set-ups including TCM institutions.
TCM food therapy can also be taught to enrich dietary selection for preventive care. Body constitution assessment and Yin-Yang measurement scores can be quantified and made available for self-monitoring using mobile apps, with food property charts included for easy daily reference.
If TCM information and therapies are made available officially, it will provide additional motivation for people to practise preventive healthcare and help reduce the need for hospital attention.
INCORPORATING TCM IN MEDICAL ESTABLISHMENTS
Apart from being used as preventive healthcare, there is a case to be made for TCM to be incorporated in medical establishments such as step-down care, polyclinics and hospitals.
Acupuncture services are already offered at several hospitals. For example, Sengkang General Hospital’s acupuncture service provides treatment for mainly chronic pain patients when conventional treatment is either contraindicated or unable to provide desired pain relief.
The National University Hospital has an acupuncture clinic, while Singapore General Hospital’s Pain Management Centre offers acupuncture as an alternative treatment, and Tan Tock Seng Hospital has a Complementary Integrative Medicine Clinic that offers acupuncture, cupping and TCM medicinal herbs. Khoo Teck Puat Hospital also offers acupuncture and cupping.
More can be done in this area.
MANY HURDLES
There are many hurdles for TCM to gain more recognition in a public healthcare arena dominated by Western medicine.
First, evidence-based medicine must be used to prove the efficacy of TCM. In this area, the MOH in 2014 launched a TCM Research Grant. One of its objectives is to assist policymakers by providing clinically proven treatments to serve the healthcare needs of the public.
In the area of TCM research, progress has been made over the last decades locally and overseas, particularly in China. But much of this research might have gone unnoticed due to the use of non-Western or non-English means of publication.
Hence, it may be meaningful to conduct a regular systematic review of all research literature to assess the increasing availability of evidence over time. This could provide useful information to facilitate policymakers in giving recognition to TCM in tandem with the production of efficacy evidence.
Second, there is a dearth of professionals in the TCM sector. As of 2021, there were about 3,320 registered TCM practitioners in Singapore, comprising both physicians and acupuncturists. This compares with more than 15,000 doctors, comprising both specialists and non-specialists.
The TCM sector is not known to have great professional advancement opportunity or high salaries, which may deter youngsters in pursuing TCM as a career.
During my tenure as director of the Biomedical Sciences and Chinese Medicine programme at Nanyang Technological University, I noticed a low percentage of registered physicians practising TCM full time. There were also students who opted out of the TCM programme during their course selection, resulting in another concern over succession and sustainability.
The current community-supported system – mainly in Chinese medicinal halls and charitable TCM clinics - portrays an image that TCM is cheap, unrefined and of low standard. There are private TCM clinics, of course, but without stronger official recognition, TCM will continue to be perceived as a low-value healthcare service.
INNOVATIVE MINDSET NEEDED
At this juncture, an open and innovative mindset, and the willingness to recognise a different concept and practice is needed if TCM is to play a part in Singapore's healthcare future.
If we are committed to empowering individuals to take charge of their own health, the wide acceptance of TCM by many users for preventive treatment could be the very endorsement it needs for its efficacy.
As the saying goes, “all beginnings are hard”. If we believe in the possibility of establishing a world-class healthcare system, we will have to act innovatively to begin the integration of contemporary science with ancient wisdom to surpass countries that rely solely on modern medicine.
Such a unique system could enlarge the red dot on the world map and give Singapore an edge to realise the huge economic potential of holistic and integrative healthcare.
Dr Goh Chye Tee is a registered TCM physician. He is also the former director of the NTU Chinese Medicine Clinic and the Biomedical Sciences and Chinese Medicine programme at Nanyang Technological University, Singapore.

















