Commentary: Retention bonuses may help reduce attrition in short term, but won’t fix problems in nursing
Singapore is desperately in need of more nurses as its population ages, but money alone won’t help solve the issues in the profession, say two public health experts.

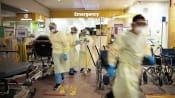
Tired healthcare worker in Singapore. (Photo: iStock)
SINGAPORE: A nurse’s primary role is to care for patients, see to their needs and help them achieve their health goals. As part of that, they work long hours and overnight shifts, risking injury and illness to themselves.
But beyond that, they are also the go-to person for patients’ families, providing emotional support and answering their questions. Then there’s the administrative work.
The announcement last week of a special retention bonus for nurses in the public sector is welcome news.
It demonstrates the Government’s recognition of the value of our nurses and signals willingness to invest to attract and retain talent. However, while money is important of course, it cannot paper over inherent structural issues Singapore has to address.
What are some of these structural issues? A McKinsey survey of nurses in six countries including Singapore published in May 2022 revealed “the most important factors keeping them in their direct-patient-care roles included doing meaningful work, a positive and engaging work environment, and feeling healthy and safe”.
Let’s dissect these. Meaningful work for most nurses would typically mean direct patient care. Administration is of course important but how do we keep it to a minimum?
As Singapore embraces becoming a Smart Nation with copious amounts of data collection and documentation for Big Data analytics, nurses often bear the brunt of the data collection and entry. How do we strike the right balance?
Meetings are an essential reality of organisational life but they take away from the core roles in direct patient care - what is the right balance?
HELPING NURSES FEEL SAFE
On the work environment, there is ample evidence from the fields of sociology and organisational behaviour that people stay on their jobs because of a sense of meaning and purpose attached to the work.
Achieving success, job progression, acquiring new skills and capabilities, being recognised and rewarded all contribute to job satisfaction.
Here the Ministry of Health deserves due credit for its work over the last decade in redesigning career paths, creating multiple opportunities for nurses to upgrade skills, develop new job roles and practise at ever-higher levels of expertise to improving patient care at individual and system levels. Perhaps more needs to be done for more nurses, but the frameworks exist and the commitment is evident.
When it comes to helping nurses feel “healthy and safe”, I fear we collectively have let our nurses down. The healthcare ethos is that patients come first which is admirable, but one cannot pour from an empty pot.
At the societal level, how often do we hear nurses being derided as just bedpan changers and verbally abused by patients or relatives?
At the organisational level, the manpower shortage is such that some nurses find it a challenge to take time off.
In an article by CNA Insider, a nurse at a public hospital spoke of how she was accused of being “selfish” when she requested for leave to care for her father who had contracted COVID-19.
RISE IN ABUSE CASES
Then there’s the abuse they face. There were about 1,400 abuse and harassment cases reported as of end-November last year, up from 1,300 cases in 2020, 1,200 cases in 2019 and 1,080 cases in 2018.
Retention bonuses may be necessary as a stop-gap short-term measure to reduce attrition, but in the long run, other factors are more important to address decisively.
Interestingly in the May 2022 McKinsey survey, pay was not reported as a top-three factor in respondents’ decisions to leave nursing in any of the countries surveyed except Japan.
The Financial Times in a June article described a “global crisis in nursing”, and it won’t get better for Singapore.
With population ageing and rising burden of chronic diseases, we will desperately need more nurses both local and foreign.
We as a society and country get the number of nurses we deserve. Let’s fix nursing and make sure we deserve the nurses Singapore needs.
Associate Professor Jeremy Lim is director of the Leadership Institute for Global Health Transformation at the NUS Saw Swee Hock School of Public Health.
Dr Lim Huai Yang is a public health specialist with an interest in organisational health.