New eczema treatments available in Singapore, but high costs keep them out of reach
Targeted treatments have emerged as a safer and more effective option for eczema patients, but high costs remain a barrier.
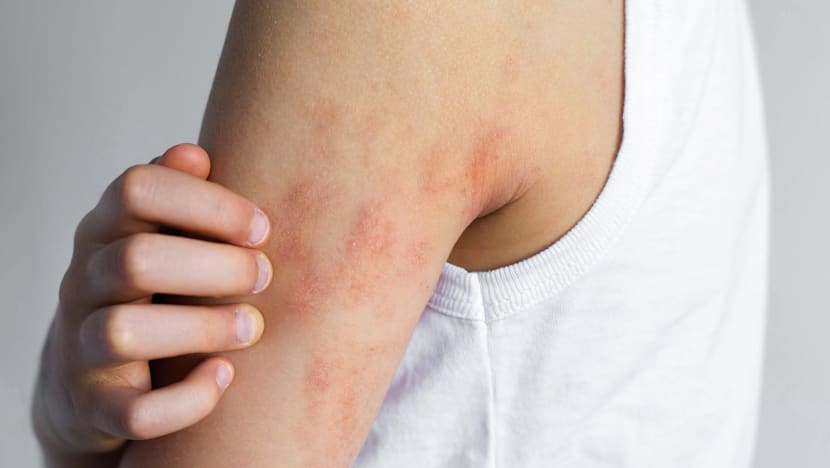
Eczema affects one in five children and one in ten adults in Singapore. (Photo: iStock/Evgeniia Gordeeva)

This audio is generated by an AI tool.
SINGAPORE: At the height of her eczema flare, Ms Chloe Ng struggled to hold a pen or carry a spoon as her fingers were covered in open wounds.
For years, she cycled through treatments, including oral steroids and immunosuppressants. While they provided some relief, they also came with significant side effects.
A turning point came in 2021, when she tried new treatments at the National Skin Centre. An oral Janus kinase (JAK) inhibitor – a drug that blocks specific immune responses – worked best.
“I live a normal life after taking this new medicine. Otherwise, I can't sleep. Since 2008, until the day before I tried the new medicine, I didn't sleep well for all these years,” said Ms Ng, 43, who first developed eczema in her 20s.
Atopic dermatitis, the most common form of eczema, is a chronic inflammatory disorder affecting about one in five schoolchildren and one in 10 adults. It causes itchy, dry and inflamed skin.
Newer targeted therapies, such as JAK inhibitors and biologics, have emerged as safer, more effective options for moderate to severe cases. But their cost puts them out of reach for many.
The JAK inhibitor cleared about 95 per cent of Ms Ng’s eczema, but costs about S$1,200 (US$940) a month. She now takes a more affordable medication to manage her condition.
“Eczema is what our grandmothers call ‘rich people’ kind of sickness,” the talent manager said in Mandarin. “Because if you are financially okay, you can buy better medicine to treat yourself. But if you don’t have money, you have no choice. You just take cheaper medicine.”
BREAKTHROUGH TREATMENTS
Most eczema patients can manage their condition with topicals, moisturisers and trigger avoidance, said Dr Yew Yik Weng, a senior consultant dermatologist at the National Skin Centre.
About 20 per cent of those whose disease is not well controlled may need systemic treatment.
For years, severe cases typically relied on oral immunosuppressants, which broadly dampen the immune system to reduce inflammation and itching.
But these drugs can have significant side effects, including high blood pressure and increased risk of infections. Long-term immunosuppression has also been associated with a higher risk of certain cancers.
It was not until 2019 that Singapore approved the use of a biologic drug – dupilumab, known by its brand name Dupixent – to treat moderate to severe eczema. Unlike immunosuppressants, biologics target specific immune pathways activated during eczema flare-ups.
The theory is that if you only block that singular pathway, you can control the eczema without widespread immune suppression, said Dr Yew.
JAK inhibitors followed in the early 2020s, blocking enzymes involved in the immune signalling that drives inflammation.
What are biologics and JAK inhibitors?
Biologics and JAK inhibitors are targeted therapies used to treat moderate to severe eczema, among other autoimmune conditions.
Biologics are injectable drugs that work by blocking specific immune proteins responsible for inflammation. Approved options in Singapore include dupilumab (Dupixent), lebrikizumab (Ebglyss) and nemolizumab (Nemluvio).
JAK inhibitors are oral medications that block specific enzyme pathways inside immune cells, reducing inflammation and itching. These include upadacitinib (Rinvoq), abrocitinib (Cibinqo) and baricitinib (Olumiant).
The treatment option depends on the patient. In general, biologics have better safety data, while JAK inhibitors have better efficacy data, said Dr Uma Alagappan, a dermatologist at The Dermatology Clinic.
Biologics are associated with side effects such as eye inflammation and injection-site reactions. JAK inhibitors carry warnings about cardiovascular complications and blood clots, and require regular blood monitoring.
Dr Uma Alagappan, a dermatologist at The Dermatology Clinic, said these therapies have become first- or second-line options for moderate to severe eczema, and an alternative for milder cases that do not respond to topical steroids.
Relief also comes faster: patients on JAK inhibitors can see improvement within days, biologics within weeks – compared to several months for immunosuppressants.
In clinical trials, about 44 to 51 per cent of adults treated with Dupixent alone achieved a 75 per cent improvement in eczema severity at 16 weeks, according to the manufacturer.
“Socioeconomically, it can have a huge impact on a young adult … just treating the skin gives them so much more confidence,” said Dr Uma.
HIGH COST OF TREATMENT
The price, however, remains a steep barrier.
A single Dupixent jab costs Mr Reyes Lim over S$900. The 19-year-old's eczema worsened when he was 16, and after finding no relief from Western or traditional Chinese medicine, he started Dupixent in January.
“It really feels like hope shining down on you ... A stop from all the doctors, all the medications," said the polytechnic student, who takes the jab every two weeks.
The itch on his scalp stopped almost immediately and his sleep improved, though his skin has not fully healed.
“I'm quite happy with the treatment so far. The only thing that I cannot take is the price.”
One in 10 adults in Singapore suffer from atopic dermatitis, the most common form of eczema in the country. In line with World Atopic Dermatitis Day on Tuesday (Sep 14), Cheryl Goh looks at one patient’s struggle with the condition.
JAK inhibitors are similarly expensive, ranging from S$500 to about S$2,000 a month, said Clinical Associate Professor Mark Koh, head and senior consultant at KK Women's and Children's Hospital's (KKH) dermatology department.
Of the targeted therapies, only one – abrocitinib (Cibinqo), a JAK inhibitor – is subsidised under the Ministry of Health's Medication Assistance Fund, after being added to the list in March 2024. Singaporeans can qualify for up to 75 per cent off, depending on their household income, bringing higher-dose pills to between S$300 and S$900 a month.
Why do these drugs cost so much? Drug patents last about 20 years, granting manufacturers a monopoly that eliminates competition. For biologics specifically, the manufacturing process – biological rather than chemical – is costlier and harder to reproduce, said Dr Yew.
Dupixent is subsidised in parts of Europe, Canada and Australia, but not in Singapore. In November 2024, then-Senior Minister of State for Health Dr Janil Puthucheary said in parliament that Dupixent was not recommended for subsidy as its benefits did not justify its cost at the price proposed by the manufacturer.
Cibinqo, an oral medication, was assessed as at least as effective and available at a lower price, he said.
“If patients face issues affording dupilumab, they may approach medical social workers at our public healthcare institutions to apply for financial assistance through MediFund,” Dr Janil said.
However, JAK inhibitors like Cibinqo may not be suitable for all patients – those who are older or have more comorbidities may not be recommended the drug due to its lower safety profile, Dr Uma said.
For children aged below 12, only Dupixent and baricitinib (Olumiant) are approved in Singapore.
Mr Quek, 43, who declined to give his full name, secured a 75 per cent Dupixent subsidy for his primary school-aged son through a medical social worker. The improvement was immediate.
“Ever since the injection, the skin started healing, his sleep is a lot better. And because he's sleeping better, school-wise is better – he pays attention, has more energy. He's growing better,” said the educator.
His son is also no longer as self-conscious about his skin. While he used to insist on wearing long sleeves and long pants, he’s now happy to wear T-shirts and shorts, he added.
But the subsidy lasted only 20 weeks. “We can see that there are times the eczema is coming back, and then we may have to visit this S$900 jab in the future,” said Mr Quek.
KKH's Dr Koh, who sees mostly paediatric cases, said better access to newer treatments will help, given the condition's broader impact.
“Having a good sleep at night is everyone's right, especially children. And eczema, although it's just on the skin … it's a systemic disease,” said Dr Koh.
Patients may not grow well, or may not want to go to school or socialise, he added.
MANAGING A CHRONIC DISEASE
Dr Yew stressed that these treatments are not a cure – they buy patients time for their skin to heal.
“We tell our patients that all these agents are not meant to cure them. It's meant to control their condition so that their skin has a chance to heal, and when the skin heals, they no longer need these agents,” he said.
Patients typically try them for about a year before weaning off.
The treatments also address only one aspect of eczema, which is to reduce inflammation. Managing the condition still requires moisturising, trigger avoidance, itch control and treating skin infections.
“They should not view all these agents as the final solution to everything. At the end of the day, you really need a combination approach,” he said.
For now, these treatments remain out of reach for many who need them. Ms Ursula Soh, 35, who started an eczema support group on Facebook, said members often ask about biologics and JAK inhibitors but often get no response – because only a small fraction of people can afford to try them, she said.
“From what I've heard so far, those people who are privileged enough to afford it, they say it's good. It changed their lives,” she said.
“Whether long-term or short-term, I can't answer that. But I think every bit counts if you have a few years of relief to just focus on your life.”