Commentary: Post-COVID psychosis is a rare but frightening condition
For a small number of people, a COVID-19 infection may be accompanied by days or weeks of paranoid delusions and hallucinations, says this researcher.

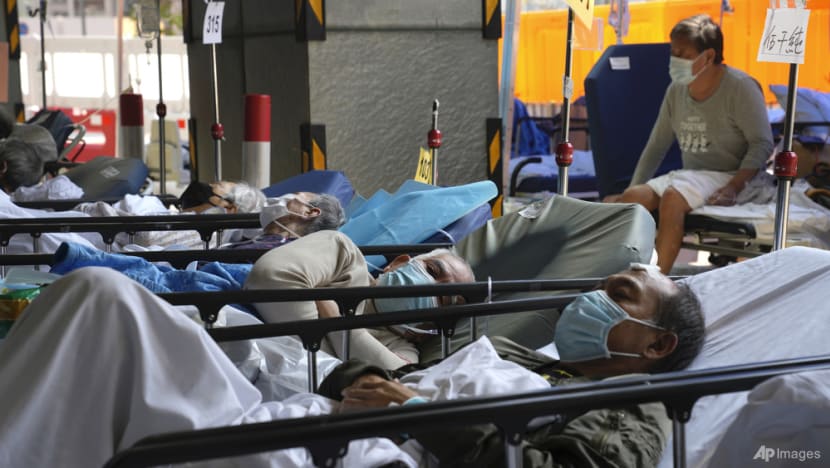
There was a decrease in suicide deaths across all age groups for the first time in 2023. (File photo: iStock)
PERTH: Far from the respiratory disease it seemed at first, COVID-19 can impact almost all parts of the body, including the brain. For a small number of people, COVID-19 infection may be accompanied by an episode of post-COVID psychosis, a break from reality which can be frightening for the patient and their loved ones.
Psychosis is a condition characterised by confused thoughts, delusions and hallucinations. People with psychosis can struggle to tell what’s real from what isn’t. Psychosis occurs in “episodes” which may last for days or weeks. Since the start of the COVID-19 pandemic, reports of post-COVID psychosis have come from all over the world.
Post-COVID psychosis is different to psychosis seen in other brain illnesses and diseases. So-called “first episode psychosis” is usually seen in teens or young adults in the development of schizophrenia, or alongside dementia in elderly people.
But people experiencing post-COVID psychosis are typically in their 30s, 40s and 50s, and are experiencing psychosis for the first time. They usually do not have any family history of psychosis.
People with post-COVID psychosis also frequently have insight into the way they are feeling. They can recognise this is not normal for them, and something has changed in the way they are thinking.
DELUSIONS WEEKS OR MONTHS AFTER INFECTION
Based on the small number of reports so far, the start of psychosis has been days, weeks or even months after COVID-19 diagnosis.
While the symptoms of post-COVID psychosis can be varied, there are some commonalities: People usually have problems sleeping, followed by paranoid delusions and hallucinations. Some people feel compelled to hurt themselves or others.
The scientific evidence of post-COVID psychosis comes mostly from “case reports”, which are research papers describing symptoms and recovery of individual patients.
In the first and most widely reported case, a 36-year-old American woman developed psychosis approximately four days after she started having mild COVID-19 symptoms. She became delusional, thinking that her partner was trying to kidnap her children.
She was convinced she was being tracked through her mobile phone. After trying to pass her children through a fast-food restaurant drive-through serving counter to protect them, she was taken to hospital for care. After one week of in-patient care to treat her psychosis, she was discharged. Her delusions did not return.
In another case, a 43-year-old Bulgarian man began experiencing psychosis two days after he was discharged from hospital for severe COVID-19. He believed the doctors had faked the results saying his COVID-19 illness had resolved.
He also had delusions that he had already died and his organs were rotten. He became a danger to his family, believing he should kill them to “spare them the same slow suffering”. After two weeks of treatment in hospital, his psychotic symptoms resolved and did not return.
Other case studies have reported people having delusions that patients in the hospital were actors and medical staff were trying to harm them, hearing voices speaking in foreign languages or telling them to take on grand tasks, like saving the earth.
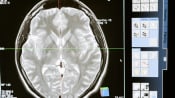
CHANGES IN THE BRAIN
The cause of post-COVID psychosis is not well understood. Some scientists think it could be due to persistent inflammation in the brain, prolonged inflammatory signals in the body or due to changes in blood vessels in the brain.
There is new evidence that brain areas undergoing change in mild COVID-19 infection may also be areas that change in people who are at risk of, or who are experiencing, first-episode psychosis (that is, not after COVID-19 infection).
These areas are the orbitofrontal cortex at the front of the brain, and the parahippocampal gyrus - a key memory region deep in the brain. These regions may shrink in both mild COVID-19 and psychosis. However, more research is needed to understand this link.
RARE BUT FRIGHTENING COMPLICATION
COVID-19 is not the first virus to be linked to psychosis. During the “Spanish flu” influenza pandemic of 1918 there were reports of post-viral psychosis.
Psychosis has been reported after infections with the other human coronaviruses, like those that cause Severe Acute Respiratory Syndrome (SARS) and Middle East Respiratory Syndrome (MERS). Links between coronaviruses, immune system activation and psychosis have also been found, suggesting COVID-19 may not be the only coronavirus capable of causing psychosis.
Just how common is post-COVID psychosis? The evidence to date suggests it is rare, occurring in about 0.25 per cent of COVID-19 cases who are not hospitalised (and likely have a mild infection), and 0.89 per cent of people who are hospitalised for COVID-19.
Because there have been so many cases of COVID-19 worldwide, isolated reports of post-COVID psychosis may stand out more. The frightening nature of what people might experience means we might hear more and more about them on social media and in the news.
Although the risk of post-COVID psychosis is low, people who have had COVID-19 and their families should look out for any sudden changes in personality, paranoia or delusions in the days, weeks and months following infection.
If these signs are noticed, seeking medical help is vital. Most cases of post-COVID psychosis resolve quickly with proper psychiatric care and treatment with medication.
Sarah Hellewell is Research Fellow in Faculty of Health Sciences and The Perron Institute for Neurological and Translational Science, Curtin University. This commentary first appeared on The Conversation.