Heart of the Matter: Recent changes to cancer drug list have lowered costs substantially, say experts
Changes to an approved cancer drug list last September have helped more patients get wider coverage for their treatment. While it may have been a significant improvement in out-of-pocket expenses for many people, is the cost of treating cancer in Singapore still too high? This episode of the Heart of the Matter podcast gets answers.
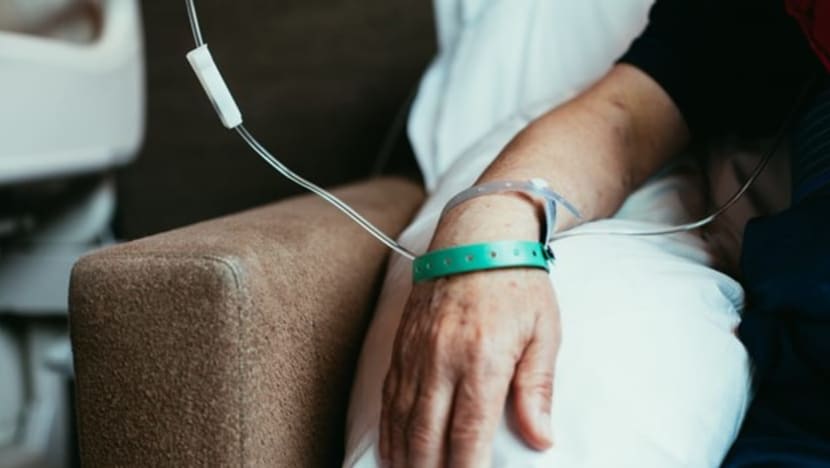
Patient getting cancer treatment. (File photo: iStock/agrobacter)
SINGAPORE: When Gina Ho was told that she had early signs of thyroid cancer, the 43-year-old mother of three teenagers remembered being “struck with fear”.
“I remember crying so much at the MRT station when I received the news, instead of going to (see) a doctor straight (away),” said Ms Ho.
Among her many worries was the fear that she may not be able to afford the necessary cancer drugs and treatment, especially if she needed long-term care.
While Ms Ho did qualify for medical care in a private hospital under her insurance plan, she told host Steven Chia on the Heart of the Matter podcast that she was also concerned she may have to end private treatment if she lost her job.
Joining them on the podcast were Associate Professor Ravindran Kanesvaran, chairperson of the Cancer Treatment Fund Committee and Evelyn Goh, deputy CEO and chief advisory officer of Providend.
Dr Ravindran said it is not unusual for cancer patients he sees to go through the “whole gamut of emotional upheaval” before coming to terms with the disease.
“They go through such concerns about cost, about side effects, about survival. Mortality becomes something very real to them,” he added.
But Dr Ravindran noted that the government has negotiated prices with pharmaceutical companies to bring down the costs of cancer drugs substantially.
“You are talking about drug cost reduction from 30 to 60 percent, 65 per cent for some of the drugs,” said Dr Ravindran.
“With that savings, the government has now channeled the savings to fund drugs that they didn’t fund in the past,” he added.
In August 2021, the Ministry of Health announced changes to the MediShield Life, MediSave and Integrated Shield Plan coverage, as well as established a cancer drug list.
Under the changes, treatments that are in the cancer drug list are covered and the number of treatments has increased from 270 to 340 as of February this year. This covers about 90 per cent of all cancer treatments approved by the Health Sciences Authority.
INSURANCE IS ALL ABOUT WHAT YOU WANT
But ahead of these changes, some insurers were offering additional coverage for cancer treatment and services in the form of riders.
Deputy CEO of Providend Ms Goh noted that many patients with a rider have a “buffet syndrome” and often make claims on unnecessary procedures. In turn, insurance companies will charge a higher premium for these riders.
When asked if MediShield Life coverage is sufficient, Ms Goh said it depends on a person’s healthcare expectations.
Those who are satisfied with a C-class ward in a restructured hospital will not need extra coverage while others who prefer a more conducive environment and who may want to choose their doctor, will have to upgrade and buy more insurance.
After consulting with other cancer patients, Ms Ho shared that she chose not to go for the private option but to seek treatment at the National University Hospital instead, hoping to extend her financial coverage.
“Let's say, the insurance does cover for this occurrence of cancer, what if future treatments, I can't afford it anymore? So that has always been a nagging point for me. And that's why public health care was my first choice all along,” explained Ms Ho.
Here are other highlights from the conversation:
MAKING FINANCIAL DECISIONS AS IMPORTANT AS TREATING CANCER
Gina Ho: I already have a “p plus plan” from my insurance provider. So that will cater for me for private hospital. However, if I'm not able to have a secure income at the end of the day, if there are any financial challenges that come along the way, would I be able to afford private class? So that was definitely one key consideration that I had.
Evelyn Goh: (On whether MediShield Life is enough), it's really a function of what's your healthcare expectations. If you're happy going to C ward at a restructured hospital, no air-con, no TV, no shared bathrooms and all that, then that's fine.
But if you want something that is more conducive for yourself, you want to have air-con, you want to perhaps choose your doctor, then I would say you will need to upgrade. You have to buy additional insurance beyond MediShield Life.
LOWER COSTS SINCE NEW DRUG LIST ANNOUNCEMENT
Dr Ravindran Kanesvaran: Prior to Sep 1 last year, when the cancer drug list first came into the picture. There were many gaps, a lot of drugs did not get reimbursement from the government … After Sep 1, the government negotiated prices with pharmaceutical companies to bring down cancer drug costs substantially. You're talking about drug cost reduction from 30 to 60 per cent, 65 per cent for some of the drugs.
So with that savings, the government has now channelled the savings to fund drugs that they didn't fund in the past.
IS TREATING CANCER TOO COSTLY IN SINGAPORE?
Dr Ravindran: The cost of surgery in public hospitals, in general, is pretty much well controlled in terms of pricing. And it's relatively affordable, because the government controls pricing across all public hospitals.
You don't have to “hospital shop” to get the cheapest surgery somewhere, as a subsidised patient.
Dr Ravindran: If you're concerned, you're not sure about insurance coverage and you're willing to get C or B2 class treatment, you will get very reasonably priced treatment. Now, the elephant the room always has been the systemic therapy part because these drugs are controlled by pharmaceutical companies that sell these drugs to us.
Goh: (MediShield Life and Integrated Shield plans) actually can finance up to 90 per cent of the medical cost. And if people have a rider, this bill can be entirely paid by the plans that they have. But because of this kind of “buffet-as-charged" feature of such plans, the claims experience of the insurance companies has increased exponentially, that led on to big jumps in the premiums, which then led on to all these concerns about you know whether premiums can be sustainable over the long term, especially as one grows older.
For the full Heart of the Matter podcast conversation, listen to the episode.